Frequency by Location
Posterior segment (vitreous, retina): Accounts for 58–88% of all IOFBs. Most common.
Anterior segment (anterior chamber, iris, lens): 10–15%.
Lens and orbit: 2–8%.
An intraocular foreign body (IOFB) is a foreign object that penetrates the eye wall from outside and remains inside the eye. It is a form of open globe injury (OGI) and is an ophthalmic emergency that significantly affects visual prognosis. Metal fragments, glass shards, plastic pieces, wood chips, etc., enter the eye during hammering, grinding, drilling, using automatic lawn mowers, explosions, or traffic accidents, often in factories or workplaces. Most are small metallic foreign bodies entering through the corneoscleral junction. The time to removal greatly influences visual prognosis, so early diagnosis and prompt removal are essential.
The incidence of OGI in the United States is 4.5 per 100,000 per year, and IOFB accounts for 18–41% of OGI 1). Globally, the number of IOFB cases per million population increased from 350 in 2008 to over 450 in 2019 1). The most common patient group is men aged 21–40, with injuries occurring at work in 54–72% and at home in about 30% of cases 1). It is common among workers in metal manufacturing, processing, and construction, with metal fragments (iron, copper, lead, etc.) accounting for the majority.
The Zone of Injury classification is used for severity grading based on the injured site1).
Frequency by Location
Posterior segment (vitreous, retina): Accounts for 58–88% of all IOFBs. Most common.
Anterior segment (anterior chamber, iris, lens): 10–15%.
Lens and orbit: 2–8%.
Types of Material
Metals: Iron, copper, lead, zinc, aluminum, nickel, etc. Most common.
Non-metals: Glass, plastic, stone, wood, plant matter, etc.
Organic materials: Wood, fiber, plant matter. Strong tissue reaction and high risk of endophthalmitis.
Intraocular foreign bodies are classified into the following five types based on their location.
A small iron particle may not be noticed at the time of injury. However, if left untreated, siderosis can gradually reduce vision. If you experience floaters or vision changes after metalworking, you should promptly see an ophthalmologist.
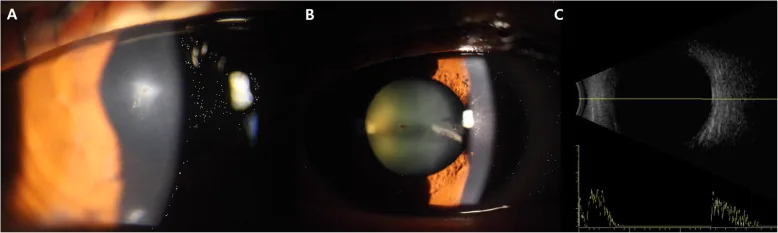
Note that with very small foreign bodies like iron filings, the patient may be unaware of the injury. Symptoms include eye pain, tearing, and visual impairment. If a corneal perforation is present with leakage, hypotony and shallow anterior chamber often occur.
Clinical findings of open globe injury are diverse. If globe rupture is suspected, avoid using applanation tonometry for intraocular pressure measurement 1). Up to 55% of IOFBs are undetectable by clinical examination alone, so imaging is essential 1).
Even if vision is preserved, a foreign body may remain inside the eye. Particularly, iron filings or copper fragments can cause siderosis or chalcosis if left untreated, leading to vision loss months to years later. It is important to visit an ophthalmologist immediately after injury and undergo CT to rule out IOFB.
The most common mechanism of IOFB is hammering metal (59%) 5). Other main mechanisms are listed below.
The overall rate of endophthalmitis complicating IOFB is 5–30% (average 6.5%) 1). Rural areas, organic foreign bodies, and delayed treatment increase the risk.
The effect on tissue varies greatly depending on the material of the foreign body.
| Material | Toxicity | Main Complications |
|---|---|---|
| Iron/Steel | Moderate | Siderosis (chronic) |
| Copper (pure copper) | High | Chalcosis / Panophthalmitis |
| Glass/Plastic | Low (inert) | May be left in place |
When using a grinder or hammer, there is a risk of intraocular foreign body from flying metal fragments. Always wear protective eyewear (goggle type preferred) that meets ANSI or JIS standards. 54–72% of IOFBs occur in the workplace, and most can be prevented with appropriate protective equipment1).
Imaging is essential for localizing intraocular foreign bodies. It is important to determine whether the foreign body is magnetic (iron) or non-magnetic (copper, aluminum, lead, zinc, glass, wood), and a detailed history of the injury should be obtained. The characteristics of each modality are described below.
| Test | Detection sensitivity | Notes |
|---|---|---|
| CT | Up to 95% | First choice. Effective for metal, glass, and stone |
| X-ray (Waters view) | Metal fragments ≥2 mm | Low sensitivity. Screening only |
| MRI | — | Absolute contraindication for metallic IOFB |
Regardless of the location of the foreign body, consider the possibility of infection and perform bacterial and fungal culture of intraocular fluid.
OTS is a prognostic score that predicts final visual acuity based on initial visual acuity at the time of injury, presence of globe rupture, endophthalmitis, perforation, retinal detachment, and RAPD 1). It is used to guide treatment decisions and patient counseling.
If a metallic IOFB is suspected, do not undergo MRI. Magnetic foreign bodies can move in the MRI magnetic field, causing additional intraocular damage 1). First, evaluate the presence and material of the foreign body with CT; consider MRI only if non-metallic nature is confirmed.
Recommended systemic antibiotic regimen1):
Open globe injuries should undergo primary closure first. Suture material guidelines are as follows1).
Primary repair within 24 hours of injury is an independent protective factor against endophthalmitis1)7).
Once an intraocular foreign body is confirmed, prompt removal as soon as possible leads to better visual prognosis in terms of both tissue reconstruction and infection control.
Anterior Segment Foreign Body
Removal method: After maintaining the anterior chamber with viscoelastic material, remove with forceps through a corneoscleral incision.
Magnetic foreign body: An external magnet can also be used for small iron fragments in the anterior segment.
Indications: IOFB in the anterior chamber, iris, or lens.
Posterior Segment Foreign Body
Standard procedure: Small-incision pars plana vitrectomy (PPV) using 23G/25G/27G is standard1).
Large foreign body (>4 mm): Removed via a corneoscleral tunnel incision1).
Use of PFCL: Macular protection with liquid perfluorocarbon (PFCL) is controversial1).
Anterior chamber, angle, and iris foreign bodies: Create a sufficiently wide corneoscleral incision, inject enough viscoelastic into the anterior chamber to maintain space, and ensure the foreign body does not move. Then remove it with forceps, taking care not to damage the corneal endothelium or lens.
Intralenticular foreign body: Inject sufficient viscoelastic into the anterior chamber, then remove the foreign body with a magnet or forceps. If the posterior capsule is intact, proceed with standard cataract surgery and intraocular lens implantation. If the posterior capsule is damaged, perform vitrectomy.
Vitreoretinal foreign body: For large magnetic foreign bodies with a large corneal perforation, removal with a giant magnet is possible. Generally, vitrectomy is performed using an intraocular magnet, microforceps, or diamond forceps, creating a wound at the limbus or pars plana corresponding to the size of the foreign body.
Choroidal/scleral foreign body: Similar to scleral buckling, visualize the fundus, perform a partial-thickness scleral incision over the foreign body, remove it with a magnet or forceps, and then perform cryocoagulation.
Intravitreal administration is performed according to the risk of endophthalmitis. Recommended drugs and doses are shown below 1). Antibiotics are also added to the vitrectomy perfusion fluid in accordance with vitrectomy for bacterial endophthalmitis.
| Drug | Dose | Indication |
|---|---|---|
| Vancomycin | 1.0 mg/0.1 mL | Gram-positive coverage |
| Ceftazidime | 2.25 mg/0.1 mL | Gram-negative coverage |
| Voriconazole | 50–100 μg/0.1 mL | Rural areas/soil contamination cases (fungal risk) 1)3) |
The urgency varies depending on the material of the foreign body 1).
For large perforations of the posterior sclera, a three-layer plug (filled from the inside) using donor sclera, amniotic membrane, and fibrin glue has been reported to be effective4).
Primary repair of open globe injuries is recommended within 24 hours. Repair within 24 hours has been reported as an independent protective factor against endophthalmitis1)7). Toxic metals (iron, copper) and organic foreign bodies should be removed immediately in principle, while inert foreign bodies such as glass may sometimes be managed electively.
It depends on the material. Toxic metals such as iron and copper, and organic materials are generally removed due to the risk of tissue damage and endophthalmitis. Inert foreign bodies such as glass or plastic may be left in place if the risk of removal complications is high1). Individual assessment by an ophthalmologist is necessary.
When a ferrous foreign body remains in the eye, iron ionizes into ferrous and ferric forms, diffuses throughout the eye, and accumulates in various tissues2).
The toxicity of copper foreign bodies depends on the purity of the copper. Copper has an affinity for basement membranes such as the internal limiting membrane.
Plant fragments, wood chips, cotton fibers, etc., cause severe granulomatous tissue reaction and endophthalmitis1). In principle, immediate removal is necessary. However, cotton fibers that have strayed after intravitreal injection are relatively inert and may not require removal6).
When a foreign body is completely embedded in the choroid, removal may be technically impossible 5). If long-term inflammation persists, enucleation of the eye may be necessary.
Postoperatively, there is a possibility of progression to proliferative vitreoretinopathy (PVR). If the uvea is severely damaged, sympathetic ophthalmia may develop. Maximum attention must also be paid to endophthalmitis.
Zhao et al. (2025) reported a novel magnetic foreign body extractor (JIN magnetic foreign body extractor) using a rare earth-gold alloy 2). It is compatible with 20–27G ports and allows foot pedal-controlled on/off switching of magnetic force ranging from 254 to 86.3 Gauss-seconds (Gs). The importance of early removal to prevent retinal pigment epithelial toxicity due to iron ion release is also emphasized 2).
Celo et al. (2023) reported a technique for internal closure of posterior perforations using a three-layer plug combining donor sclera, amniotic membrane, and fibrin glue 4). This is noted as an alternative procedure for posterior perforations where conventional external suturing is difficult.
Mishra et al. (2023) performed simultaneous bilateral vitrectomy by two surgeons in two cases of bilateral open globe trauma caused by explosives 3). This reduced general anesthesia time compared to sequential surgery by a single surgeon and is considered a useful option in managing bilateral ocular trauma.
McMaster et al. (2025) published a systematic review and meta-analysis of primary repair timing in open globe injuries 7). Repair within 24 hours is an independent protective factor against endophthalmitis, supporting the benefit of early repair as the latest evidence.
Drnovsek et al. (2022) reported a case of a cotton fiber that migrated into the vitreous cavity after intravitreal injection 6). Cotton fibers are relatively inert, and observation or endoscopic removal should be considered. Awareness of iatrogenic IOFB is increasing.
Reports indicate that 15% of pediatric patients develop GAD, PTSD, or depression after trauma, highlighting the importance of psychological support alongside ophthalmic treatment 1).