
Ophthalmic Complications of Corticosteroids
1. What are the ophthalmic complications of corticosteroids?
Section titled “1. What are the ophthalmic complications of corticosteroids?”Corticosteroids (glucocorticoids) are essential drugs for treating a wide range of diseases, including autoimmune diseases, inflammatory eye diseases, and postoperative inflammation. However, long-term or high-dose use can cause serious ocular side effects.
The most common drug-induced lens opacity is steroid cataract, which, once developed, can cause severe visual impairment in a relatively short period. It often occurs with systemic administration, but can also develop with long-term inhalation therapy or eye drops. Patients receiving steroids require regular ophthalmic examinations.
The main diseases and conditions in which steroids are used in ophthalmology are as follows.
- Allergic/hypersensitivity reactions: hay fever, vernal catarrh, allergic conjunctivitis
- Uveitis (anterior, posterior, panuveitis): recurrence prevention and inflammation control
- Scleritis/episcleritis: autoimmune inflammation
- Giant cell arteritis: emergency systemic administration to protect vision
- Postoperative inflammation management: after cataract surgery or corneal transplantation
- Herpetic eye disease: Inflammation of stromal keratitis (used in combination with antiviral drugs)
- Orbital diseases: Thyroid eye disease, orbital inflammatory pseudotumor
Short-term use rarely causes ocular complications, but increased intraocular pressure can appear about 2 weeks after starting treatment. Cataracts usually occur with long-term use, but in steroid responders, intraocular pressure can rise even with short-term use, so regular intraocular pressure measurement is recommended regardless of treatment duration.
2. Main symptoms and clinical findings
Section titled “2. Main symptoms and clinical findings”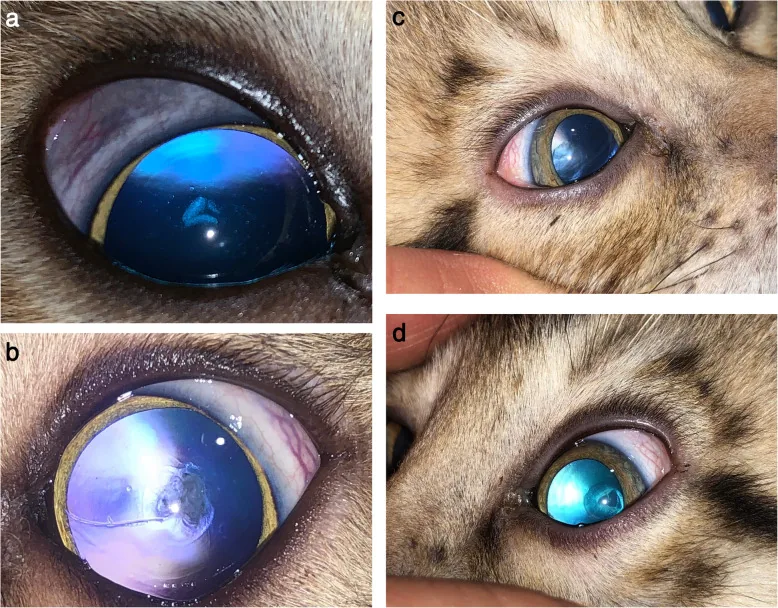
Subjective symptoms
Section titled “Subjective symptoms”Posterior subcapsular cataract (steroid cataract):
- Decreased visual acuity (significant when opacity reaches 3 mm or more in diameter)
- Photophobia and glare (sensitivity to light sources, brightness)
- Marked reduction in contrast sensitivity despite good visual acuity
- Visual dysfunction is often noticed even when the opacity is small
Steroid glaucoma:
- Often asymptomatic (difficult to notice even with high intraocular pressure)
- High intraocular pressure may cause eye heaviness, discomfort, or blurred vision
- Visual field defects (peripheral vision loss as it progresses)
Stages of Opacity Progression
Section titled “Stages of Opacity Progression”| Stage | Findings |
|---|---|
| Early | Faint punctate opacities or vacuoles directly beneath the posterior capsule on the visual axis |
| Advanced | Punctate opacities coalesce into a well-demarcated, homogeneous, disc-shaped posterior subcapsular opacity (2–3 mm in diameter). Polychromatic granules in blue, green, and red. |
| Further progression | Extends into the anterior cortex. It takes time to expand beyond the boundary line. |
| Late stage | Increased backward scattering intensity in the embryonic nucleus → Complicated nuclear cataract |
Steroid cataract is generally recognized as posterior subcapsular cataract, but the risk of nuclear cataract is also high, and co-occurrence is not rare. PSC progresses faster than other cataract types, and three large studies have shown that PSC progresses more rapidly than nuclear or cortical cataracts 3).
Findings of steroid glaucoma:
- Open angle (no angle abnormalities)
- Elevated intraocular pressure (often 30 mmHg or higher)
- Accumulation of extracellular matrix in the trabecular meshwork
- In long-standing cases, optic disc cupping and thinning of the retinal nerve fiber layer
| Complications | Typical opacity/findings | Early symptoms |
|---|---|---|
| Steroid cataract | Posterior subcapsular disc-shaped opacity (4-stage progression) | Glare and photophobia |
| Steroid glaucoma | Optic disc cupping enlargement | Almost asymptomatic |
Typical steroid cataract presents as a disc-shaped opacity in the posterior subcapsular region on the visual axis, often accompanied by polychromatic granules. Although age-related cataract can also cause posterior subcapsular opacity, if posterior subcapsular cataract is observed in a patient under 40 years of age, a history of steroid use should be actively investigated. Differentiation from complicated cataract due to uveitis may sometimes be difficult.
3. Causes and Risk Factors
Section titled “3. Causes and Risk Factors”Risk by Route of Administration
Section titled “Risk by Route of Administration”The risk of ophthalmic complications from steroids varies by route of administration. Systemic administration carries the highest risk, but long-term topical use can also lead to development 1).
- Systemic administration (oral/intravenous): Highest risk for both cataract and glaucoma. Onset is relatively rare at prednisolone-equivalent doses below 10 mg/day. It often occurs in cases of long-term high-dose systemic administration over one year.
- Steroid eye drops: Lower risk than systemic administration, but long-term use can cause posterior subcapsular cataract and increased intraocular pressure3)
- Inhaled steroids (asthma treatment): Risk of posterior subcapsular cataract8)
- Intranasal steroids: Systematic reviews indicate no significant risk of cataract or increased intraocular pressure9)
- Intravitreal triamcinolone injection: Increased intraocular pressure occurs in over 50% of cases, with 1–2% requiring surgical intervention2)
Risk Factors for Cataract
Section titled “Risk Factors for Cataract”The AAO Cataract Preferred Practice Pattern states that systemic steroid use is a risk factor for posterior subcapsular cataract, and long-term users of inhaled or oral corticosteroids have a higher risk of developing cataract3).
- Children are more susceptible to steroid-induced cataracts than adults
- Patients receiving long-term systemic treatment for systemic diseases (collagen disease, SLE, rheumatoid arthritis, nephrotic syndrome, post-renal transplant) are at particularly high risk
Risk factors for glaucoma
Section titled “Risk factors for glaucoma”- Pre-existing primary open-angle glaucoma
- History of increased intraocular pressure from previous steroid use (steroid responder)
- Type 1 diabetes
- Children and the elderly (high reactivity)
- Long-term use exceeding 3 months2)
4. Diagnosis and Examination Methods
Section titled “4. Diagnosis and Examination Methods”Diagnosis of Cataracts
Section titled “Diagnosis of Cataracts”Observation of the lens using a slit lamp microscope is fundamental.
- Observation points: Presence of saucer-shaped opacities and polychromatic granules directly under the posterior capsule, and the diameter of the opacity (≥2 mm indicates visual impairment).
- Retroillumination: Easy to confirm posterior subcapsular opacity and vacuoles
- Visual function evaluation: Even if corrected visual acuity is good, contrast sensitivity may be significantly reduced, and surgery may be indicated early
- LOCS III classification: Opacity is evaluated in four categories: nuclear (NO/NC), cortical (C), and posterior subcapsular (PSC). PSC evaluates the degree of posterior subcapsular opacity using retroillumination 4)
The most important aspect of diagnosis is detailed inquiry about steroid use history, including route of administration (systemic, eye drops, inhalation, nasal spray), dose, and duration. In uveitis patients using steroids, differentiation from uveitis-related complicated cataract may be difficult. History of radiation exposure and ocular trauma should also be confirmed as risk factors for posterior subcapsular cataract 3).
Diagnosis of Glaucoma
Section titled “Diagnosis of Glaucoma”- Intraocular pressure measurement: Goldmann applanation tonometry is the standard
- Gonioscopy: Assessment of open angle or angle abnormalities
- Visual field test: Evaluation of visual field defects using Humphrey static perimetry
- Optic nerve evaluation: Assessment of optic disc morphology and retinal nerve fiber layer using OCT
Visual acuity measures the ability to distinguish high-contrast (sharp black-and-white) targets, whereas contrast sensitivity is the ability to distinguish subtle differences in brightness. In posterior subcapsular cataract, contrast sensitivity often decreases markedly even when visual acuity is relatively good, causing difficulties in daily life (e.g., walking or driving in dim light). If contrast sensitivity is significantly reduced, surgery may be indicated even with good visual acuity.
5. Standard Treatment
Section titled “5. Standard Treatment”Treatment of Steroid-Induced Cataract
Section titled “Treatment of Steroid-Induced Cataract”Conservative management:
- Medical treatment for cataract lacks sufficient evidence of efficacy and is not recommended3)
- For small central opacities, temporary visual improvement with mydriatic agents is possible, but caution is needed for worsening glare
- Consider reducing or discontinuing steroids to the minimum effective dose (while balancing management of the underlying disease)
Surgical indications:
- Surgery is often necessary when the diameter of posterior subcapsular opacity is 2 mm or more and visual function is impaired.
- If contrast sensitivity is markedly reduced, surgery may be considered even if visual acuity is good.
- Since PSC progresses rapidly, early surgery is often required.
Surgical method:
- Phacoemulsification + IOL insertion is the main approach.
- Intraoperative caution (important): In eyes with posterior subcapsular opacity, the posterior capsule may be fragile, so care must be taken to avoid posterior capsule rupture.
- In cases with underlying uveitis, surgery is performed while continuing oral steroids during a relatively stable period. IOL insertion is not problematic.
- If filtration surgery for secondary glaucoma may be necessary, preserve the superior conjunctiva and perform surgery via a corneal incision.
Postoperative management:
- Control of inflammation of the underlying disease (e.g., uveitis) is important.
- The risk of posterior capsule opacification (PCO) is high during continued steroid administration.
Treatment of steroid-induced glaucoma
Section titled “Treatment of steroid-induced glaucoma”First-line: Reduce or discontinue steroids
- If possible, prioritize reducing or discontinuing steroids. However, reduction may be difficult due to management of the underlying disease.
- Tissue changes may be irreversible, so early intervention is important.
Intraocular pressure-lowering therapy (similar to primary open-angle glaucoma):
- Use in order: prostaglandin analogs, beta-blockers, carbonic anhydrase inhibitors (eye drops or oral), alpha-2 receptor agonists.
- If intraocular pressure is not controlled with eye drops or oral medication, surgery may be necessary2)
Surgical treatment:
- Trabeculotomy: This is an option for steroid-induced glaucoma when intraocular pressure cannot be adequately controlled with medication. Multicenter studies have reported its effectiveness in controlling intraocular pressure in eyes with steroid-induced glaucoma13)
- Selective laser trabeculoplasty: It is likely to be effective, but should not be performed in cases complicated by uveitis
- Trabeculectomy (filtering surgery): Performed when trabeculotomy is insufficient
In many cases, discontinuing or reducing steroids lowers intraocular pressure. However, if long-term use has caused irreversible trabecular meshwork changes (accumulation of extracellular matrix), intraocular pressure may not improve even after discontinuation, and pressure-lowering medications or surgery may be needed. If discontinuation is difficult due to the underlying disease, the ophthalmologist and primary care physician should collaborate on management.
Surgery itself can be expected to have good outcomes similar to routine cataract surgery. However, if steroids are continued, the risk of posterior capsule opacification (PCO) is high, and regular follow-up is necessary after surgery. PCO can be treated with Nd:YAG laser posterior capsulotomy. Since the posterior capsule may be fragile, surgical techniques that avoid intraoperative posterior capsule rupture are required.
6. Pathophysiology and Detailed Mechanisms
Section titled “6. Pathophysiology and Detailed Mechanisms”Mechanisms of Steroid-Induced Cataract
Section titled “Mechanisms of Steroid-Induced Cataract”The exact mechanism of steroid-induced cataract is not fully understood, but several mechanisms have been reported5)6)10).
- Schiff base intermediate formation theory: A Schiff base is formed between the C-20 ketone group of steroids and nucleophilic groups of lens proteins. Subsequently, a Heyns rearrangement of the C-21 hydroxy group occurs, producing a stable amine-substituted adduct. This adduct is reportedly observed only in steroid-induced cataracts5)
- Metabolic and membrane dysfunction: Impaired ion transport in lens epithelial cells
- Oxidative damage: Lens protein denaturation (crystallin aggregation) due to free radical production
- Mechanism via glucocorticoid receptor: Glucocorticoid receptors affect over 5,000 genes and cause abnormalities in cell adhesion molecules10)
- Formation of protein adducts
- Decreased transparency of posterior lens fiber cells and crystallin aggregation
- Migration of damaged lens equatorial cells to the posterior capsule side6)
Posterior subcapsular cataract occurs on the visual axis, causing visual dysfunction relatively early. If the opacity diameter is 1 mm or more, it affects visual function; at 2 mm or more, contrast sensitivity markedly decreases even with good corrected visual acuity; at 3 mm or more, visual acuity often decreases.
Mechanism of steroid glaucoma
Section titled “Mechanism of steroid glaucoma”Glucocorticoids increase intraocular pressure by reducing aqueous humor outflow from the anterior chamber.
- Increased extracellular matrix production in trabecular meshwork cells: Steroids inhibit the degradation and promote deposition of extracellular matrix (such as fibronectin, laminin, and collagen) in trabecular meshwork cells. This obstructs the trabecular meshwork structure and impairs aqueous humor outflow.
- Myocilin induction: Myocilin is a 55 kDa protein induced in trabecular meshwork cells upon exposure to steroids, and it is involved in reduced aqueous humor outflow and steroid-induced intraocular pressure elevation2).
- Cytoskeletal changes: Rearrangement of the actin cytoskeleton causes morphological changes in the aqueous humor outflow pathway.
There are individual differences in the intraocular pressure response to steroids. In young patients, those with high intraocular pressure, or those with severe optic nerve damage, surgery may be required11). In steroid responders, regular intraocular pressure monitoring is necessary regardless of the route or duration of administration12).
Mechanism of increased infection risk
Section titled “Mechanism of increased infection risk”Glucocorticoid receptors suppress the transcription of cytokines and chemokines, inhibiting the migration and activation of immune cells. This reduces local immunity against fungi, viruses, and bacteria. In particular, fungal infections are more likely to worsen under steroid-induced immunosuppression7).
7. Latest Research and Future Prospects
Section titled “7. Latest Research and Future Prospects”Ocular Safety of Intranasal Steroids
Section titled “Ocular Safety of Intranasal Steroids”Recent systematic reviews have shown that intranasal steroids are not significantly associated with the risk of cataracts or increased intraocular pressure9). However, even steroids considered to have low intraocular penetration, such as fluorometholone and loteprednol, have been noted to carry risks of increased intraocular pressure and cataracts with long-term use, requiring caution.
Fluocinolone Acetonide Sustained-Release Implant
Section titled “Fluocinolone Acetonide Sustained-Release Implant”Research on intravitreal fluocinolone acetonide sustained-release devices is advancing, suggesting potential utility in the long-term management of uveitis2). However, local side effects (increased intraocular pressure, cataracts) are more likely compared to systemic steroids, necessitating individualized management.
Genetic Identification of Steroid Responders
Section titled “Genetic Identification of Steroid Responders”Intraocular pressure response to steroids is thought to be genetically determined, and identification of related genes such as the myocilin gene is progressing. In the future, personalized medicine that uses genetic information to identify individuals at high risk for steroid-induced glaucoma in advance is expected to be realized12).
Yes, regular ophthalmology visits are strongly recommended. Elevated intraocular pressure often has few subjective symptoms, and cataracts are often asymptomatic in the early stages. Regardless of the route of administration (systemic, eye drops, inhalation), patients on long-term use require ophthalmic evaluation (intraocular pressure, lens, optic nerve) at least once or twice a year. In particular, checking intraocular pressure at 2 weeks to 1 month after starting treatment is important.
8. References
Section titled “8. References”-
McGhee CNJ, Dean S, Danesh-Meyer H. Locally administered ocular corticosteroids: benefits and risks. Drug Saf. 2002;25(1):33-55. PMID: 11820911. doi:10.2165/00002018-200225010-00004.
-
Okoye O, Okonkwo O. Inflammatory glaucoma. Community Eye Health. 2019;32(106):S1-S4.
-
Miller KM, Oetting TA, Tweeten JP, et al. Cataract in the Adult Eye Preferred Practice Pattern. Ophthalmology. 2022;129(1):P1-P126.
-
Chylack LT Jr, Wolfe JK, Singer DM, et al. The Lens Opacities Classification System III. Arch Ophthalmol. 1993;111(6):831-836. PMID: 8512486. doi:10.1001/archopht.1993.01090060119035.
-
Urban RC Jr, Cotlier E. Corticosteroid-induced cataracts. Surv Ophthalmol. 1986;31(2):102-110. PMID: 3541262. doi:10.1016/0039-6257(86)90077-9.
-
Jobling AI, Augusteyn RC. What causes steroid cataracts? A review of steroid-induced posterior subcapsular cataracts. Clin Exp Optom. 2002;85(2):61-75. PMID: 11952401. doi:10.1111/j.1444-0938.2002.tb03011.x.
-
Carnahan MC, Goldstein DA. Ocular complications of topical, peri-ocular, and systemic corticosteroids. Curr Opin Ophthalmol. 2000;11(6):478-483. PMID: 11141645.
-
Cumming RG, Mitchell P, Leeder SR. Use of inhaled corticosteroids and the risk of cataracts. N Engl J Med. 1997;337(1):8-14. PMID: 9203425. doi:10.1056/NEJM199707033370102.
-
Valenzuela CV, Liu JC, Vila PM, et al. Intranasal corticosteroids do not lead to ocular changes: a systematic review and meta-analysis. Laryngoscope. 2019;129(1):6-12. PMID: 30229924. PMCID: PMC6320292. doi:10.1002/lary.27209.
-
James ER. The etiology of steroid cataract. J Ocul Pharmacol Ther. 2007;23(5):403-420. PMID: 17900234. doi:10.1089/jop.2006.0067.
-
Sihota R, Konkal VL, Dada T, Agarwal HC, Singh R. Prospective, long-term evaluation of steroid-induced glaucoma. Eye (Lond). 2008;22(1):26-30. PMID: 16823461. doi:10.1038/sj.eye.6702474.
-
Phulke S, Kaushik S, Kaur S, Pandav SS. Steroid-induced glaucoma: an avoidable irreversible blindness. J Curr Glaucoma Pract. 2017;11(2):67-72. PMID: 28924342. PMCID: PMC5577123. doi:10.5005/jp-journals-10028-1226.
-
Japanese Steroid-Induced Glaucoma Multicenter Study Group. Success rates of trabeculotomy for steroid-induced glaucoma: a comparative, multicenter, retrospective cohort study. Am J Ophthalmol. 2011;151(6):1047-1056.e1. doi:10.1016/j.ajo.2010.11.028.
