Keratoconjunctivitis Sicca
Schirmer test: ≤5 mm/5 min indicates decreased secretion.
BUT (tear break-up time): ≤5 seconds indicates unstable tear film.
Fluorescein staining: Punctate epithelial erosions on inferior cornea and conjunctiva.
Rheumatoid arthritis (RA) is a chronic inflammatory autoimmune disease primarily affecting the synovial membrane of joints. It presents with various systemic symptoms including the lungs, skin, and eyes, and is the most common collagen disease.
It commonly occurs in women aged 30–60 years, with a male-to-female ratio of approximately 1:3. The proportion of males increases in elderly-onset cases. The prevalence in Japan is estimated to be about 0.5–1% of the population (approximately 600,000 to 1.2 million people).
Approximately 25–30% of RA patients have some ocular symptoms 1). The frequency of ocular complications is related to the duration of RA, disease activity, and the presence of extra-articular symptoms 2).
Ocular complications associated with RA are classified into the following five types.
| Ocular Complication | Frequency | Main Features |
|---|---|---|
| Keratoconjunctivitis sicca (dry eye) | Most common | Often associated with Sjögren’s syndrome |
| Scleritis | Relatively common | Eye pain, deep congestion, necrotizing form possible |
| Episcleritis | Relatively common | Superficial inflammation, tendency to resolve spontaneously |
| Peripheral corneal ulcer | Relatively rare | Rapid corneal thinning and risk of perforation |
| Iridocyclitis | Rare | Anterior uveitis |
Malignant rheumatoid arthritis is a severe form accompanied by scleritis, pleuritis, interstitial pneumonia, pericarditis, myocarditis, multiple mononeuritis, mesenteric artery embolism, and fingertip ulcers, and has a poor prognosis.
Approximately 25–30% of patients have some ocular symptoms. The most common is dry eye (keratoconjunctivitis sicca), followed by scleritis and episcleritis. Peripheral corneal ulcers and necrotizing scleritis are relatively rare but are serious complications directly linked to visual prognosis.
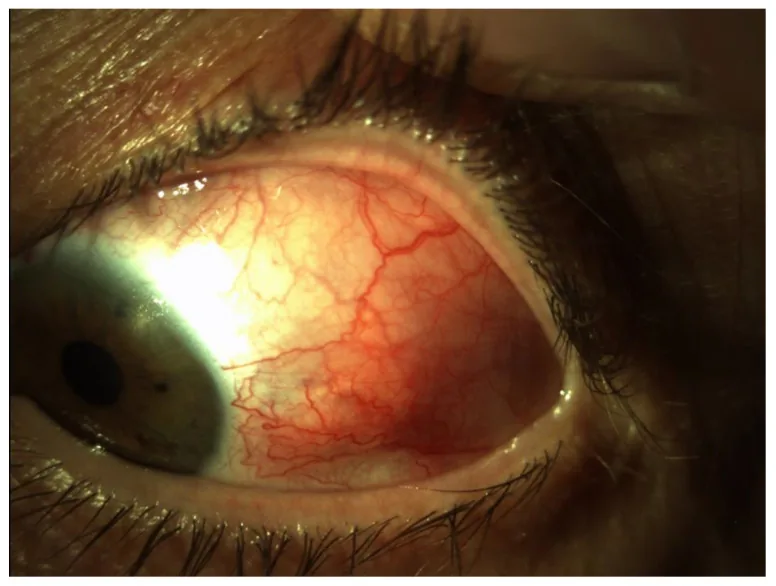
Subjective symptoms vary depending on the type of ocular complication.
Keratoconjunctivitis Sicca
Schirmer test: ≤5 mm/5 min indicates decreased secretion.
BUT (tear break-up time): ≤5 seconds indicates unstable tear film.
Fluorescein staining: Punctate epithelial erosions on inferior cornea and conjunctiva.
Scleritis
Anterior diffuse: Diffuse redness and edema over the entire sclera.
Anterior nodular: Nodule formation on the sclera.
Necrotizing: Central yellowish-white ischemic area with avascular appearance.
Posterior scleritis: Fundus edema, T-sign (on ultrasound).
Episcleritis
Peripheral Corneal Ulcer
Location: Groove-like thinning along 1–2 mm from the limbus.
Progression: Expands circumferentially in a crescent shape and may rapidly lead to perforation.
Fluorescein staining: Positive fluorescein in epithelial defects.
Scleritis is classified according to the Watson classification into anterior scleritis (diffuse, nodular, necrotizing) and posterior scleritis, with necrotizing being the most severe 7). Approximately 30–50% of scleritis patients have a systemic autoimmune disease, with RA being the most common 5).
Scleritis involves inflammation of the blood vessels in the sclera (deep layer of the white of the eye) and is accompanied by severe eye pain (deep, throbbing). The redness is dark red and does not easily blanch with pressure. Conjunctivitis involves superficial redness that is bright red, with mild pain or burning sensation, and the redness easily blanches with pressure. If scleritis is suspected, prompt ophthalmologic evaluation is necessary.
Ocular involvement in RA results from autoimmune-mediated systemic vasculitis and granulomatous inflammation spreading to the scleral and limbal vessels 11).
Patients who develop necrotizing scleritis or peripheral corneal ulcers have been reported to have a reduced 10-year survival rate 8), and these ocular lesions serve as indicators of systemic vasculitis activity.
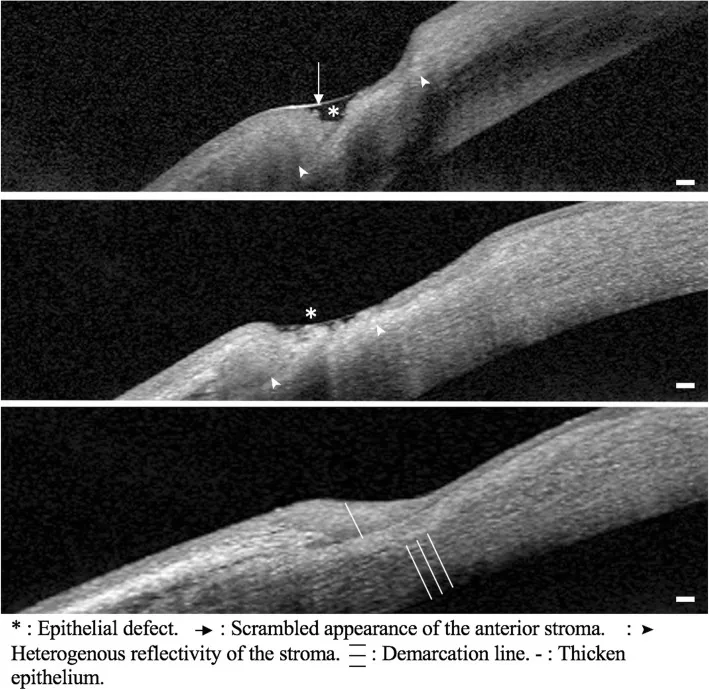
The diagnosis of RA is based on the 2010 ACR/EULAR classification criteria 9). Four domains are scored: number of swollen joints, serological tests (RF, anti-CCP antibody), symptom duration, and acute-phase reactants (CRP, ESR).
In blood tests, elevated ESR, elevated CRP, positive RF (approximately 75%; negative in about 25%), anti-CCP antibody, and elevated MMP-3 are useful for diagnosis 4). On X-ray, joint erosion and bone destruction in the hands and fingers are characteristic.
Ocular complications are evaluated by the following tests.
| Test | Evaluation Target | Finding Criteria |
|---|---|---|
| Schirmer test | Tear secretion volume | ≤5 mm/5 min indicates decreased secretion |
| Tear break-up time (BUT) | Tear film stability | ≤5 seconds indicates instability |
| Slit-lamp microscopy | Sclera, cornea, anterior segment | Check for necrotic changes and corneal thinning |
| Intraocular pressure measurement | Glaucoma, steroid response | Mandatory when using steroids |
| Fundus examination | Posterior scleritis, papilledema | Exclude posterior lesions |
| B-scan ultrasound | Posterior scleritis | T-sign (Tenon’s capsule edema) |
| Orbital MRI | Evaluate extent of posterior scleritis | Scleral thickening and enhancement |
Posterior scleritis is easily overlooked and may present with eye pain, vision loss, proptosis, and diplopia. The T-sign on B-scan ultrasound is useful for diagnosis.
In patients with scleritis, systematic evaluation including RF, ANA, ANCA, complement, and chest X-ray is recommended to screen for systemic diseases5).
Regular ophthalmologic screening is strongly recommended. Early detection and treatment of scleritis and peripheral corneal ulcers directly impact visual prognosis. Especially during periods of high RA disease activity or in malignant RA, ocular screening is important even in the absence of symptoms. Additionally, patients using hydroxychloroquine require regular monitoring for retinal toxicity.
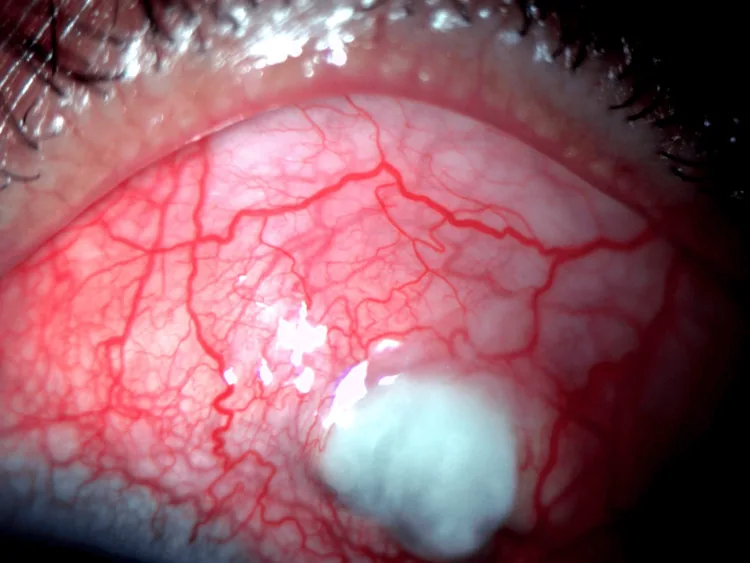
Treatment of ocular manifestations of RA involves both local ophthalmic therapy and systemic treatment by a rheumatologist.
For mild to moderate keratoconjunctivitis sicca, the following are applied stepwise:
In cases with Sjögren’s syndrome, dry eye tends to be more severe, and adding cyclosporine ophthalmic solution may be considered.
| Severity | Treatment Options |
|---|---|
| Mild | Oral NSAIDs (diclofenac sodium 75-100 mg/day, indomethacin 75 mg/day) |
| Moderate | Prednisolone 0.5-1 mg/kg/day orally. Taper after response. |
| Severe/necrotizing | Methylprednisolone 1 g/day IV pulse for 3 days + immunosuppressant |
| Indication for immunosuppressants | Cyclophosphamide (2 mg/kg/day) or azathioprine (2 mg/kg/day) |
| Refractory | Biologics such as rituximab and tocilizumab |
| Scleral perforation | Lamellar keratoplasty or scleral graft using preserved cornea |
Nonsteroidal anti-inflammatory drugs may be effective for nodular and diffuse scleritis, but more aggressive immunosuppressive therapy is required for necrotizing scleritis6).
The following systemic treatments are applied for RA4).
DMARDs (disease-modifying antirheumatic drugs):
Biologic DMARDs:
JAK inhibitors:
Steroids (prednisolone, etc.) carry risks of cataract (posterior subcapsular cataract), increased intraocular pressure, and glaucoma with long-term use, so regular ophthalmologic examinations are necessary. Some biologic agents such as anti-TNF-α antibodies have rarely been reported to cause paradoxical uveitis. Hydroxychloroquine (HCQ) can cause retinal toxicity (hydroxychloroquine retinopathy) when exceeding a certain dose, so annual ophthalmologic monitoring is recommended.
The onset of RA involves a combination of genetic predisposition (HLA-DR4/DR1, etc.) and environmental factors (smoking, protein citrullination by periodontal pathogens, etc.). Autoantibodies against citrullinated proteins (anti-CCP antibodies) are produced and deposited as immune complexes in the joints.
In the synovium, tissue destruction progresses through the following mechanisms:
Ocular manifestations are local expressions of systemic vasculitis and immune reactions in RA 3).
Mechanism of scleritis:
Mechanism of marginal corneal ulcer:
Mechanism of keratoconjunctivitis sicca (associated with Sjögren’s syndrome):
Scleritis and peripheral corneal ulcer are extra-articular manifestations of RA, and their exacerbation and remission parallel systemic vasculitis activity. Suppression of RA disease activity with biologics or immunosuppressants also contributes to improvement of ocular lesions1).
The efficacy of rituximab (anti-CD20 antibody)3) and tocilizumab (anti-IL-6 receptor antibody) for refractory scleritis and peripheral corneal ulcer has been reported in case reports and small studies. Intensification of systemic RA treatment with biologics may contribute to improvement and prevention of recurrence of ocular complications.
Cases of paradoxical uveitis (demyelinating uveitis-like reaction) occurring during anti-TNF-α antibody administration have been reported 4). Ophthalmologic monitoring before and after administration is necessary, and when inflammation worsens, the continuation of administration should be reconsidered.
JAK inhibitors (tofacitinib, baricitinib, etc.) are becoming widely used as systemic treatments for RA, and research on their effects on ocular inflammation such as scleritis is progressing. The JAK-STAT pathway is involved in ocular inflammation mediated by IL-6 and IFN-γ signaling, and local ocular application is expected.
For cases of severe peripheral corneal ulcer perforation, cell engineering approaches such as amniotic membrane transplantation, artificial cornea, and cultured corneal stromal cell transplantation have been attempted. Evaluation of long-term outcomes remains a challenge.
Sainz de la Maza M, Molina N, Gonzalez-Gonzalez LA, et al. Clinical characteristics of a large cohort of patients with scleritis and episcleritis. Ophthalmology. 2012;119(1):43-50.
Galor A, Thorne JE. Scleritis and peripheral ulcerative keratitis. Rheum Dis Clin North Am. 2007;33(4):835-854.
Artifoni M, Rothschild PR, Brézin A, et al. Ocular inflammatory diseases associated with rheumatoid arthritis. Nat Rev Rheumatol. 2014;10(2):108-116.
日本リウマチ学会 編. 関節リウマチ診療ガイドライン2020. メディカルレビュー社; 2021.
Akpek EK, Thorne JE, Qazi FA, Do DV, Jabs DA. Evaluation of patients with scleritis for systemic disease. Ophthalmology. 2004;111(3):501-506. doi:10.1016/j.ophtha.2003.06.006. PMID:15019326.
Jabs DA, Mudun A, Dunn JP, et al. Episcleritis and scleritis: clinical features and treatment results. Am J Ophthalmol. 2000;130(4):469-476.
Watson PG, Hayreh SS. Scleritis and episcleritis. Br J Ophthalmol. 1976;60(3):163-191.
Foster CS, Forstot SL, Wilson LA. Mortality rate in rheumatoid arthritis patients developing necrotizing scleritis or peripheral ulcerative keratitis. Ophthalmology. 1984;91(10):1253-1263.
Aletaha D, Neogi T, Silman AJ, et al. 2010 Rheumatoid arthritis classification criteria: an American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis Rheum. 2010;62(9):2569-2581.
Messmer EM, Foster CS. Vasculitic peripheral ulcerative keratitis. Surv Ophthalmol. 1999;43(5):379-396.
Smith JR, Mackensen F, Rosenbaum JT. Therapy insight: scleritis and its relationship to systemic autoimmune disease. Nat Clin Pract Rheumatol. 2007;3(4):219-226.
Bongartz T, Sutton AJ, Sweeting MJ, et al. Anti-TNF antibody therapy in rheumatoid arthritis and the risk of serious infections and malignancies. JAMA. 2006;295(19):2275-2285.