Method I (Standard Method)
Anesthetic eye drops: Not used (includes reflex secretion)
Indications: The most standard method used for general dry eye screening
Measurement content: Basal secretion + conjunctival sac storage + reflex secretion
The Schirmer test (Schirmer test) is a tear secretion function test devised by Schirmer in 1903. A 5 mm × 35 mm filter paper with 1 mm interval markings is placed on the lower eyelid, and the length (mm) of wetting of the filter paper after 5 minutes is measured to quantitatively evaluate tear secretion.
With a history of over 100 years and simple operation, it is widely used worldwide. Its main purpose is to assist in the diagnosis and severity assessment of dry eye (tear-deficient type), and it also plays an important role in the diagnosis of systemic diseases associated with lacrimal gland hypofunction (e.g., Sjögren’s syndrome, graft-versus-host disease [GVHD]).
Dry eye is a frequently encountered condition in daily practice, with an estimated prevalence of 12.5% in men and 21.6% in women aged 40 years or older 1). The Schirmer test is standardly used for screening and objective evaluation of tear secretion.
According to the 2016 revised diagnostic criteria for dry eye, diagnosis can be made based on “subjective symptoms + BUT ≤ 5 seconds,” and the Schirmer test is no longer mandatory. However, it remains important as a reference indicator when objective quantitative evaluation of tear secretion is needed or when differentiating severe dry eye such as Sjögren’s syndrome or GVHD.
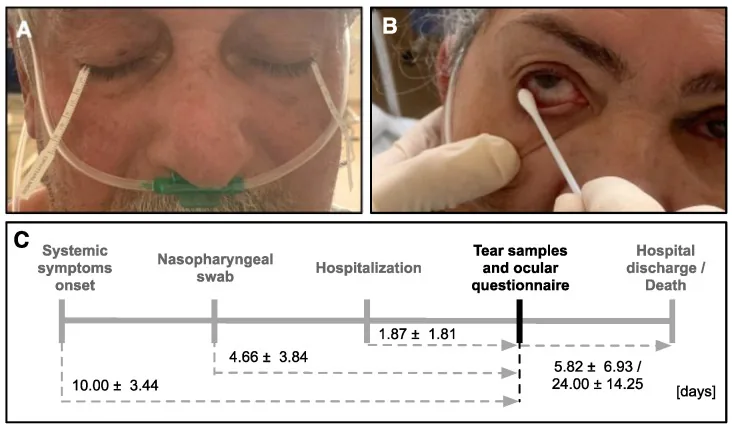
There are three types of Schirmer test, used according to the purpose.
Method I (Standard Method)
Anesthetic eye drops: Not used (includes reflex secretion)
Indications: The most standard method used for general dry eye screening
Measurement content: Basal secretion + conjunctival sac storage + reflex secretion
Method I Modified (Under Anesthesia)
Anesthetic eye drops: Used (0.4% oxybuprocaine hydrochloride ophthalmic solution)
Indication: To evaluate pure basal tear secretion excluding reflex secretion
Measurement: Basal secretion + conjunctival sac reservoir volume
Method II (Nasal Stimulation Test)
Anesthetic eye drops: Not used
Indication: Performed additionally only in cases with low values in Method I
Measurement: Evaluation of reflex secretion (confirms reflex pathway via nasal mucosal stimulation)
The standard procedure for Schirmer Test Method I is described below.
This test is performed additionally only in patients with low tear secretion on the Schirmer I test.
Mechanical stimulation of the nasal mucosa induces reflex tear secretion via the trigeminal nerve. This test checks whether this pathway is intact.
The Schirmer I test does not use topical anesthesia, so there is a sensation of irritation or foreign body when the filter paper contacts the conjunctival sac. There is no severe pain, but tear secretion may be stimulated. In the modified Schirmer I test, anesthesia is performed with 0.4% oxybuprocaine hydrochloride eye drops before the test, reducing the irritation.
The evaluation criteria for each test method are shown below.
| Test Type | Normal Value | Borderline | Abnormal Value |
|---|---|---|---|
| Schirmer I test (old diagnostic criteria) | 10 mm or more | 5 to 10 mm | 5 mm or less |
| Schirmer test I (current criteria) | 10 mm or more | — | 5 mm or less (reference value) |
| Schirmer test II | 10 mm or more | — | 10 mm or less |
In the old dry eye diagnostic criteria (2006), a Schirmer test I value of 5 mm or less was considered positive1). In the current criteria revised in 2016, BUT is the main criterion, and a Schirmer test I value of 5 mm or less is treated as a reference value1).
Understanding the differences in what each test measures helps in accurately interpreting the test results.
| Test type | Basal secretion volume | Conjunctival sac storage volume | Reflex secretion volume |
|---|---|---|---|
| Schirmer test I | ○ | ○ | ○ (includes) |
| Schirmer test I modified | ○ | ○ | ✕ (excludes) |
| Schirmer test II | ○ | ○ | ○ (additional evaluation of reflex secretion by nasal stimulation) |
In the diagnostic criteria for dry eye before 2006, the Schirmer test I value was used as one of the main criteria. However, because the sensitivity and specificity of the Schirmer test are not as high as those of BUT, and the reproducibility of measurement is poor, the 2016 revised diagnostic criteria changed BUT ≤5 seconds to the main criterion, and the Schirmer test was changed to an auxiliary reference value 1). Combining BUT and Schirmer values helps differentiate dry eye subtypes (aqueous-deficient type and evaporative type).
The Schirmer test is widely used in the following clinical situations.
Dry eye screening: The Schirmer I test quantitatively assesses decreased tear secretion. In particular, low values in the Schirmer I test suggest the possibility of aqueous tear-deficient dry eye.
Evaluation of Sjögren’s syndrome and GVHD: For cases with low values on the Schirmer I test, the Schirmer II test is added. If the Schirmer II test also shows abnormal values of 10 mm or less, it indicates impairment of the reflex secretory pathway of the lacrimal gland, providing evidence to suspect severe dry eye such as Sjögren’s syndrome or GVHD.
Objective evaluation of dry eye treatment efficacy: By comparing Schirmer values before and after treatment, changes in tear secretion can be assessed numerically. It is used to confirm the therapeutic effect of eye drops (e.g., cyclosporine ophthalmic solution, diquafosol sodium ophthalmic solution).
Preoperative evaluation for ophthalmic surgery: It is used as a preoperative screening for cataract surgery and refractive surgery (e.g., LASIK) to check for the presence of dry eye. It provides a basis for explaining to patients the risk of dry eye worsening after surgery.
Position in TFOS DEWS III: In the international dry eye workshop (TFOS DEWS III), the Schirmer test is positioned as a test alongside tear meniscus height measurement and OCT measurement for tear volume assessment 2). Although OCT meniscus measurement is superior in terms of sensitivity and specificity, the Schirmer test remains useful due to its widespread availability and simplicity 2).
When the Schirmer II test shows abnormal values of 10 mm or less, it indicates a significant decrease in reflex tear secretion. There is a high possibility of severe dry eye with marked impairment of lacrimal gland function, such as Sjögren’s syndrome (primary or secondary) or GVHD (graft-versus-host disease) after hematopoietic stem cell transplantation. In these diseases, tear secretion is severely reduced, which also affects treatment choices such as the frequency of eye drop use and punctal occlusion (punctal plugs).
The main factors affecting measurement values are as follows:
False high (higher than actual value):
False negative (lower than actual value):
Advantages:
Limitations:
The Schirmer test is a physical method that uses the capillary action of filter paper to absorb and quantify tears. When the graduated filter paper absorbs tears, the liquid advances linearly due to capillary force. The wetting length after 5 minutes serves as a surrogate indicator of tear secretion. This test is the simplest method for evaluating tear volume, requiring no biochemical or optical analysis.
There are several tests for tear evaluation, each assessing different aspects.
Evaluation of tear film stability (BUT test): The tear film breakup time is measured under fluorescein staining. It evaluates the “quality (stability)” of tears. It has been adopted as the primary criterion in the 2016 revised diagnostic criteria for dry eye 1).
Evaluation of tear volume (Schirmer test, OCT meniscus measurement): The Schirmer test assesses secretion volume, while OCT (optical coherence tomography) measurement of the lower tear meniscus height evaluates storage volume. OCT meniscus measurement is non-invasive, highly quantitative and reproducible, with a threshold of 0.2 mm or less indicating a decrease 2).
Subtype classification of dry eye: In aqueous-deficient dry eye, the Schirmer test tends to show low values. In evaporative dry eye, BUT is shortened but Schirmer values are often within the normal range. Combining both tests enables differentiation of subtypes 1).
Tear osmolarity measurement: In recent years, tear osmolarity has gained attention as a biomarker for dry eye. Devices with a positive threshold of 316 mOsm/L or higher are commercially available, allowing complementary evaluation with Schirmer 2).
Measurement of tear meniscus height using anterior segment OCT is being studied as a non-invasive, quantitative, and highly reproducible method for tear volume assessment. It has been shown to have superior sensitivity and specificity compared to the Schirmer test, and may potentially replace Schirmer as a standard test in the future 2). Currently, complementary use of both tests is recommended.
Research has been reported on an improved Schirmer test using a new filter paper material with optimized fiber uniformity and water absorption rate, replacing conventional paper filter paper. The aim is to reduce the coefficient of variation of measurements and improve reproducibility. International efforts toward standardization are ongoing.