Flat Nevus
Appearance: Flat pigmentation on the iris surface
Elevation: None to very slight
Characteristics: The most common type. It appears as shades of pigment spreading along the iris surface.
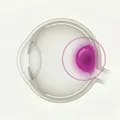
Iris nevus is a benign pigmented tumor caused by proliferation of melanocytes in the iris. Macroscopically, it appears as a dark brown to brown pigmented lesion on the iris. It is usually stationary (non-growing) and malignant transformation is extremely rare; in most cases, only observation is needed. A large study of 1611 cases reported that transformation from iris nevus to malignant melanoma occurred in 2.6% at 5 years and 4.1% at 10 years, indicating a generally stable long-term course [1].
Iris malignant melanoma is a rare tumor arising from the iris among uveal malignant melanomas, and it is often less malignant than intraocular malignant melanomas originating from the choroid or ciliary body. Differentiation between iris nevus and iris malignant melanoma is based on size, presence of growth, and irregularity of shape.
It is more common in Caucasians and tends to occur in people with lightly pigmented irises (blue, green, gray). It is often found in middle-aged and older individuals, but can also occur in younger people. Most cases are asymptomatic and are discovered incidentally during eye examinations or examinations for other diseases.
In most cases, it is a benign iris nevus, and malignant transformation is extremely rare. However, if growth, change in shape, vision changes, or eye pain occur, it is important to see an ophthalmologist promptly. Regular eye examinations can detect any changes early.
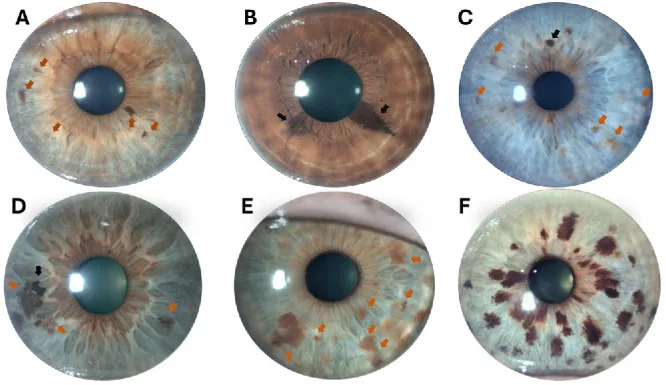
Iris nevi are usually asymptomatic, and cosmetic concerns (changes in iris color or pattern) are often the main complaint. If infiltration occurs in the angle (the drainage pathway of intraocular fluid), it can lead to increased intraocular pressure, and eye pain or decreased vision may appear.
The main findings observed with a slit lamp microscope are as follows:
Iris nevi are classified into the following three types based on morphology:
Flat Nevus
Appearance: Flat pigmentation on the iris surface
Elevation: None to very slight
Characteristics: The most common type. It appears as shades of pigment spreading along the iris surface.
Elevated Nevus
Appearance: A lesion clearly elevated from the iris surface
Elevation: Present
Features: May require differentiation from iris malignant melanoma. Regularly check for growth.
Nodular Type
Appearance: A small nodular pigmented lesion near the pupillary margin
Elevation: Elevated as a small nodule
Features: Requires differentiation from pigmented nodules on the iris seen in Cogan-Reese syndrome.
If the following findings are observed, consider the possibility of transformation to iris malignant melanoma or a malignant lesion, and further examination is necessary. Shields et al. organized the risk of malignant transformation of iris nevus into six items (ABCDEF: Age ≤40 years, Blood [hyphema], Clock hour [inferior 4–9 o’clock position], Diffuse, Ectropion uveae, Feathery margin), which is widely used as a clinical decision indicator [1].
Iris nevus is caused by benign proliferation of melanocytes that make up the iris. Many details of the mechanism of occurrence remain unclear.
The main risk factors include the following:
As a rare association, an association with BAP1 tumor predisposition syndrome has been reported. Families with BAP1 gene mutations are thought to have an increased risk of uveal melanoma, and caution may be needed in the observation of iris nevi.
The basic diagnostic test for iris nevus is detailed observation of the anterior segment using a slit-lamp microscope. Record the size, color, shape, borders, and degree of elevation of the lesion. Taking high-resolution photographs regularly and tracking changes over time is the core of management.
Anterior segment OCT is a useful test for quantitatively evaluating the depth and height of iris nevi. It can quantify tumor thickness and width and objectively record changes over time. Combined with slit-lamp photography, early detection of growth is possible. Anterior segment OCT has been reported to capture 96% of iris melanocytic tumors, and for evaluating pure iris tumors, it is a useful non-contact and simple method, while UBM is superior for detecting ciliary body invasion [4].
Ultrasound biomicroscopy (UBM) is useful for evaluating invasion of the ciliary body and angle using anterior segment ultrasound. It is performed when a raised iris nevus or extension to the ciliary body is suspected. It assesses the presence and extent of angle invasion and evaluates glaucoma risk.
When an iris nevus invades the angle, pigment dispersion to the trabecular meshwork can cause elevated intraocular pressure. Regular intraocular pressure measurement enables early detection of secondary glaucoma.
Important differential diagnoses of iris nevus are shown in the table below.
| Disease | Key Points for Differentiation |
|---|---|
| Iris malignant melanoma | Rapid growth, irregular shape, ciliary body invasion, angle seeding, rubeosis iridis. May be small and locally resectable. |
| Cogan-Reese syndrome | Unilateral pigmented nodules on the iris with pigmentation, accompanied by slowly progressive peripheral anterior synechiae and glaucoma. A variant of the iridocorneal endothelial syndrome. |
| Metastatic iris tumor | Often white to milky white in color. May be multiple. Check history of primary tumor in other organs. |
| Juvenile xanthogranuloma (JXG) | Common in infants and young children. Yellow to orange iris nodules. May present with hyphema. |
Cogan-Reese syndrome is characterized mainly by pigmented nodular elevated lesions or pigmentation on the iris of one eye, resembling iris nevus, and gradually causes peripheral anterior synechiae leading to glaucoma. Morphologically, it is difficult to distinguish from iris nevus, and sometimes differentiation from malignant melanoma is necessary.
If there is rapid enlargement, irregular shape or indistinct borders, angle infiltration, iris rubeosis (iris neovascularization), local inflammatory reaction, or hemorrhage, iris malignant melanoma should be suspected. Combine quantitative evaluation with anterior segment OCT/UBM and regular photographic documentation, and consider referral to an ocular oncology center if changes are observed.
For small iris nevi without enlargement, observation is the basic policy. Regular slit-lamp photographic documentation tracks changes in lesion size and shape. Combining quantitative evaluation with anterior segment OCT allows objective recording of even minute changes.
General guideline for observation intervals (may vary depending on facility policy):
If findings suggest malignancy, referral to an ocular oncology center is appropriate. The following treatments may be selected.
Iris malignant melanoma is often less malignant than intraocular malignant melanoma originating from the choroid or ciliary body, but appropriate management is necessary due to the risk of infiltration and metastasis. Iris malignant melanoma accounts for about 4% of uveal malignant melanoma, with reported mean tumor diameter at diagnosis of 5.5 mm, seeding in 28%, and secondary glaucoma in 35%, highlighting the importance of early management [2].
If secondary glaucoma due to angle infiltration is present, glaucoma treatment should be performed concurrently. Topical medication for intraocular pressure control is the first choice; if control is poor, surgical therapy should be considered.
Most iris nevi follow a benign course. Malignant transformation is very rare, and it is important to detect changes early through regular follow-up. If no growth or morphological changes are observed, the condition often remains stable over the long term.
Iris nevi are formed by benign proliferation of melanocytes in the iris stroma. Melanocytes are cells that produce pigment (melanin) and determine the color of the iris. In nevi, cell proliferation is localized and does not show invasive growth, which is the essential difference from malignant lesions.
Most iris nevi are stationary, but rarely they may undergo malignant transformation to iris malignant melanoma. The mechanism of malignant transformation is thought to involve molecular abnormalities such as GNAQ/GNA11 mutations found in uveal melanoma overall, but many details of the specific malignant transformation mechanism of iris nevi remain unknown.
Pigment granules shed from an iris nevus may be dispersed into the angle (anterior chamber angle). When these dispersed pigments deposit on the trabecular meshwork (the intraocular aqueous humor drainage pathway), outflow resistance may increase, leading to elevated intraocular pressure. Secondary glaucoma due to this mechanism can be detected early by intraocular pressure measurement and regular gonioscopy.
Cogan-Reese syndrome is a type of iridocorneal endothelial (ICE) syndrome. ICE syndrome is a unilateral disease common in middle-aged women and is classified into three types: essential iris atrophy, Chandler syndrome, and Cogan-Reese syndrome [5]. Abnormally proliferated corneal endothelial cells cover the anterior surface of the iris, and compression or traction on the iris forms nodular lesions resembling iris nevi and pigmentation. Gradually, peripheral anterior synechiae progress, leading to glaucoma. Morphologically, it may be difficult to distinguish from iris nevi; evaluation of corneal endothelial cell abnormalities (by specular microscopy) aids in differentiation [5].
Quantitative longitudinal evaluation of iris nevi using anterior segment OCT is attracting attention as a method to objectively capture minute changes in tumor thickness, width, and volume. Compared to conventional slit-lamp photography, it may reduce inter-observer variability and enable early detection of growth.
Establishment of quantitative criteria to accurately differentiate iris nevi from iris malignant melanoma based on imaging findings is needed. Development of risk stratification criteria specific to iris lesions, similar to the TFSOM-UHHD criteria for choroidal nevi, is considered a future challenge.
Large-scale, long-term data on the prevalence and malignant transformation rate of iris nevi are limited, and accumulation of epidemiological data, especially in Asian populations, is needed. Multi-center, long-term cohort studies are required to identify risk factors for malignant transformation and determine optimal follow-up intervals.