Entropion
Key Points at a Glance
Section titled “Key Points at a Glance”1. What is Entropion?
Section titled “1. What is Entropion?”Entropion is a condition in which the eyelid margin turns inward toward the eye, causing the eyelashes to contact the ocular surface and leading to corneal epithelial damage. Symptoms include foreign body sensation, tearing, and discharge.
Entropion is broadly classified into congenital and acquired types. Acquired entropion is further subdivided into involutional (age-related), cicatricial, spastic, and mechanical types. Since the pathophysiology, predilection sites, and treatment methods differ significantly by type, accurate identification of the type is essential for treatment selection.
Epidemiology
Section titled “Epidemiology”Congenital entropion (epiblepharon) is common in East Asians and rare in Caucasians. Most cases of entropion in infants are called epiblepharon or congenital entropion. It tends to be more prominent on the nasal side of the lower eyelid.
Involutional entropion most commonly occurs in the lower eyelids of elderly individuals. According to a review by Lin et al., it occurs in approximately 2.1% of the elderly population and is more frequent in East Asians [1].
Regarding the significance of surgical intervention for congenital entropion (epiblepharon), surgical treatment is standard for symptomatic cases or those with corneal damage, and many reports recommend active surgical intervention rather than waiting for spontaneous resolution [4].
Cicatricial entropion is primarily caused by trachoma worldwide, and can also result from Stevens-Johnson syndrome, ocular pemphigoid, chemical trauma, etc. Unlike other types, it can also occur in the upper eyelid.
2. Main Symptoms and Clinical Findings
Section titled “2. Main Symptoms and Clinical Findings”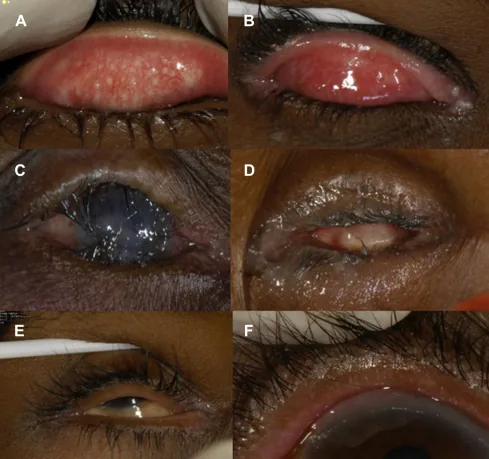
Subjective Symptoms
Section titled “Subjective Symptoms”Subjective symptoms of entropion arise from contact of the eyelashes or inverted eyelid skin with the ocular surface.
- Foreign body sensation: Persistent feeling of sand in the eye
- Eye pain: Pain associated with corneal epithelial damage
- Tearing: Reflex tearing due to ocular surface irritation
- Eye discharge: Increased secretions due to inflammation or epithelial damage
- Photophobia: Light sensitivity due to corneal epithelial damage
- Decreased vision: Occurs with progression of corneal opacity or irregular astigmatism
The severity of symptoms varies. While some cases resolve spontaneously with growth, if symptoms persist and become a factor hindering visual development or negatively affect emotional well-being, surgery may be indicated.
Clinical Findings
Section titled “Clinical Findings”- Inward rolling of the eyelid margin: Adduction toward the eyeball can be confirmed on visual inspection
- Contact of eyelashes with cornea and conjunctiva: Contact sites can be confirmed with fluorescein staining
- Corneal epithelial damage: Punctate keratopathy, erosion, and opacity may occur
- Conjunctival injection and inflammation: Reactive changes due to chronic irritation
Characteristic Findings by Type
Section titled “Characteristic Findings by Type”In congenital entropion (epiblepharon), inversion is more pronounced on the nasal side of the lower eyelid, and a chin-up head posture (compensatory posture with the jaw thrust forward) may be observed. In involutional entropion, the entire lower eyelid turns inward, and the eyelid skin including the eyelashes contacts the cornea and conjunctiva. In cicatricial entropion, conjunctival scarring and shortening are observed, and it can also occur in the upper eyelid. In spastic entropion, strong orbicularis oculi muscle spasm accompanies the inversion.
In congenital entropion (epiblepharon), spontaneous resolution may occur with growth due to facial skeletal development and increased orbital volume, which relatively reduces the excess of the anterior lamella. However, in school-age children with corrected visual acuity less than 1.0, there is a risk of amblyopia, so surgery should be actively considered without waiting for spontaneous improvement. In involutional and cicatricial entropion, spontaneous resolution is not expected.
3. Classification and Types
Section titled “3. Classification and Types”Entropion is classified into five types based on differences in pathophysiology. Since treatment strategies differ fundamentally by type, accurate identification of the type at the initial visit is important.
| Type | Pathophysiology | Common site | Common age | Main features |
|---|---|---|---|---|
| Congenital (epiblepharon) | Excess anterior lamella (congenitally redundant skin and orbicularis muscle) | Nasal side of lower eyelid | Infants and young children | Common in East Asians. Some cases resolve spontaneously. |
| Age-related (involutional) | Laxity of lower eyelid supporting structures (e.g., capsulopalpebral fascia) | Lower eyelid | Elderly | Most common. Hotz procedure alone is inappropriate. |
| Cicatricial | Scar contracture of the posterior lamella (tarsus and conjunctiva) | Upper and lower eyelids | All ages | Caused by trachoma, SJS, ocular pemphigoid, etc. |
| Spastic | Spasm of the orbicularis oculi muscle (overriding) | Lower eyelid | Elderly | Often secondary to surgery or ocular surface inflammation |
| Mechanical | Decreased orbital volume | Lower eyelid | All ages | Anophthalmos, phthisis bulbi, orbital fat atrophy |
Detailed Description of Each Type
Section titled “Detailed Description of Each Type”Congenital (epiblepharon)
The essence of the pathology is that the anterior lamella (skin + orbicularis oculi muscle) is inherently redundant compared to the posterior lamella (tarsus). In East Asians, the presence of epicanthus promotes anterior lamellar excess, and poor development of the nasal tarsus is also considered a contributing factor. Natural resolution can occur as facial skeletal development and increased orbital volume with growth relatively resolve the anterior lamellar redundancy.
Involutional (degenerative)
The main pathology is laxity of the lower eyelid retractor aponeurosis. This laxity causes the inferior tarsal border to move anteriorly and superiorly, and the eyelid margin moves inward (downward), resulting in entropion. Relaxation of the orbicularis oculi muscle and changes in its direction of action also contribute to entropion. Atrophy of orbital fat and enophthalmos associated with aging may also contribute. Since the pathology is laxity of supporting tissues, the Hotz method, which corrects anterior lamellar redundancy, is inappropriate and does not address the condition.
Cicatricial
This occurs when scar tissue from trauma or inflammation contracts the posterior lamella (tarsus and conjunctiva). Shortening of the posterior lamella causes the eyelid margin to roll inward. Causative diseases include trachoma (chronic conjunctivitis due to Chlamydia trachomatis leading to scarring), Stevens-Johnson syndrome (extensive conjunctival scarring associated with severe drug eruption), ocular cicatricial pemphigoid (autoimmune progressive conjunctival scarring), and after chemical trauma or burns. A characteristic feature is that it can also occur in the upper eyelid.
Spastic
This results from strong spasm of the orbicularis oculi muscle rotating the eyelid margin inward. It is often triggered by reflex orbicularis contraction due to postoperative or ocular surface inflammation.
Mechanical
This is caused by reduced globe volume, such as anophthalmos, phthisis bulbi, or orbital fat atrophy. Enophthalmos prevents the eyelid from supporting the globe, leading to entropion. It may improve with appropriate prosthetic eye wear.
4. Diagnosis and Examination Methods
Section titled “4. Diagnosis and Examination Methods”Visual Inspection and History Taking
Section titled “Visual Inspection and History Taking”Visual inspection of the condition where eyelashes touch the ocular surface is easy. Confirm the extent and degree of eyelid rolling and the site of lash contact.
In history taking, confirm whether the condition is congenital or acquired. When entropion that was not present from birth occurs in young or middle-aged adults, factors such as trauma or inflammation should be considered. Also check for history of trauma, surgery, or inflammatory eye diseases (SJS, ocular cicatricial pemphigoid, etc.).
Examination
Section titled “Examination”- Slit-lamp microscopy: Evaluates the eyelid margin and eyelash condition, presence of conjunctival scarring, and corneal epithelial damage.
- Fluorescein staining: Confirms the extent and severity of corneal epithelial damage.
- Visual acuity and refraction tests: Assess induced astigmatism. In children, corrected visual acuity measurement directly determines surgical indication.
Surgical Indication
Section titled “Surgical Indication”Surgical indication is determined based on subjective symptoms, visual acuity, induced astigmatism, and the degree of corneal epithelial damage or opacity. Although entropion may improve spontaneously with age to some extent, surgery should be actively recommended in children of school age or younger with poor corrected visual acuity below 1.0.
Differential Diagnosis
Section titled “Differential Diagnosis”- Trichiasis: A condition where individual eyelashes are misdirected without inversion of the entire eyelid. Eyelid position is normal.
- Pseudo-entropion: Apparent eyelash contact due to epicanthus. The eyelid margin itself is not inverted.
- Congenital glaucoma: Mechanical eyelash contact due to buphthalmos (enlarged eye). Accompanied by elevated intraocular pressure and increased corneal diameter.
Entropion is a condition where the entire eyelid margin rolls inward toward the eye, with an underlying eyelid position abnormality. In contrast, trichiasis involves normal eyelid margin position, but individual eyelashes are directed posteriorly (toward the eye). Treatments also differ: entropion requires surgery to correct eyelid position, while trichiasis is mainly managed by removal of abnormal lashes, electrolysis, or cryotherapy.
5. Standard Treatment
Section titled “5. Standard Treatment”5-1. Conservative Treatment
Section titled “5-1. Conservative Treatment”Children (up to about 2 years old)
Because the eyelashes are thin and soft, damage to the cornea is relatively mild. Conservative observation is possible while protecting the cornea with sodium hyaluronate eye drops. This approach is reasonable during the period when spontaneous healing due to growth can be expected.
Spastic entropion
Injection of botulinum toxin can relieve orbicularis oculi muscle spasm and improve entropion in some cases. Since the effect is temporary, removal of the underlying cause (postoperative inflammation, ocular surface disease) is important.
Mechanical entropion
Attempt to improve entropion with appropriate artificial eye wear. Adjusting the shape and size of the artificial eye to the orbital volume improves eyelid support.
5-2. Surgery for congenital (pediatric) epiblepharon
Section titled “5-2. Surgery for congenital (pediatric) epiblepharon”Surgical indications
Surgery is considered when any of the following apply:
- Persistent cases where spontaneous healing is not expected
- Cases with risk of amblyopia (corrected visual acuity less than 1.0 in school-age children or younger)
- Cases with adverse emotional effects
Incision method (Hotz method)
The Hotz method combines excision of excess skin and eversion correction of the eyelid margin using sutures.
- Excision of excess skin should be minimal, about 1-2 mm
- The excision area should avoid the lacrimal punctum and cover about two-thirds of the nasal side of the eyelid horizontally
- Treat the orbicularis oculi muscle while preserving it as much as possible.
- Pass a 6-0 nylon suture.
- Order of suture passage: lower skin → half-layer of tarsal plate → skin on the eyelid margin side.
Suture method (buried suture method)
This is a surgical technique that minimizes skin incision and everts the eyelid margin using only sutures.
- Use 7-0 nylon suture with a 0 cutting needle.
- Pass sutures at 3 points on the upper eyelid and 2-3 points on the lower eyelid.
- The strength of the ligation should be such that the knot is buried under the skin by the tension of the suture.
5-3. Surgery for age-related (involutional) lower eyelid entropion
Section titled “5-3. Surgery for age-related (involutional) lower eyelid entropion”For age-related lower eyelid entropion, the principle is to select a surgical technique that corrects the relaxation of the tarsal supporting tissues. Lin et al. organized the main factors of age-related lower eyelid entropion into three elements: “vertical laxity of the lower eyelid, horizontal laxity, and overriding of the preseptal orbicularis oculi muscle over the pretarsal orbicularis oculi muscle.” They reported that combining surgical techniques that directly correct these factors reduces the recurrence rate [1]. They are broadly classified into three categories.
1. Shortening of the lower eyelid retractor aponeurosis
Shorten and refix the relaxed retractor aponeurosis to return the tarsal plate to its normal position, correcting vertical laxity.
- Modified Jones method
- Kakizaki method
2. Shortening of horizontal eyelid supporting tissues
Shorten the horizontally lax eyelid supporting tissues to restore overall eyelid tension.
- Wheeler modification combined with Hisatomi method
- Lateral tarsal strip procedure
3. Combination of the above
For combined vertical and horizontal laxity, a procedure combining both approaches is selected. In cases of combined laxity, this approach is effective in preventing recurrence. In a randomized controlled trial by Nakos et al., the lateral tarsal strip group (success rate 88.5% at 12 months postoperatively) showed significantly better results than the everting sutures alone group (57.1%) [2]. In a long-term outcome report by Jang et al., recurrence was observed within 2 years in 49.3% of cases with Quickert alone, and it is recommended to consider combining other procedures in men and in cases with horizontal lower eyelid laxity [3].
5-4. Treatment of cicatricial entropion
Section titled “5-4. Treatment of cicatricial entropion”It is essential to evaluate and manage the activity of the underlying disease (trachoma, Stevens-Johnson syndrome, ocular cicatricial pemphigoid, etc.). Surgical correction of posterior lamellar scar contracture is performed, but in progressive scarring diseases (ocular cicatricial pemphigoid, severe post-SJS), scarring continues postoperatively, leading to many refractory cases that may require multiple surgeries. Ross et al. reported that procedures centered on anterior lamellar repositioning and terminal tarsal rotation, which reposition and recess tissues without excision, are useful for upper eyelid cicatricial entropion, and that excision should be avoided especially in progressive immune diseases [5]. Trachomatous cicatricial entropion/trichiasis is a leading cause of blindness worldwide, and bilamellar tarsal rotation is the standard surgical procedure as part of the WHO SAFE strategy’s S (surgery) [6].
5-5. Postoperative precautions
Section titled “5-5. Postoperative precautions”Swelling (edema) always occurs after surgery. Congenital epiblepharon has a higher recurrence rate. Reoperation for recurrence due to undercorrection is not very difficult. It is important to fully explain the possibility of recurrence to the patient and guardians in advance.
It is inappropriate. The pathology of age-related lower eyelid entropion is laxity of the lower eyelid retractor aponeurosis. The Hotz procedure alone, which corrects anterior lamellar excess, does not address the essence of the pathology and leads to a high recurrence rate. The basic principle is to select a retractor aponeurosis shortening procedure such as the Jones modification or Kakizaki method, or a horizontal supporting tissue shortening procedure such as the lateral tarsal strip, or a combination thereof.
Until around 2 years of age, the eyelashes are thin and soft, and corneal damage is mild, so observation with sodium hyaluronate eye drops for protection is possible. However, in children of school age or younger with poor corrected visual acuity below 1.0, surgery is actively recommended to prevent progression of amblyopia. Surgery is also indicated when symptoms persist and have a negative impact on emotional well-being.
6. Pathophysiology and Detailed Mechanism of Onset
Section titled “6. Pathophysiology and Detailed Mechanism of Onset”Basic Anatomy of the Eyelid
Section titled “Basic Anatomy of the Eyelid”The eyelid consists of two layers: the anterior lamella and the posterior lamella.
- Anterior lamella: Skin + orbicularis oculi muscle (innervated by cranial nerve VII)
- Posterior lamella: Tarsal plate + conjunctiva, and in the upper eyelid, the levator aponeurosis and Müller’s muscle; in the lower eyelid, the lower eyelid retractor aponeurosis
The balance between the anterior and posterior lamellae determines the position of the eyelid margin. Excess, shortening, or laxity of either layer is the basis of the pathology.
Mechanism of Congenital (Entropion/Epiblepharon)
Section titled “Mechanism of Congenital (Entropion/Epiblepharon)”The fundamental pathology is that the anterior lamella (skin + orbicularis oculi muscle) is inherently redundant relative to the posterior lamella (tarsal plate). The redundant anterior lamella pushes the eyelashes inward. In East Asians, the presence of epicanthus contributes to anterior lamellar excess, and poor development of the nasal tarsal plate is also a factor. As the facial skeleton develops and orbital volume increases with growth, the relative anterior lamellar redundancy resolves, allowing the eyelid margin to return to a normal position, leading to spontaneous resolution.
Mechanism of Age-Related (Involutional) Entropion
Section titled “Mechanism of Age-Related (Involutional) Entropion”The starting point is age-related laxity and thinning of the lower eyelid retractor aponeurosis. Laxity of the aponeurosis causes the lower border of the tarsal plate to move anteriorly and superiorly, resulting in inward and downward displacement of the eyelid margin, leading to entropion. The orbicularis oculi muscle also becomes lax with age, and changes in its direction of action further induce entropion. Atrophy of orbital fat and enophthalmos cause the eyelid to separate from the globe, and entropion due to lack of support is exacerbated.
Mechanism of Cicatricial Entropion
Section titled “Mechanism of Cicatricial Entropion”The essence is that scar tissue after trauma or inflammation contracts the posterior lamella (tarsal plate and conjunctiva). Shortening of the posterior lamella causes the eyelid margin to roll inward.
- Trachoma: Repeated chronic conjunctivitis caused by Chlamydia trachomatis leads to progressive scarring of the upper tarsal conjunctiva.
- Stevens-Johnson syndrome (SJS): Scarring occurs after extensive conjunctival and corneal epithelial damage associated with severe drug eruptions.
- Ocular cicatricial pemphigoid: Progressive conjunctival scarring due to an autoimmune mechanism, with ongoing scarring during the active phase.
Spastic mechanism
Section titled “Spastic mechanism”Caused by spasm of the orbicularis oculi muscle rotating the eyelid margin inward. It is often triggered by reflex orbicularis contraction due to postoperative irritation, ocular surface inflammation, or dry eye. Treatment of the underlying condition along with botulinum toxin injection may be effective.
7. Prognosis and course
Section titled “7. Prognosis and course”Congenital (epiblepharon)
Some cases resolve spontaneously with growth, while those with persistent symptoms or risk of amblyopia require surgery. Management of amblyopia (corneal astigmatism → anisometropia) is important, and regular visual acuity assessment is needed even after surgery. Both incision and suture methods have a certain recurrence rate, but reoperation is relatively easy.
Age-related
Prognosis after surgery is good if an appropriate procedure (retractor aponeurosis shortening plus horizontal support tissue shortening) is selected. Recurrence can occur but can be managed with reoperation. Recurrence rate is high if only the Hotz procedure is performed.
Cicatricial
Management of the underlying disease greatly influences prognosis. Progressive scarring diseases (ocular cicatricial pemphigoid, severe post-SJS) are refractory and may require multiple surgeries. Since postoperative scarring continues as long as the underlying disease activity persists, collaboration with internal medicine, dermatology, and immunology is necessary.
Spastic
Botulinum toxin provides temporary improvement, but the effect lasts only a few months. Fundamentally, it is important to eliminate triggers such as ocular surface inflammation and dry eye.
8. References
Section titled “8. References”-
Lin P, Kitaguchi Y, Mupas-Uy J, Sabundayo MS, Takahashi Y, Kakizaki H. Involutional lower eyelid entropion: causative factors and therapeutic management. Int Ophthalmol. 2019;39(8):1895-1907. PMID: 30315389. https://pubmed.ncbi.nlm.nih.gov/30315389/
-
Nakos EA, Boboridis KG, Kakavouti-Doudou AA, Almaliotis DD, Sioulis CE, Karampatakis VE. Randomized Controlled Trial Comparing Everting Sutures with a Lateral Tarsal Strip for Involutional Lower Eyelid Entropion. Ophthalmol Ther. 2019;8(3):397-406. PMID: 31127533. https://pubmed.ncbi.nlm.nih.gov/31127533/
-
Jang SY, Choi SR, Jang JW, Kim SJ, Choi HS. Long-term surgical outcomes of Quickert sutures for involutional lower eyelid entropion. J Craniomaxillofac Surg. 2014;42(8):1629-1631. PMID: 24962041. https://pubmed.ncbi.nlm.nih.gov/24962041/
-
Woo KI, Kim YD. Management of epiblepharon: state of the art. Curr Opin Ophthalmol. 2016;27(5):433-438. PMID: 27213926. https://pubmed.ncbi.nlm.nih.gov/27213926/
-
Ross AH, Cannon PS, Selva D, Malhotra R. Management of upper eyelid cicatricial entropion. Clin Exp Ophthalmol. 2011;39(6):526-536. PMID: 21819506. https://pubmed.ncbi.nlm.nih.gov/21819506/
-
Rajak SN, Collin JRO, Burton MJ. Trachomatous trichiasis and its management in endemic countries. Surv Ophthalmol. 2012;57(2):105-135. PMID: 22285842. PMCID: PMC3316859. https://pubmed.ncbi.nlm.nih.gov/22285842/
