Dermatochalasis
1. What is dermatochalasis?
Section titled “1. What is dermatochalasis?”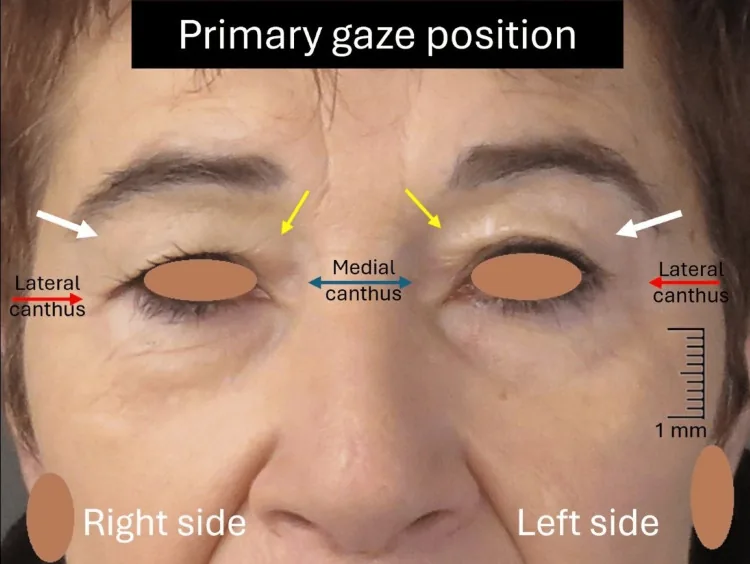
Dermatochalasis is a condition in which excess upper eyelid skin hangs over the eyelid margin despite MRD-1 (margin reflex distance-1: distance from corneal light reflex to upper eyelid margin) ≥ 3.5 mm, i.e., without ptosis. It is also called “skin laxity” 12.
The normal value of MRD-1 is 3.5 to 5.5 mm, and maintaining this value is the essential differentiating point from ptosis 1.
Classification
Section titled “Classification”Dermatochalasis is broadly classified into two types based on the presence or absence of ptosis.
| Type | Characteristics | MRD-1 |
|---|---|---|
| Isolated type | Only excess skin. Levator function is normal. | 3.5 mm or more |
| Combined with ptosis | Excess skin plus decreased MRD-1 and decreased levator function. | Less than 3.5 mm |
In elderly individuals, the combined type with ptosis is more common than the isolated type. Since excess skin and decreased levator function coexist, it is important to accurately evaluate both during examination.
Epidemiology
Section titled “Epidemiology”It is frequently observed as an age-related change. With aging, the eyelid skin becomes thinner and loses elasticity, and continuous gravitational traction leads to the formation of excess skin. In elderly individuals, it is often combined with ptosis. Detailed epidemiological data on prevalence and age distribution are limited.
In dermatochalasis, MRD-1 is maintained at 3.5 mm or more, and only excess skin causes the skin to hang over the eyelid margin. Ptosis is a condition where MRD-1 is less than 3.5 mm, and the essence is a decrease in levator function. However, in elderly individuals, both conditions often coexist, and measuring MRD-1 while holding down the eyebrows during examination is important for differentiating between the two.
2. Main Symptoms and Clinical Findings
Section titled “2. Main Symptoms and Clinical Findings”Functional Symptoms
Section titled “Functional Symptoms”- Superior visual field constriction: Excess skin covering the pupillary area causes visual field impairment. This manifests as overlooking steps in daily life or difficulty with reading and computer work3.
- Heaviness of the eyelids: The weight of excess skin causes a feeling of fatigue when opening the eyes. Symptoms tend to worsen with prolonged reading or work.
- Shoulder stiffness and frontal headache: Compensatory eyebrow elevation leads to sustained contraction of the frontalis muscle, causing shoulder stiffness, neck and shoulder pain, and tension-type headaches in the forehead4.
Skin Symptoms
Section titled “Skin Symptoms”- Dermatitis of the lateral canthus: Contact between the upper and lower skin at the outer corner of the eye (lateral canthus) creates friction and a moist environment, leading to chronic dermatitis.
- Epiphora from the lateral canthus: Skin contact at the lateral canthus can impede tear drainage and cause epiphora.
Clinical Findings
Section titled “Clinical Findings”- Drooping of excess upper eyelid skin: The skin hangs over the eyelid margin, sometimes covering the eyelid crease.
- Maintenance of MRD-1 ≥ 3.5 mm: This is a criterion to confirm that it is not true ptosis.
- Compensatory eyebrow elevation: Tension in the frontalis muscle raises the eyebrow position, sometimes maintaining an apparently normal upper eyelid position.
- Forehead wrinkles: Formed as a result of long-term frontalis muscle contraction.
- Skin fold on upward gaze: Excess skin may fold over the pupillary area and obstruct the visual field.
3. Diagnosis and Examination Methods
Section titled “3. Diagnosis and Examination Methods”Key Points in Examination
Section titled “Key Points in Examination”Compensatory eyebrow elevation may keep the apparent MRD-1 normal. Therefore, measuring MRD-1 in the usual state alone may not accurately assess the degree of excess skin.
By gently pressing the upper eyelid with a finger to prevent eyebrow elevation and asking the patient to look straight ahead, the degree of excess skin becomes clearer. Measure MRD-1 in this state to determine the presence of concomitant ptosis.
With the upper eyelid gently pressed by a finger to prevent compensatory eyebrow elevation, ask the patient to look straight ahead and measure MRD-1. If MRD-1 is 3.5 mm or more and excess skin droops over the eyelid margin, dermatochalasis is diagnosed. If MRD-1 is 2 mm or less, consider concomitant ptosis and evaluate combined ptosis surgery.
Determination of Surgical Indication Based on MRD-1
Section titled “Determination of Surgical Indication Based on MRD-1”Based on the measured MRD-1 value, surgical indication and procedure selection are determined as follows.
| MRD-1 Value | Clinical Judgment | Recommended Procedure |
|---|---|---|
| 3–3.5 mm | Dermatochalasis alone | Skin excision only |
| 2 mm or less | High likelihood of coexisting ptosis | Consider combining ptosis surgery |
Additional Evaluation Items
Section titled “Additional Evaluation Items”- Measurement of levator function (LF): With the brow held down, measure the excursion of the eyelid margin from downgaze to upgaze. Normal is 10 mm or more. Less than 4 mm indicates severe levator dysfunction.
- Assessment of superior visual field defect: Confirming that redundant skin is an objective cause of visual field impairment is useful for determining surgical indication.
4. Differential Diagnosis
Section titled “4. Differential Diagnosis”The main diseases to be distinguished from dermatochalasis are listed below.
- Ptosis (aponeurotic, congenital, etc.): MRD-1 is less than 3.5 mm, and levator function is decreased. The palpebral fissure is narrow even without redundant skin, which differs from dermatochalasis. Age-related aponeurotic ptosis is the most common acquired ptosis in the elderly, characterized by elevation or loss of the eyelid crease and superior sulcus deformity.
- Pseudo-ptosis: A condition in which MRD-1 is normal but there is an apparent drooping sensation due to skin laxity. It conceptually overlaps with dermatochalasis.
- Brow ptosis: A condition in which the redundant skin of the upper eyelid appears relatively increased due to a lowered brow position. It is differentiated by evaluating brow position.
5. Standard Treatment
Section titled “5. Standard Treatment”5-1. Surgical Indications
Section titled “5-1. Surgical Indications”Surgery is indicated when functional impairment (superior visual field constriction) due to excess skin is present. Refer to the above determination of surgical indication based on MRD-1 to select the surgical procedure.
Postoperatively, eyelid swelling may occur, presenting a transient ptosis-like state. Therefore, if even mild ptosis is present preoperatively, consider combining ptosis surgery after consulting with the patient.
5-2. Eyelid margin skin excision (standard blepharoplasty)
Section titled “5-2. Eyelid margin skin excision (standard blepharoplasty)”This is a standard procedure in which excess skin is excised through an incision line in the upper eyelid crease12.
Advantages:
- In cases with concomitant ptosis, the levator aponeurosis and Müller’s muscle can be approached through the same surgical field.
- Since levator advancement can be performed simultaneously, skin laxity and ptosis can be treated in a single surgery.
- There is a cosmetic advantage of being able to create a new eyelid crease.
Disadvantages:
- In upper eyelids with thick anterior lamella and skin, the postoperative eyelid crease may appear thick and puffy.
5-3. Subbrow skin excision (brow-scar blepharoplasty)
Section titled “5-3. Subbrow skin excision (brow-scar blepharoplasty)”This is a procedure in which an incision is made along the lower border of the eyebrow and excess skin is excised5. In Asians, subbrow incision for excess skin removal has been reported as a method that efficiently treats lateral hooding while minimizing cosmetic changes5.
Advantages:
- Because the thin skin near the eyelid margin is preserved, postoperative cosmetic changes are minimal.
- This procedure is particularly advantageous for upper eyelids with thick skin.
- The scar under the eyebrow is hidden by the eyebrow, so postoperative cosmetic problems are unlikely to occur.
Options for two-stage surgery:
In upper eyelids with thick skin, a two-stage surgery may be effective: first perform subbrow skin excision, then add an upper eyelid crease skin excision. By reducing skin thickness in the first stage and forming the crease in the second stage, a more natural cosmetic result can be achieved.
5-4. Summary of surgical technique selection
Section titled “5-4. Summary of surgical technique selection”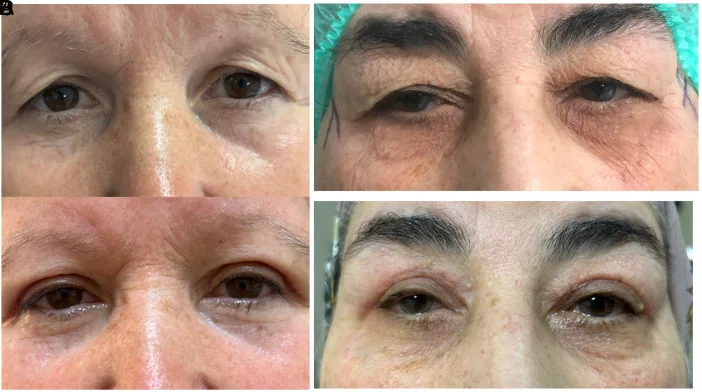
| Surgical technique | Main indications | Advantages | Disadvantages |
|---|---|---|---|
| Eyelid margin skin excision (standard blepharoplasty) | Cases with ptosis, desire for crease formation | Access to levator aponeurosis and Müller muscle, crease formation possible | In thick skin, postoperative puffiness may persist |
| Subbrow skin excision (brow-scar blepharoplasty) | Thick skin, desire to minimize cosmetic change | Preserves thin skin near eyelid margin, less postoperative change in appearance | Scar remains under eyebrow, difficult to manipulate levator |
Caution: transient postoperative blepharoptosis
After surgery, transient blepharoptosis-like conditions may occur due to eyelid swelling. If mild blepharoptosis is present preoperatively, skin resection alone may not provide sufficient improvement. It is necessary to discuss with the patient preoperatively about combining blepharoptosis surgery.
There are two surgical techniques: eyelid margin skin resection (standard blepharoplasty) and subbrow skin resection (brow-scar blepharoplasty). In cases with blepharoptosis, the levator aponeurosis can be approached through eyelid margin resection, allowing simultaneous blepharoptosis surgery. In cases with thick skin, subbrow resection is cosmetically advantageous and results in less change in postoperative impression.
Since the underlying cause is age-related changes, skin laxity may progress again over years. However, functional and cosmetic improvements after surgery are generally good, and clinical need for reoperation is not common.
6. Pathophysiology and detailed mechanisms
Section titled “6. Pathophysiology and detailed mechanisms”Age-related changes in eyelid skin
Section titled “Age-related changes in eyelid skin”Eyelid skin undergoes the following changes due to aging and ultraviolet exposure:
- Skin thinning: Both the dermis and epidermis become thinner, reducing elasticity and tension.
- Degeneration of elastic fibers (elastin): Elastin fibers in the dermis break and degenerate, leading to loss of skin elasticity.
- Degeneration of collagen fibers: Degeneration and remodeling of collagen fibers reduce the tensile strength of the skin.
- Degeneration of the orbicularis oculi muscle: Atrophy and degeneration of the orbicularis oculi muscle reduce the supporting function of the eyelid.
- Decreased skin moisture content: Along with reduced skin barrier function, moisture content decreases, making the skin harder and more brittle.
These changes progress in combination, manifesting as sagging and wrinkles of the skin.
Changes in orbital tissues
Section titled “Changes in orbital tissues”In parallel with eyelid changes, age-related changes also occur in the orbital tissues.
- Relaxation of the orbital septum: Tissue relaxation of the orbital septum weakens the supporting structure of the upper eyelid.
- Atrophy of orbital fat: Atrophy of orbital fat tissue leads to a sunken eye appearance, creating a depression between the superior orbital rim and the eyeball.
- Anterior protrusion of orbital fat (fat herniation): In some cases, relaxation of the orbital septum allows orbital fat to protrude forward, forming a bulge in the upper eyelid.
Compensatory mechanisms and their adverse effects
Section titled “Compensatory mechanisms and their adverse effects”To compensate for visual field obstruction caused by excess skin, compensatory eyebrow elevation by the frontalis muscle occurs. This compensatory mechanism preserves the visual field in the short term but leads to the following problems in the long term:
- Formation of forehead wrinkles: Sustained contraction of the frontalis muscle creates deep wrinkles.
- Shoulder stiffness and neck pain: Hypertonicity of the frontalis muscle leads to tension in the neck and shoulder muscles.
- Tension-type headache in the forehead: Muscle tension in the forehead causes chronic headaches.
When compensatory eyebrow elevation is present, the apparent MRD-1 is maintained at a normal level, so evaluation without compensation is essential during examination.
7. Prognosis and course
Section titled “7. Prognosis and course”Postoperative outcomes
Section titled “Postoperative outcomes”Postoperative cosmetic and functional improvement is generally good.
- Improvement of visual field obstruction: Removal of excess skin widens the upper visual field and improves activities of daily living3.
- Reduction of lateral canthal dermatitis: Resolution of skin contact improves dermatitis at the lateral canthus.
- Reduction of shoulder stiffness and frontal headache: Compensatory eyebrow elevation becomes unnecessary, and relaxation of the frontalis muscle reduces shoulder stiffness and frontal headache4.
- Improvement of contrast sensitivity and visual quality: Significant improvement in contrast sensitivity has been reported, especially in the elderly, and visual quality may improve even without changes in visual acuity (decimal visual acuity)6.
Long-term course
Section titled “Long-term course”Since age-related changes are the underlying cause, skin laxity may slowly recur over years after surgery. However, recurrence to a clinically problematic degree is relatively rare.
If ptosis surgery is not combined in cases with concomitant blepharoptosis, ptosis symptoms may become apparent after temporary improvement following skin resection. Accurate preoperative assessment of concomitant ptosis and selection of an appropriate surgical technique are important for good long-term outcomes.
8. References
Section titled “8. References”Footnotes
Section titled “Footnotes”-
Patel BC, Malhotra R. Upper Eyelid Blepharoplasty. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024. [Updated 2023 Jul 24]. NBK537078. https://www.ncbi.nlm.nih.gov/books/NBK537078/ ↩ ↩2 ↩3
-
Bhattacharjee K, Misra DK, Deori N. Updates on upper eyelid blepharoplasty. Indian J Ophthalmol. 2017;65(7):551-558. doi: 10.4103/ijo.IJO_540_17. PMID: 28724810. PMCID: PMC5549405. https://pubmed.ncbi.nlm.nih.gov/28724810/ ↩ ↩2
-
Altin Ekin M, Karadeniz Ugurlu S. Prospective analysis of visual function changes in patients with dermatochalasis after upper eyelid blepharoplasty. Eur J Ophthalmol. 2020;30(5):978-984. doi: 10.1177/1120672119857501. PMID: 31203659. https://pubmed.ncbi.nlm.nih.gov/31203659/ ↩ ↩2
-
Simsek IB. Association of upper eyelid ptosis repair and blepharoplasty with headache-related quality of life. JAMA Facial Plast Surg. 2017;19(4):293-297. doi: 10.1001/jamafacial.2016.2120. PMID: 28253391. PMCID: PMC5815105. https://pubmed.ncbi.nlm.nih.gov/28253391/ ↩ ↩2
-
Lee D, Law V. Subbrow blepharoplasty for upper eyelid rejuvenation in Asians. Aesthet Surg J. 2009;29(4):284-288. doi: 10.1016/j.asj.2009.02.008. PMID: 19717059. https://pubmed.ncbi.nlm.nih.gov/19717059/ ↩ ↩2
-
Nalcı H, Hoşal MB, Gündüz ÖU. Effects of upper eyelid blepharoplasty on contrast sensitivity in dermatochalasis patients. Turk J Ophthalmol. 2020;50(3):151-155. doi: 10.4274/tjo.galenos.2019.95871. PMID: 32631001. PMCID: PMC7338742. https://pubmed.ncbi.nlm.nih.gov/32631001/ ↩
