Group A
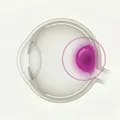
Definition: Retinal tumor ≤3 mm.
Features: No proximity to the macula or optic nerve. No seeding. Highest eye preservation rate.
Retinoblastoma is a malignant tumor derived from embryonic neural retina. 95% are diagnosed by age 5, and currently 70–80 cases occur annually in Japan. It occurs in 1 in 15,000–23,000 live births, accounting for 3.5% of childhood cancers.
Selective intra-arterial chemotherapy is also called superselective intra-arterial chemotherapy or chemosurgery. For intraocular retinoblastoma, a catheter is inserted directly into the ophthalmic artery to inject chemotherapy agents. It achieves high local drug concentrations in the eye that are unattainable with systemic chemotherapy while reducing systemic toxicity.
The history of selective intra-arterial chemotherapy is long, and it has evolved through several technical developments to its current form.
Currently, selective ophthalmic artery infusion chemotherapy is performed in more than 31 countries worldwide, and over 20 peer-reviewed papers have been published.
The conventional global standard treatment was a combination of systemic chemotherapy (chemoreduction) and local ocular therapy (transpupillary thermotherapy, retinal cryocoagulation). In recent years, selective ophthalmic artery infusion chemotherapy and intravitreal injection of anticancer drugs are becoming first-line treatments. In Japan, selective ophthalmic artery infusion chemotherapy is considered investigational, and the Alkeran injection (melphalan) used is not covered by insurance.
In Japan, selective ophthalmic artery infusion chemotherapy is considered investigational, and the Alkeran injection (melphalan) used is not covered by insurance. Although this treatment is performed in more than 20 countries worldwide, its implementation in Japan is limited to specialized facilities.
Early lesions are often asymptomatic and difficult to detect. The main symptoms that lead to detection are as follows.
A white retinal tumor grows endophytically or exophytically. The feeding vessels are retinal vessels, and dilated vessels are observed entering the tumor. When the tumor is large, necrosis and calcification occur internally, leading to retinal detachment, subretinal seeding, and seeding into the vitreous or anterior chamber.
As it progresses, it may be accompanied by severe inflammatory findings resembling cellulitis.
The International Classification of Retinoblastoma (ICRB) is widely used for staging.
Group A
Definition: Retinal tumor ≤3 mm.
Features: No proximity to the macula or optic nerve. No seeding. Highest eye preservation rate.
Group B
Definition: Retinal tumor >3 mm, or located near the macula or optic nerve.
Features: No seeding. Main target for TTT and brachytherapy.
Group C/D
Group C: Localized seeding (vitreous or subretinal).
Group D: Diffuse seeding (vitreous or subretinal). Advanced cases that are important targets for selective ophthalmic artery infusion chemotherapy.
Group E
Definition: Advanced cases where visual function cannot be preserved.
Features: Intraocular tumor filling the eye, anterior chamber invasion, neovascular glaucoma, etc. Enucleation is often recommended.
Retinoblastoma is caused by abnormalities in the RB1 gene, a tumor suppressor gene located on the long arm of chromosome 13 at band 14 (13q14). Knudson’s two-hit theory is the basis of the pathogenesis: the first mutation (genetic) and the second mutation (somatic) occur within a single cell, leading to uncontrolled cell division and malignancy.
The main differences between hereditary and non-hereditary forms are shown below.
| Classification | Frequency | Stage of Gene Mutation | Clinical Features | Second Cancers |
|---|---|---|---|---|
| Hereditary (germline) | Approximately 40% | Germline | Bilateral, multifocal, familial | High risk (15.7% at 20 years) |
| Non-hereditary (somatic) | Approximately 60% | Somatic level | Unilateral, solitary, sporadic | Same as general population |
The characteristics of hereditary (germline mutation) are as follows.
Approximately 40% are hereditary due to germline mutations and are inherited by offspring with a probability of 1/2. Bilateral cases always have germline mutations. On the other hand, about 60% are sporadic due to somatic mutations and are not inherited. In hereditary cases, the risk of secondary cancers is high, so long-term follow-up is important.
Intraocular lesions can be directly observed through transparent tissue, and clinical diagnosis is highly accurate. For eye-preserving treatment, diagnosis is based on clinical findings (biopsy carries a risk of tumor cell dissemination outside the eye).
The characteristics of the main examination methods are shown below.
| Examination method | Main purpose | Remarks |
|---|---|---|
| Fundus examination | Main diagnosis (vascularized white mass + calcification) | Mainstay of definitive diagnosis |
| Ultrasonography | Confirmation of intratumoral calcification and solid tumor | Note that calcification is scarce in children over 5 years old |
| MRI | Evaluation of optic nerve, choroid, and extraocular invasion | Also useful for screening for trilateral retinoblastoma |
| CT | Visualization of calcification | Radiation exposure. Less useful if MRI is available |
Bone marrow examination, cerebrospinal fluid examination, whole-body CT, and nuclear medicine studies are almost never positive in the intraocular localized stage. They are recommended only when extraocular disease is present, performed around the time of enucleation.
(1) Laser therapy (transpupillary thermotherapy, TTT)
Indicated for tumors up to about 3 mm in diameter. Direct irradiation with an infrared laser achieves local control in approximately 90% of cases. Start at 300 mW and adjust up to a maximum of 600 mW, with three additional sessions at monthly intervals. For macular tumors, chemotherapy is recommended first to avoid irreversible visual impairment.
(2) Cryotherapy
Tumors about 3 mm in size located at or anterior to the equator are targeted. The triple freeze-thaw method, which repeats freezing and thawing three times, is common, achieving local control in about 90% of cases.
(3) Brachytherapy
In Japan and Europe, 106Ru (beta source) is used, while 125I is used in North America. Indications include tumors with thickness ≤5 mm, diameter ≤15 mm, and located away from the optic disc. Local control is possible in 80–90% of cases. This treatment involves temporarily suturing a radioactive source onto the sclera over the tumor, requiring a special treatment room, which limits available facilities.
(4) Systemic Chemotherapy (Chemoreduction)
It is performed as first-line treatment for intraocular advanced tumors. Three-drug combination chemotherapy is widely used, but cure with chemotherapy alone is achieved in less than 10% of cases, necessitating consolidation with local treatment.
Example regimen repeated every 3–4 weeks for 2–6 cycles:
(5) Selective Ophthalmic Artery Infusion Chemotherapy
A catheter is used to directly administer the drug into the ophthalmic artery. This allows high-concentration delivery to the eye while reducing systemic drug exposure, thereby mitigating side effects such as bone marrow suppression. In Japan, this is an investigational treatment using Alkeran injection (melphalan) (not covered by insurance). It is performed in more than 20 countries worldwide.
The main drugs used in selective ophthalmic artery infusion chemotherapy are shown below (based on overseas reports).
| Drug name | Standard dose (per eye) | Main indications |
|---|---|---|
| Melphalan | 2.5–7.5 mg | First-line; most widely used |
| Topotecan | 0.3–0.4 mg | For cases unresponsive to melphalan monotherapy |
| Carboplatin | 15–30 mg | For cases unresponsive to multiple drugs; tandem therapy |
Used for vitreous seeding. Systemic chemotherapy and intra-arterial infusion have limited efficacy, so it is used in combination with them. In Japan, it is an investigational treatment using Alkeran injection (off-label). No effect is expected on retinal lesions.
(7) External beam radiation therapy
Until the 1990s, it was the mainstay of eye-preserving treatment, but orbital bone deformity and increased secondary cancers became evident, and it is now limited to cases uncontrollable by other treatments. Fractionated X-ray irradiation of 40–46 Gy. Stereotactic radiotherapy is not recommended due to difficulty in accurate irradiation in children and increased risk of secondary cancers from low-dose areas to surrounding tissues.
Enucleation is recommended in the following cases: when visual function cannot be expected, when glaucoma or cellulitis-like inflammation is present, when anterior chamber or iris invasion is present, or when extraocular invasion is suspected. Surgery involves long resection of the optic nerve and pathological examination of the enucleated eye.
The following is an overview of the procedure established at an overseas facility (Memorial Sloan Kettering Cancer Center).
Overseas, three main drugs are used: melphalan (most widely used), topotecan, and carboplatin. Melphalan shows the greatest effect against retinoblastoma cells in vitro. Topotecan is increasingly used in cases where melphalan alone is ineffective, and ophthalmic artery infusion achieves higher vitreous concentrations and lower systemic exposure than periocular injection. In Japan, Alkeran injection (melphalan) is used but is not covered by insurance.
The RB1 gene produces the RB1 protein, which is important for cell cycle control. There are two gene loci within a cell; a mutation in only one locus maintains function. When both loci are mutated, cell division becomes uncontrolled, leading to malignancy (Knudson’s two-hit hypothesis).
Histopathologically, differentiated type (characterized by rosettes and fleurettes, which are crown-like arrangements of malignant photoreceptor cells) and undifferentiated type (cells with scant cytoplasm and large chromatin-rich nuclei, often arranged around blood vessels) coexist within the tumor.
The pharmacological rationale for selective ophthalmic artery infusion chemotherapy is that direct injection into the ophthalmic artery achieves high local drug concentrations in the eye that are unattainable with systemic administration, while minimizing systemic toxicity. Melphalan is an alkylating agent that shows the greatest cytotoxic effect against cultured human retinoblastoma cells in clonogenic assays. In a pig model, topotecan administered via ophthalmic artery infusion achieved significantly higher intravitreal concentrations and longer exposure times compared to periocular injection, while maintaining low systemic exposure.
Gobin et al. (Memorial Sloan Kettering Cancer Center, 2006–2010) reported a non-randomized prospective study of 78 patients (95 eyes). At presentation, 73 eyes were RE Vb, 10 eyes RE Va, 4 eyes RE IV, and 8 eyes RE I–III. Fifty-two eyes (54.7%) had failed systemic chemotherapy or external beam radiotherapy. Catheterization success rate was 98.5% (255/259 attempts), mean number of infusions 3.1 (median 3, range 2–7). Two-year ocular survival (Kaplan-Meier estimate) was 70.0% for all eyes, 81.7% for treatment-naïve eyes, and 58.4% for previously treated eyes. Median follow-up 13 months (range 1–29 months): no deaths, 2 patients with metastasis (currently in remission), no cases of trilateral retinoblastoma. No eyes with RE I–IV required enucleation; 19 of 83 eyes with RE V were enucleated.
Abramson et al. (Memorial Sloan Kettering Cancer Center, 2006–2010) conducted a retrospective study of 67 patients (76 eyes) with vitreous and/or subretinal seeding. Forty-three eyes (56.5%) were previously treated, 29 eyes (38.1%) were treatment-naïve (primary treatment). Median follow-up for surviving eyes was 2.04 years (range 0.19–5.04). Two-year ocular preservation probability for treatment-naïve eyes: subretinal seeding only 83%, vitreous seeding only 64%, both 80%. For previously treated eyes: subretinal seeding only 50%, vitreous seeding only 76%, both 54%.
More recent series report further improvements in ocular preservation rates. In a 2018 report from Memorial Sloan Kettering Cancer Center, a series of 452 eyes treated from 2006 to 2017 showed a 2-year ocular survival rate of 96% (all eyes). A 2019 series from Wills Eye Hospital demonstrated ocular preservation rates of 88% for Group D and 100% for Group B/C. However, meta-analyses of all published selective ophthalmic artery infusion chemotherapy series show lower success rates for all eyes and advanced eyes (Group D/E), and the reasons for inter-institutional differences are unknown.
External beam radiotherapy avoided enucleation in only about 20–25% of RE V eyes (Reese et al.). Even the best results of chemoreduction for RE V eyes (Shields et al.) reported that at 5 years, 47% required external beam radiotherapy and 53% required enucleation. Selective ophthalmic artery infusion chemotherapy achieves higher enucleation avoidance rates than these modalities, particularly showing efficacy in treatment-naïve eyes with subretinal seeding.
At the Bascom Palmer Eye Institute (Miami, Florida), a total of 26 injections were performed in 15 patients (17 eyes), all with RE Vb (International Classification of Retinoblastoma Group D) and all with vitreous seeding, nearly all refractory to multi-agent chemotherapy. Success rate 100%, eye preservation rate 76.5% (13 of 17 eyes), mean follow-up 8.6 months.
Cardiac glycosides such as digoxin have been shown to have antitumor activity against retinoblastoma in vitro and in vivo. In clinical use via intra-arterial injection, moderate responses have been reported at the case report level. On the other hand, methotrexate showed no effect with two doses of 6 mg and 12 mg.
It varies by institution and disease stage. In the initial study at Memorial Sloan Kettering Cancer Center (2006–2010), the 2-year ocular survival rate was 70.0% for all eyes and 81.7% for primary treatment eyes. A more recent series from the same center (2006–2017, 452 eyes) showed a 96% ocular survival rate with a median follow-up of about 2 years. However, meta-analyses of all published series show lower success rates for all eyes and advanced eyes, with differences between institutions.