First-Degree Burn
Gross findings: Erythema only. No blisters.
Pain: Present (+).
Prognosis: Heals within a few days.
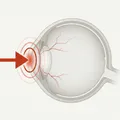
Ocular burn is a thermal injury caused by contact of the eye with high-temperature liquids, solids, or flames. Common causes include splashes of hot water or cooking oil, molten metal, fireworks, and flames. Ocular burns are broadly classified into eyelid burns and ocular burns. When facial burns involve the eyelids and ocular surface, visual function may be impaired, requiring ophthalmological treatment.
At the time of injury, reflexive eyelid closure and Bell’s phenomenon (a defensive upward eye movement) reduce direct corneal burns. However, burns from molten metal can cause high temperatures to reach deep into the cornea, leading to persistent epithelial defects, corneal stromal melting, corneal thinning, and in severe cases, corneal perforation, often resulting in significant visual impairment.
The eyelid skin is 0.3–0.6 mm thick, among the thinnest in the body. Lacking subcutaneous fat, it is prone to deep burns, and the orbicularis oculi muscle and tarsal plate may also be damaged. After scar formation, functional problems such as trichiasis, entropion, ectropion, and lagophthalmos may persist.
Ophthalmic involvement is observed in 7.5–27% of patients admitted to burn units. The most common mechanism is fire/flame (46%), followed by scalding (32%). Other causes include cooking oil, molten metal splashes, fireworks, and flames. In a retrospective study of 125 cases by Cabalag et al. (2015), the severity of corneal damage and eyelid burns were identified as independent risk factors for early and late complications (Reference 4).
At the time of injury, Bell’s phenomenon and the blink reflex are activated, so direct damage to the cornea is relatively rare. However, with molten metals, high temperatures can penetrate deep into the cornea, leading to severe damage that progresses from persistent epithelial defects to stromal melting and perforation. Since 7.5–27% of burn unit inpatients have ocular involvement, an ophthalmological evaluation should always be performed at the time of injury.
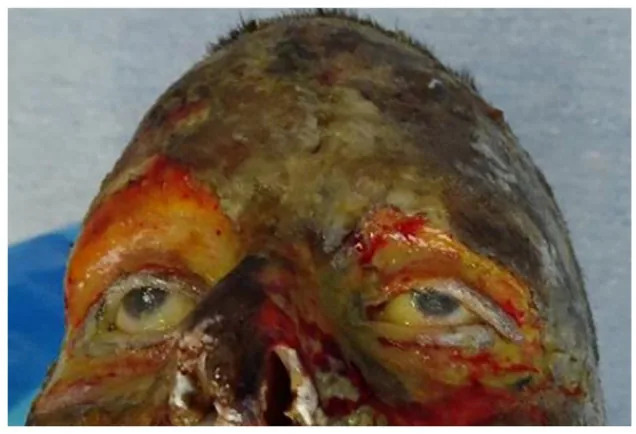
Acute ocular burns are classified into first to third degrees.
| Classification | Findings |
|---|---|
| First-degree burn | Conjunctival hyperemia, superficial corneal opacity |
| Second-degree burn | Conjunctival edema, corneal epithelial necrosis |
| Third-degree burn | Conjunctival necrosis, corneal necrosis/carbonization |
In ocular burns of second degree or higher, similar to chemical burns, subsequent complications such as persistent corneal epithelial defect, corneal opacity, corneal perforation, corneal endothelial damage, iritis, secondary glaucoma, symblepharon, pseudopterygium, and scarring of the ocular surface may occur.
First-Degree Burn
Gross findings: Erythema only. No blisters.
Pain: Present (+).
Prognosis: Heals within a few days.
Second-Degree (Superficial)
Gross findings: Blisters form. The dermis under the blister is red.
Pain: Severe (++).
Prognosis: Heals in 1 to 2 weeks.
Second-Degree (Deep)
Gross findings: Blisters form. The dermis under the blister is white.
Pain: Severe (++).
Prognosis: Requires 3 to 4 weeks.
Third-Degree Burn
Macroscopic findings: Waxy hardening. Dry, leathery appearance.
Pain: Absent (±). Due to nerve destruction.
Prognosis: More than 1 month. Spontaneous epithelialization cannot be expected.
The Kinoshida classification (Grade I–IV) is used to assess the severity of corneoconjunctival disorders. Grades I and II, in which corneal epithelial stem cells are not damaged, have a good prognosis and do not result in visual impairment if there is no stromal damage. Grade IIIa and above, where the limbus is damaged, leads to persistent corneal epithelial defects and conjunctival scarring, resulting in a poor prognosis. Grades IIIb and IV require amniotic membrane transplantation or corneal epithelial transplantation.
| Grade | Main findings | Prognosis |
|---|---|---|
| I | Conjunctival hyperemia, mild corneal epithelial defect | Good (no visual impairment) |
| II | Conjunctival ischemia, corneal opacity | Good (no visual impairment) |
| IIIa or higher | Severe ischemia, total corneal opacity, limbal damage | Poor (scarring, persistent epithelial defect) |
| IIIb to IV | Extensive limbal necrosis / total corneal damage | Poor (ocular surface reconstruction required) |
Burns from molten metal follow a particularly severe course. The high heat reaches deep into the cornea, causing persistent epithelial defects, corneal stromal melting, and corneal thinning, which in the worst case can lead to corneal perforation. Often accompanied by severe visual impairment, long-term ocular surface management is required.
Eyelid burns often involve not only the eyelids but also burns to other parts of the body. In particular, burns from the neck to the face in children can cause airway obstruction due to edema from the burn, and careful observation is necessary for 24 to 48 hours after injury.
Molten metal is at a high temperature, and its heat penetrates deep into the cornea. This causes persistent epithelial defects, corneal stromal melting, and corneal thinning, which can eventually lead to corneal perforation. In superficial burns, the blink reflex provides some protection, but with molten metal, this protection is insufficient.
Understanding the characteristics of each cause helps in predicting severity and initial management.
| Cause | Characteristics | Points to note |
|---|---|---|
| Hot water / cooking oil | Frequent household accidents. Widespread entry into the ocular surface. | Common in children and the elderly |
| Molten metal | Factory/occupational accidents. High temperature penetrates deep into the cornea. | Confirming occupational history is important. |
| Fireworks/gas explosion | May be accompanied by high-energy trauma. | Intraocular or orbital foreign bodies must be ruled out. |
| Flame | Accounts for 46% of burn unit admissions. | Be aware of concurrent systemic burns and airway burns. |
Factors affecting depth include exposure intensity (temperature), exposure duration, and skin thickness. Higher temperature, longer contact time, and thinner skin/tissue result in deeper burns.
Concurrent chemical burns should also be considered. After combustion, gunpowder becomes alkaline and may cause both thermal and chemical injuries simultaneously.
Diagnosis is based on history of injury and visual inspection. Obtain detailed information about the causative substance, contact time, and contact area.
Key points of initial evaluation:
Comprehensive severity assessment:
Combine the depth classification of eyelid burns (grades I–III), the severity classification of ocular burns (grades 1–3), and the Kinoshida classification of corneoconjunctival damage (grades I–IV) to determine overall severity. Grade IIIa or higher suggests limbal stem cell deficiency, requiring long-term ocular surface management.
If high-velocity trauma or explosion is involved, perform imaging studies to rule out intraocular or intraorbital foreign bodies.
Immediately after injury, apply local cooling with cold water as soon as possible. Use tap water or a water bag to cool the area promptly to prevent burn extension, reduce pain, and suppress edema.
If facial burns or airway burns are present, systemic management including respiratory management is necessary. When the oral and facial areas are involved, securing the airway is the top priority.
Use a lid speculum to carefully observe the anterior segment, and remove any adherent foreign bodies or necrotic corneal and conjunctival epithelium.
For first- and second-degree eyelid burns, conservative treatment is performed to prevent infection, reduce inflammation, and promote epithelialization. Maintaining a moist environment is important for wound healing. The wound should be left open, and antibiotic eye ointment should be applied to keep it moist. Wound dressings may also be useful in some cases.
The burn treatment guidelines suggest the use of basic fibroblast growth factor (bFGF) preparations for second-degree burns due to their usefulness as wound healing promoters.
For third-degree burns, spontaneous epithelialization cannot be expected, so skin grafting should be considered. If there is a tendency for eyelid ectropion making closure difficult, tarsorrhaphy may be considered as a temporary measure until grafting to prevent exposure keratitis. In a review by Malhotra et al. (2009), early ophthalmological examination and prophylactic ocular surface lubrication are principles of eyelid burn management, and early surgical intervention is recommended for eyelid retraction causing corneal exposure (Reference 2). An analysis of 66 cases over 10 years at Alfred Hospital by Spencer et al. (2002) also showed that prophylactic ocular surface lubrication and early ophthalmology referral contributed to avoiding surgery (Reference 3).
Treatment of ocular burns follows that of chemical burns. Administer antibiotic eye drops and oral antibiotics, steroid eye drops and oral steroids, and sodium hyaluronate eye drops. If epithelial defects persist, serum eye drops, amniotic membrane transplantation (amniotic membrane graft, amniotic membrane cover), and tarsorrhaphy are also effective.
If corneal limbal epithelium remains (Grade I-II), use antibiotics and 0.1% betamethasone eye drops to reduce inflammation and promote epithelialization. For Grade IIIb and IV, amniotic membrane transplantation, limbal transplantation (auto or allo), and keratoepithelioplasty (KEP) are required. A systematic review and meta-analysis by Klifto et al. (2019) showed that acute surgical intervention (e.g., amniotic membrane transplantation) had superior outcomes in visual prognosis, healing of corneal epithelial defects, and improvement of limbal ischemia compared to non-surgical intervention (Reference 1).
Steroid treatment for ocular burns is selected according to severity.
| Severity | Treatment |
|---|---|
| Severe (total corneal epithelial defect, tissue necrosis) | Methylprednisolone 125 mg IV 1-2 times, betamethasone 1 mg/day or prednisone 10 mg/day orally for 1-2 weeks, betamethasone eye drops 4 times daily |
| Moderate (severe hyperemia, partial corneal epithelial defect) | Prednisone 5-10 mg/day orally for several days, betamethasone eye drops 4 times daily |
| Mild | Betamethasone eye drops 2-4 times daily |
For all severities, combine with antibacterial eye drops or ointment to prevent infection.
Patients with extensive burns who have undergone massive fluid resuscitation require monitoring for orbital compartment syndrome (OCS). In a study by Sullivan et al. (2006), intraocular pressure rose to 30 mmHg or higher in 5 of 13 severe burn patients requiring massive fluid resuscitation, necessitating lateral canthotomy (Reference 5). A systematic review by Makarewicz et al. (2024) also identified extensive burn area, facial burns, and massive fluid resuscitation as major risk factors for OCS, with lateral canthotomy and inferior cantholysis established as standard treatment (Reference 6). If orbital compartment syndrome is suspected, perform emergency treatment without waiting for imaging diagnosis.
Treatment in the cicatricial phase is similar to that for chemical injuries. For cases with limbal stem cell deficiency, amniotic membrane transplantation, limbal transplantation, or KEP may be necessary. Attention should also be paid to lagophthalmos due to eyelid deformity, which may require oculoplastic procedures. Long-term management addresses complications such as trichiasis, entropion, ectropion, lagophthalmos, and blepharophimosis.
For skin grafting (eyelid reconstruction), full-thickness autograft is the first choice. The incidence of ectropion after full-thickness grafting is 30%, compared to 88% after split-thickness grafting.
It is a basic fibroblast growth factor (bFGF) preparation, with trafermin being a representative product name. It promotes fibroblast proliferation and migration, accelerating wound healing. The burn care guidelines recommend its use in combination with antibiotic eye ointment for second-degree burns.
Burns cause tissue damage through direct thermal protein denaturation and tissue necrosis, combined with subsequent inflammatory reactions. Jackson’s three zones (Jackson 1947) are widely known as a concept describing the concentric structure of burn tissue.
Zone of Coagulation
Characteristics: Area of maximal damage. Protein coagulation occurs.
Outcome: Irreversible tissue loss. Cannot be salvaged.
Zone of Stasis
Characteristics: Intermediate zone with reduced tissue perfusion.
Outcome: Potentially salvageable. However, it may progress to complete necrosis due to hypotension, infection, or edema.
Zone of Hyperemia
Characteristics: Outermost layer with increased tissue perfusion.
Outcome: Always recovers unless severe sepsis occurs.
Reflex eyelid closure and Bell’s phenomenon (upward rotation of the eyeball) at the time of injury result in relatively less direct damage to the cornea. However, these protective mechanisms are not perfect, and protection becomes insufficient when contact time is long or with high-energy heat sources such as molten metal.
When molten metal solidifies, it retains high temperature and adheres to the corneal surface, continuously conducting thermal energy to deeper layers. This causes irreversible damage not only to the corneal epithelium but also to the stroma and endothelium. The slower the cooling rate, the greater the thermal penetration into deeper tissues.
As scar formation after eyelid burns progresses over several months, a chain of secondary complications occurs: lagophthalmos, corneal exposure, corneal dryness, and corneal infection. Additionally, cicatricial contracture leads to trichiasis, entropion, and ectropion, becoming major sequelae requiring long-term management.
The orbit is a rigid bony compartment. In extensive burns, massive fluid resuscitation causes third-space shifting of intravascular volume, peaking 6 to 12 hours after injury. Positive pressure ventilation also worsens edema. When intraorbital pressure exceeds perfusion pressure, ischemic optic neuropathy and retinal ischemia occur, leading to irreversible visual impairment.
Biodegradable temporizing matrix: A synthetic dermal matrix that forms neodermis as a precursor to thin autografts. Research is progressing as an alternative to conventional temporary dressings.
Cultured oral mucosal epithelial transplantation: The ocular surface can be covered with epithelium immediately after surgery, providing rapid anti-inflammatory effects. The goal is not visual improvement but stabilization of the ocular surface, and application to Grade IIIb–IV cases is being attempted.
Boston Ocular Surface Prosthesis: Used for corneal protection in cases of extensive tissue defects where amniotic membrane use is difficult and eyelid suturing is challenging. Its application to general ocular surface diseases is also being considered.
Early full-thickness autograft: Previously, waiting until scar stabilization was common, but early use of full-thickness autografts, amniotic membrane, and various flaps has been reported to reduce ophthalmic morbidity.