First-Degree Burn
Macroscopic findings: Erythema only. No blisters.
Pain: Present (+).
Prognosis: Heals within a few days.
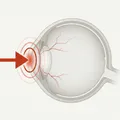
Eyelid burns are burns that occur on the skin of the eyelids. They are caused by heat, chemicals, or electricity.
Some form of ocular involvement is seen in 7.5–27% of burn unit inpatients. Among injury mechanisms, fire/flame accounts for 46% (most common), followed by scalding at 32%. Other causes include cooking oil, molten metal splashes, fireworks, and flames.
The thickness of eyelid skin is 0.3–0.6 mm, the thinnest in the body. Because it lacks subcutaneous fat, it easily progresses to deep burns. On the other hand, the blink reflex, Bell’s phenomenon, and defensive arm movements work together to relatively reduce direct injury to the eyeball.
In children, the epidermis and dermis of the skin are thin, and the impact of liquid burns is greater. In facial and neck burns, there is a risk of airway obstruction due to airway edema within 24–48 hours after injury, requiring caution.
Due to the blink reflex, Bell’s phenomenon, and defensive arm movements, direct injury to the eyeball is relatively rare. However, 7.5–27% of patients admitted to burn units have ocular involvement, so an ophthalmological evaluation is always necessary at the time of injury.
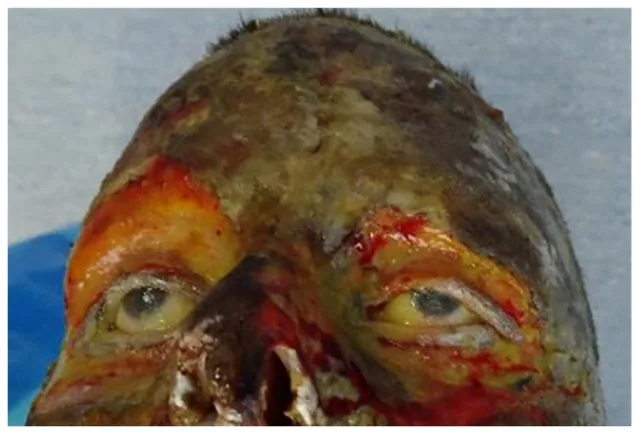
Symptoms vary according to the depth of the burn.
Burn depth is classified as follows based on macroscopic appearance, pain, and prognosis.
First-Degree Burn
Macroscopic findings: Erythema only. No blisters.
Pain: Present (+).
Prognosis: Heals within a few days.
Second degree (superficial)
Macroscopic findings: Blisters form. The dermis under the blister is red.
Pain: Severe (++).
Prognosis: Heals in 1 to 2 weeks.
Second degree (deep)
Macroscopic findings: Blisters form. The dermis under the blister is white.
Pain: Severe (++).
Prognosis: Requires 3 to 4 weeks.
Third degree burn
Macroscopic findings: Waxy hardening. Dry, leather-like appearance.
Pain: Absent (±). Due to nerve destruction.
Prognosis: More than 1 month. Spontaneous epithelialization is not expected.
Jackson’s three zones (Jackson 1947) is a concept describing the concentric structure of burn tissue. The central zone of coagulation is an area of irreversible tissue loss due to protein coagulation, and the outer zone of stasis is a zone of reduced perfusion that can be salvaged. The outermost zone of hyperemia is an area of increased perfusion that always recovers unless severe sepsis occurs.
Findings suggestive of orbital compartment syndrome include rock-hard eyelids, proptosis, decreased vision, relative afferent pupillary defect (RAPD), ophthalmoplegia, and elevated intraocular pressure (above 35–40 mmHg). Particular caution is needed in patients with extensive burns who have undergone massive fluid resuscitation.
Corneal evaluation uses fluorescein test strips and cobalt blue light. Recording the presence or absence of Bell’s phenomenon is useful for predicting later lagophthalmos. Ocular surface evaluation should include observation of the bulbar conjunctiva, fornix conjunctiva, and palpebral conjunctiva.
In third-degree burns, the heat destroys the subcutaneous nerves, resulting in loss of sensation. The absence of pain does not indicate a mild injury; on the contrary, it signifies the deepest damage.
Among the causes, fire/flame is the most common (46%), followed by hot water (32%). Other causes include cooking oil, molten metal splash, fireworks, and flames.
Three factors influence depth:
Attention should also be paid to concurrent chemical burns. Gunpowder after combustion becomes alkaline and can cause both thermal and chemical injuries simultaneously.
High-risk groups include children (thin skin), the elderly (comorbidities), and patients with extensive burns. Thresholds for the risk of developing orbital compartment syndrome include fluid volume exceeding 5–6 mL/kg/%TBSA or an Ivy Index of 250 mL/kg or more.
The eyelid skin is 0.3–0.6 mm thick, the thinnest in the body, and lacks subcutaneous fat. Therefore, even with the same thermal stimulus, heat easily reaches deeper layers, making it prone to deep burns.
Diagnosis is based on history of injury and visual inspection. Obtain detailed information about what (causative agent) and under what circumstances (contact time, temperature) the injury occurred.
Eyelid evaluation: Observe the eyelids and eyelashes with the naked eye or low magnification.
Ocular surface evaluation: Check the extent of conjunctival injection and ischemia, and the extent of corneal edema, opacity, and epithelial defect. Evert the eyelids and observe the entire conjunctiva including the fornix.
Corneal evaluation: Evaluate corneal epithelial defects using fluorescein strips and cobalt blue light.
Intraocular pressure measurement: In patients who have undergone massive fluid resuscitation, measure intraocular pressure periodically for 48–72 hours after injury.
Imaging: In high-velocity trauma or explosion, perform imaging to rule out intraocular or orbital foreign bodies.
Photographic documentation: Photograph the depth and extent of the burn at the initial evaluation.
Check for contact lenses: Do not overlook contact lens wear at the time of injury.
The Kinoshida classification (Grade I–IV) is used to evaluate corneoconjunctival damage.
| Grade | Main Findings | Prognosis |
|---|---|---|
| I | Mild conjunctival hyperemia and corneal epithelial defect | Good |
| II | Conjunctival ischemia and corneal opacity | Good |
| IIIa or higher | Severe ischemia and total corneal opacity | Poor |
Grades I–II have a good prognosis, while grade IIIa or higher is considered poor.
Initial cooling: Immediately after injury, cool the local area with tap water or an ice pack. The goal is to prevent expansion of the burn area, reduce pain, and suppress edema.
Airway assessment: If the orofacial area is involved, securing the airway is the top priority.
Lubrication: Apply frequent and copious lubricants within 24 hours of admission. This is essential for corneal protection due to decreased tear production, blink reflex, and eyelid mobility.
Antibiotics: Antibiotic eye drops or ointments are used concurrently to prevent infection.
Grade I/II (Conservative treatment): The goal is infection prevention, anti-inflammation, and promotion of epithelialization.
Grade III (Skin grafting): Since spontaneous epithelialization is not expected, skin grafting should be considered.
When eyelid closure is difficult: Tarsorrhaphy should be considered as a temporary measure to prevent exposure keratitis.
If ocular burns are present, steroids are used.
| Severity | Treatment |
|---|---|
| Severe (total corneal epithelial defect, tissue necrosis) | Methylprednisolone 125 mg IV 1–2 times, betamethasone 1 mg/day or prednisone 10 mg/day orally for 1–2 weeks, betamethasone eye drops 4 times daily |
| Moderate (severe hyperemia, partial corneal epithelial defect) | Prednisone 5–10 mg/day orally for several days, betamethasone eye drops 4 times daily |
| Mild | Betamethasone eye drops 2-4 times daily |
For any severity, combine with antibacterial eye drops or ointment to prevent infection.
If orbital compartment syndrome is suspected, perform emergency treatment without waiting for imaging.
Full-thickness autograft: First choice for eyelid reconstruction. Less contraction and lower risk of ectropion. The incidence of ectropion after full-thickness graft is 30%, compared to 88% after split-thickness graft.
Temporary coverage: Cadaveric allograft or biodegradable temporary dressing (synthetic dermal matrix) may also be used.
3-week rule: Deep partial-thickness wounds that do not re-epithelialize within 3 weeks should be considered for excision and grafting.
Corneal protection: Amniotic membrane, tarsorrhaphy, or Boston Ocular Surface Prosthesis are used. If epithelial defect persists, consider amniotic membrane transplantation, corneal epithelial transplantation (limbal transplantation), or cultured mucosal epithelial sheet transplantation.
Long-term complications may include the following:
For cicatricial entropion, eyelash management and entropion surgery are performed.
Full-thickness autograft is the first choice. It contracts less and has an ectropion rate of only 30%, compared to 88% after split-thickness grafting. However, if donor site availability is limited, temporary dressings or split-thickness grafts may be combined.
Burns trigger the release of multiple inflammatory mediators, leading to vasodilation, pain, and edema. Jackson’s three zones (1947) are a basic concept explaining the spatial distribution of tissue damage.
Zone of Coagulation
Characteristics: Area of maximal damage. Protein coagulation occurs.
Outcome: Irreversible tissue loss. Cannot be salvaged.
Stasis Zone
Characteristics: Intermediate area with reduced tissue perfusion.
Outcome: Salvageable. However, hypotension, infection, or edema can lead to complete necrosis.
Hyperemia Zone
Characteristics: Outermost layer with increased tissue perfusion.
Outcome: Always recovers unless severe sepsis occurs.
The orbit is a rigid bony compartment. In extensive burns, massive fluid resuscitation leads to third-space fluid shift peaking 6–12 hours after injury. Positive pressure ventilation also worsens edema. When intraorbital pressure exceeds perfusion pressure, ischemic optic neuropathy and retinal ischemia occur.
During blinking, the eyelid margin skin is relatively protected from injury. However, as scar formation progresses over months after burns, trichiasis, entropion, ectropion, and lagophthalmos develop. Scar contracture is a major sequela requiring long-term management.
Biodegradable Temporizing Matrix: A synthetic dermal matrix that forms neodermis as a precursor to thin autografts. Research is progressing as an alternative to conventional temporary dressings.
Cultured oral mucosal epithelial transplantation: The ocular surface can be covered with epithelium immediately after surgery, providing a rapid anti-inflammatory effect. The goal is not visual improvement but stabilization of the ocular surface.
Boston Ocular Surface Prosthesis: Used for corneal protection in cases of extensive tissue defects where amniotic membrane use is difficult and eyelid suturing is challenging.
Early full-thickness autograft: Previously, it was common to wait until scar stabilization, but there are reports that early use of full-thickness autografts, amniotic membrane, and various flaps reduces ophthalmic morbidity.