Iridodialysis
Site of injury: Tear of the iris at its attachment to the ciliary body
Main effects: Pupillary deviation, light scattering, monocular diplopia
Slit-lamp findings: Crescent-shaped or semilunar gap
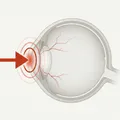
Iridodialysis is a condition in which the iris root is torn and detached from the ciliary body and scleral spur. The iris root is the thinnest part of the iris and is prone to tearing due to stretching forces during blunt trauma.
Iridodialysis
Site of injury: Tear of the iris at its attachment to the ciliary body
Main effects: Pupillary deviation, light scattering, monocular diplopia
Slit-lamp findings: Crescent-shaped or semilunar gap
Angle recession
Site of injury: Tear between the circular and longitudinal muscles of the ciliary body
Main effects: Intraocular pressure fluctuation, long-term risk of glaucoma
Slit-lamp findings: Widening of the angle, enlargement of the ciliary body band
Cyclodialysis
Site of injury: Detachment of the ciliary body from the sclera
Main effect: Ocular hypotony (formation of abnormal aqueous outflow pathway)
Slit-lamp findings: Direct observation with gonioscopy, confirmed by UBM
| Classification | Characteristics | Main symptoms |
|---|---|---|
| Small tear | Narrow tear with limited effect on pupil shape | Few subjective symptoms, sometimes asymptomatic |
| Large tear | Associated with pupillary deviation | Decreased vision, monocular diplopia, photophobia |
It occurs as a complication of blunt ocular trauma. The causative external forces include sports balls, fists, traffic accidents, flying objects, and many others. It is often accompanied by hyphema and angle recession, requiring comprehensive evaluation.
If the detachment is small and there are no symptoms, observation is often sufficient. However, if the detachment is large with pupillary distortion, or if monocular diplopia and photophobia persist, surgical repair is necessary. Also, since hyphema and angle recession are often present, long-term follow-up of intraocular pressure is essential.
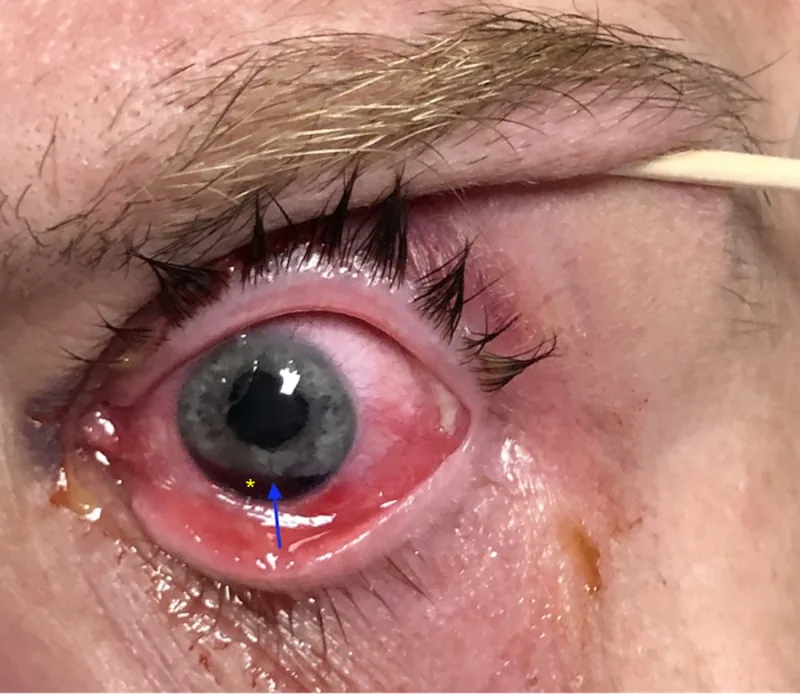
Photophobia occurs due to excessive light entering the eye from increased pupil size or distortion. When the tear is extensive and causes pupillary distortion, it can lead to decreased vision and monocular diplopia. Decreased vision is often due to increased higher-order aberrations or associated traumatic cataract and vitreous hemorrhage.
| Finding | Characteristics |
|---|---|
| Iridodialysis | Crescent-shaped or semilunar cleft (observed with slit lamp) |
| Pupillary distortion | Distortion toward the side of the tear, asymmetric pupil shape |
| Hyphema | Suggests angle recession. Visibility reduced depending on amount of bleeding. |
| Vitreous prolapse | Seen when zonular rupture is present. |
Slit-lamp examination reveals a crescent-shaped or semilunar cleft. Vitreous prolapse may be present due to zonular rupture. If hyphema is present after blunt trauma, suspect angle recession or cyclodialysis.
This is the most common cause. Typical mechanisms include direct impact to the eye from a ball (baseball, tennis, squash, etc.), fist, tree branch, or flying object.
Iris root damage occurs when the iris prolapses through a corneoscleral laceration. If iris incarceration is present at the wound, the pupil is displaced toward that direction.
Iris injury during cataract surgery can also be a cause1). Small pupil is the most important risk factor for intraoperative iris injury1). Systemic use of alpha-1 adrenergic receptor blockers (e.g., tamsulosin, used for benign prostatic hyperplasia or hypertension) can cause intraoperative floppy iris syndrome (IFIS), increasing the risk of iris prolapse1). The incidence of IFIS or iris prolapse is reported as 0.5–2.0%, and iris/ciliary body injury as 0.6–1.2%1).
Slit-Lamp Microscopy
Confirmation of iridodialysis: Observed as a crescent-shaped iris defect. Transillumination can detect a defect in light transmission at the iris root 2).
Pupil evaluation: Record pupil diameter, shape, and direction and degree of deviation. Check the presence or absence of light reflex and response to mydriatics.
Associated injuries: Evaluate for phacodonesis, anterior capsule rupture, and vitreous prolapse.
Gonioscopy and Imaging
Gonioscopy: Evaluate the increased distance from the iris root to the scleral spur and widening of the ciliary body band 2). Comparison with the fellow eye is important. Perform 1–2 weeks after resolution of hyphema.
Ultrasound biomicroscopy (UBM) and anterior segment OCT: Useful for observing from the iris root to the ciliary body. Small cyclodialysis may be difficult to detect by gonioscopy alone 2).
In the acute phase with hyphema, it is often difficult to fully assess the condition. After the hemorrhage resolves, repeat slit-lamp and gonioscopy to evaluate the extent of iridodialysis, degree of angle recession, and presence of cyclodialysis. Depending on the severity of trauma, perform fundus examination, OCT, or ultrasound B-scan to check for associated retinal or vitreous injuries.
First, prioritize conservative treatment for hyphema. Use rest and mydriatics (atropine eye drops) to calm uveitis and promote absorption of hyphema. Use steroid eye drops (e.g., betamethasone phosphate 0.1%) to suppress inflammation. If the iridodialysis is small and asymptomatic, surgery is not required.
Iridosuture is indicated when the iris is widely separated with pupillary deviation and any of the following is present:
It is known that when the pupil diameter exceeds 4 mm, higher-order aberrations significantly increase, leading to decreased visual acuity. If mydriasis of 6 mm or more remains after IOL insertion despite the use of miotics and iris traction, pupilloplasty is performed simultaneously with cataract surgery.
Preoperatively, the iris is stretched with forceps in the anterior chamber to simulate the suture position. This maneuver itself also has a miotic effect. Sutures of 9-0 or 10-0 prolene (polypropylene) are used.
| Procedure | Features |
|---|---|
| Modified Siepser Sliding Knot technique | The iris is grasped through a side port with a width of 2-3 mm and tied outside the eye. The procedure is relatively simple. Uses 9-0/10-0 prolene suture. |
| Single-pass Four-throw (SFT) technique | The suture end is passed through the pulled-out suture loop four times and tied. The intra- and extra-anterior chamber maneuvers are completed in one step. |
| McCannel technique | A long needle is inserted through the main incision to pierce the iris and limbus in one motion. Standard tying outside the eye is possible. An easy-to-understand technique. |
| Iris cerclage | Continuous suture around the iris for extensive dialysis. Intra-anterior chamber manipulation is complex and highly difficult. |
| Pick-up needle (30G thin-wall needle) technique | Used when passing the suture is difficult. The iris is punctured from the corneal side with a pick-up needle, which locks with a long needle. Allows accurate suture placement. |
The goal is to reduce the pupil diameter to approximately 4 mm or less and reposition the pupil to the center.
The iris suture procedure itself is often completed within several tens of minutes. If performed simultaneously with cataract surgery or IOL insertion, additional time is added. The surgical time varies depending on the technique and the extent of iris damage or dialysis.
If the iris trauma is isolated, pupilloplasty often improves photophobia and visual acuity. Visual prognosis is often good, but if there are concomitant retinal damage, vitreous hemorrhage, traumatic cataract, or optic nerve injury, improvement with iris repair alone is limited. Final postoperative visual acuity depends on the presence and severity of associated injuries.
When blunt external force is applied to the eye, intraocular pressure rises rapidly. The corneal limbus is stretched, and aqueous humor moves posteriorly and into the angle, exerting strong stretching force on the iris. The iris root is the thinnest part of the iris, making it most vulnerable to this stretching force, resulting in rupture at the root—iris root dialysis.
If the injury extends from the iris root to the scleral side, it takes a stepwise injury pattern. If a tear occurs between the circular (Müller) and longitudinal (Brücke) muscles of the ciliary body, angle recession occurs, leading to intraocular pressure fluctuations. If the ciliary body detaches from the sclera on the scleral side, cyclodialysis occurs, creating a new pathway for aqueous humor to flow from the anterior chamber into the suprachoroidal space, resulting in hypotony.
When the blood-aqueous barrier is disrupted by microscopic tissue damage, inflammatory cells migrate into the anterior chamber, causing traumatic iritis. Hyphema results from vascular injury in the angle. Breakdown products of red blood cells (e.g., hemosiderin) can obstruct the trabecular meshwork and impede aqueous outflow, leading to transient intraocular pressure elevation (ghost cell glaucoma).
Angle recession not only causes acute intraocular pressure elevation but also increases the long-term risk of developing glaucoma. Since late-onset glaucoma (angle recession glaucoma) may develop years to decades after the injury, long-term intraocular pressure management and regular examinations are important.
When angle recession is present, angle recession glaucoma may develop years to decades after the injury. Regular intraocular pressure measurements and visual field tests are essential. If elevated intraocular pressure goes unnoticed and untreated, irreversible visual field damage may progress. Even without symptoms after trauma, it is important to continue ophthalmic check-ups at least once a year.
Intraocular iris suturing using a very small curved needle (1.5 mm) and a dedicated needle holder has been reported. Compared to conventional extraocular manipulation with a long needle, this technique allows more precise suturing and causes less iris damage within the anterior chamber. It also has the advantage of minimizing damage to the corneal endothelium even when the needle is vertically positioned in the anterior chamber.
Artificial iris (iris prosthesis for aniridia) has accumulated clinical experience abroad as an option for extensive iris damage or cases unsuitable for iris suturing, but it is not yet approved in Japan. Iris-diaphragm intraocular lenses (IOLs) have also been developed and may become a new treatment option for aniridia or severe iris damage.