Medial transconjunctival
Frequency of use: 59%, the most common.
Advantages: Shortest route. Cosmetically superior.
Disadvantages: Strabismus risk, longer surgery time.

Optic nerve sheath decompression (ONSD), also called optic nerve sheath fenestration (ONSF), refers to the same surgical procedure. A slit or window (fenestration) is created in the dura mater surrounding the optic nerve, allowing CSF from the subarachnoid space to drain, thereby locally reducing pressure on the optic nerve. CPT code 67570 is assigned.
The most common indication is idiopathic intracranial hypertension (IIH), with about 25% of cases refractory to medical treatment requiring surgical intervention. Other indications may include cerebral venous sinus thrombosis, cryptococcal meningitis, all-trans retinoic acid (ATRA)-induced pseudotumor cerebri1), and moyamoya disease4).
Epidemiology (IIH): The annual incidence of IIH in the United States is 1.15 per 100,000. It is higher in women (1.97 per 100,000) than in men (0.36 per 100,000), with the highest rate in those aged 18–44 years (2.47 per 100,000). The prevalence of IIH is rising with the global increase in obesity.
| Year | Event |
|---|---|
| 1853 | Turck and Coccius first report papilledema |
| 1872 | De Wecker first reports ONSD (as treatment for neuroretinitis) |
| 1964 | Hayreh demonstrated resolution of papilledema after optic nerve sheath fenestration |
| 1973 | Galbraith & Sullivan developed the medial transconjunctival approach |
| 1988 | Tse et al. extended the lateral orbital approach |
| 2001 | Pelton & Patel reported the superomedial eyelid crease approach |
Both refer to the same surgical procedure. The difference is only in terminology; both involve creating a slit or window in the optic nerve dura to drain CSF. The confusion arises because the English terms ONSD (optic nerve sheath decompression) and ONSF (optic nerve sheath fenestration) are translated into Japanese as “decompression surgery” and “fenestration surgery,” respectively.
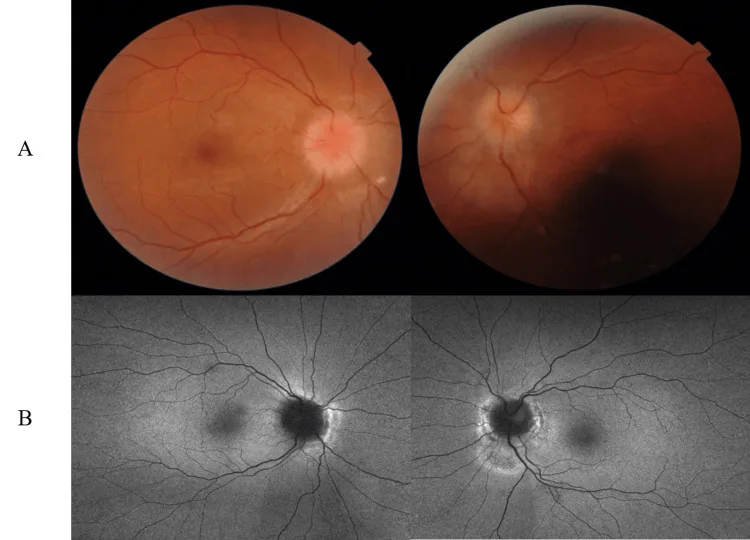
Intracranial hypertension (especially IIH) indicated for ONSD presents with the following symptoms.
Characteristics of fulminant IIH: Rapid vision loss within weeks, pRNFL >300 μm, and mean CSF opening pressure on first lumbar puncture of 54.1 cm H₂O (range 29–70) are characteristic. Visual recovery is poor when the Humphrey visual field mean deviation is < -7 dB.
The most common risk factors for IIH, for which ONSF is most frequently performed, are listed below.
ONSF may also be indicated for other causes of increased intracranial pressure (such as moyamoya disease 4), cerebral venous sinus thrombosis, infections, and space-occupying lesions).
In addition to IIH, indications may include cerebral venous sinus thrombosis, cryptococcal meningitis, increased intracranial pressure associated with moyamoya disease, and ATRA (all-trans retinoic acid)-induced pseudotumor cerebri syndrome. In cases of moyamoya disease, ONSF has been performed for refractory increased intracranial pressure, with reports of visual recovery.
All of the following items must be met.
Differential diagnosis: Venous sinus thrombosis, anemia, obstructive sleep apnea, drug-induced (tetracyclines, vitamin A, etc.), endocrine abnormalities. When accompanied by acute visual loss, differentiation from malignant hypertension, meningitis, optic neuritis (MOG, NMOSD, etc.), and optic nerve infiltration (leukemia, lymphoma) is important.
Indications: When headache is mild but there is marked papilledema with progressive or threatening vision loss. The main goal is to protect vision; it is ineffective for headache treatment.
Surgical approaches: Three main approaches are used.
Medial transconjunctival
Frequency of use: 59%, the most common.
Advantages: Shortest route. Cosmetically superior.
Disadvantages: Strabismus risk, longer surgery time.
Superomedial eyelid margin incision
Frequency of use: 31%.
Advantages: Shortest surgery time. No microscope needed.
Disadvantages: Longer route, risk of ptosis.
Lateral orbitotomy
Frequency of use: 10%, the least common.
Advantages: Good visualization of the optic nerve.
Disadvantages: Risk of ciliary ganglion injury.
Surgical outcomes (meta-analysis: 19 studies, 1159 observations)3):
| Outcome measure | Improvement rate | 95% CI |
|---|---|---|
| Visual acuity improvement | 41.09% | 29–55% |
| Visual field improvement | 76.34% | 61–87% |
| Papilledema improvement | 97% | 84–100% |
The visual field improvement rate with the transconjunctival approach (86%) is significantly higher than with other approaches (57%) (p=0.018). There is no significant difference in visual acuity improvement rates between approaches (p=0.715)3).
Bilateral effect from unilateral surgery: Unilateral ONSF also improves contralateral papilledema. In a 2-year follow-up of 9 patients (all female) with idiopathic intracranial hypertension after unilateral ONSF, bilateral visual improvement was confirmed in all cases2).
Complication risk: Overall 10–15%. The most serious complication is vision loss due to central retinal artery occlusion or central retinal vein occlusion (1–2%). Other reported complications include diplopia (22.2%), subconjunctival hemorrhage (44.4%), and orbital cellulitis (11.1%), but these are often transient2).
Venous sinus stenting may be useful in drug-refractory cases with proven venous sinus stenosis and pressure gradient. Postoperative antiplatelet therapy for 6 months is required. The level of evidence is still low, and an RCT (shunt vs. stent) is ongoing in the UK.
When obesity is the main cause, high success rates have been reported even in cases resistant to conventional treatment. Remission has been reported with a 3–15% weight reduction. Not recommended for fulminant type.
Unilateral ONSF has been confirmed to improve contralateral papilledema. In a 2-year follow-up study of 9 patients with idiopathic intracranial hypertension, bilateral visual improvement was reported in all cases. The expected protective effect on the contralateral eye after unilateral surgery is one of the important features of this procedure.
Clinical recurrence has been reported in 32% of patients. If recurrence occurs, additional surgical treatment (reoperation, shunt surgery, or stent placement) may be necessary. Regular ophthalmologic examinations for follow-up are important.
The subarachnoid space of the optic nerve is continuous with that of the central nervous system. When elevated ICP is transmitted along the entire length of the optic nerve to the optic disc, damage occurs through the following mechanisms.
The pattern of vision loss begins with enlargement of the blind spot in the early stage and progresses to peripheral visual field defects.
The mechanism by which ONSF protects the optic nerve can be divided into two stages.
Important point: ONSF does not lower ICP. It only exerts a local protective effect on the optic nerve, so no effect on systemic symptoms such as headache can be expected.
The exact mechanism of intracranial hypertension in idiopathic intracranial hypertension is not fully understood. Dysregulation of CSF dynamics and involvement of metabolic and hormonal factors are considered. Idiopathic intracranial hypertension is increasingly recognized as a systemic metabolic disease independent of obesity, and androgen dysregulation has also been suggested.
ATRA is a vitamin A derivative that stimulates RAR receptors in the choroid plexus, increasing CSF production. Impaired CSF absorption at the arachnoid granulations is also speculated to be involved.
Prokop et al. (2024) conducted a systematic review and meta-analysis of 19 studies and 1159 observations, comprehensively evaluating visual outcomes of ONSF3). They reported a visual acuity improvement rate of 41.09% (95% CI: 29–55%), visual field improvement rate of 76.34% (95% CI: 61–87%), and papilledema improvement rate of 97% (95% CI: 84–100%). Surgical delay beyond 6 months after diagnosis significantly worsened visual field outcomes (OR 0.06, 95% CI 0.005–0.70). Clinical recurrence was observed in 32%.
Latif et al. (2023) performed unilateral medial transconjunctival ONSF in 9 patients (all female, mean age 24 years) with idiopathic intracranial hypertension and followed them for 2 years 2). Preoperative BCVA (logMAR) was 0.5±0.28 in the better eye and 1.0±0.57 in the worse eye. Improvement at 1 week postoperatively (better eye 0.27±0.32, p=0.001) was maintained at 2 years (better eye 0.30±0.30, p=0.002). Bilateral effects from unilateral surgery were confirmed in all cases. Headache improvement and successful medication tapering were achieved in 66.67%.
Hokazono et al. (2023) treated a 32-year-old woman with ATRA (45 mg/m²)-induced pseudotumor cerebri syndrome (lumbar puncture opening pressure 42 cm H₂O) with a combination of ATRA dose reduction, acetazolamide 2 g/day, and right eye ONSF 1). Complete recovery was achieved at 6 months, with 20/20 vision in both eyes, normal visual fields, resolution of papilledema, and resolution of abducens nerve palsy.
Barh et al. (2021) performed right eye ONSF in a 13-year-old girl with intracranial hypertension (opening pressure 75 cm H₂O) associated with moyamoya disease (left ICA stenosis + left MCA occlusion) 4). She was refractory to conservative treatment (mannitol, acetazolamide, topiramate), but at 1 month postoperatively, vision improved to 3/60 in the right eye and 6/24 in the left eye, and bilateral papilledema resolved. At 6 months, vision was maintained at 6/36 in the right eye and 6/24 in the left eye.
This is a new approach that offers the advantages of minimal invasiveness, shorter operative time, and no need for muscle disinsertion. It is expected to reduce tissue damage, but standardization has not yet been achieved 3).
Hokazono K, Cunha LP, Preti RC, Zacharias LC, Monteiro MLR. Optic nerve sheath fenestration as adjuvant treatment for severe pseudotumor cerebri syndrome induced by all-trans retinoic acid. Case Rep Ophthalmol. 2023;14:326-330.
Latif S, Rizwan A, Khan AA, Zahra S. Optic nerve sheath fenestration for salvaging acutely threatened vision in Idiopathic Intracranial Hypertension - A two-year completed follow up. Pak J Med Sci. 2023;39(6):1853-1857.
Prokop K, Opchowska A, Siekiewicz A, Lisowski L, Mariak Z, Lyso T. Effectiveness of optic nerve sheath fenestration in preserving vision in idiopathic intracranial hypertension: an updated meta-analysis and systematic review. Acta Neurochir. 2024;166:476.
Barh A, Mukherjee B, Ambika S. Optic nerve sheath fenestration for visual rehabilitation in moyamoya disease. Saudi J Ophthalmol. 2020;34:223-226.