Cat scratch disease (most common)
Pathogen: Bartonella henselae (gram-negative bacillus)
Vector: Cats (especially kittens), dogs, cat fleas, sand flies
Incubation period: 3 days to 3 weeks

Parinaud oculoglandular syndrome (POGS) is a clinical syndrome characterized by unilateral granulomatous follicular conjunctivitis and ipsilateral regional lymphadenopathy (preauricular, parotid, submandibular, cervical) 1.
The most common cause is cat scratch disease (CSD). CSD is a zoonotic infection caused by the gram-negative bacillus Bartonella henselae, which enters through cat scratches, bites, or flea bites. POGS occurs in 5–7% of CSD patients 2,3. A retrospective study of ocular bartonellosis at a tertiary hospital in Malaysia found POGS in approximately 23% of confirmed cases, with a tendency to occur more often in younger individuals 2.
Although many microorganisms can cause this syndrome, the majority are due to cat scratch disease, and the prognosis is generally good. Both systemic and ocular lesions often resolve spontaneously within 1–2 months 1,3.
B. henselae is mainly transmitted through “hand-to-eye contact” when a person touches their eye with a hand that has been scratched by a cat. Direct infection from a cat scratch is rare in the oculoglandular form. Aerosolized cat flea feces have also been proposed as a route of transmission.
Painful swelling of ipsilateral preauricular, postauricular, submandibular, and cervical lymph nodes is characteristic1. Younger patients tend to present with cervical lymphadenopathy, while those aged 15 years and older tend to have inguinal or axillary lymphadenopathy.
In addition to POGS, CSD can cause the following ocular complications:
In ocular bartonellosis overall, small white retinal lesions are the most common (82.6%), followed by neuroretinitis (47.8%)2.
Cat scratch disease (most common)
Pathogen: Bartonella henselae (gram-negative bacillus)
Vector: Cats (especially kittens), dogs, cat fleas, sand flies
Incubation period: 3 days to 3 weeks
Tularemia
Pathogen: Francisella tularensis (gram-negative coccobacillus)
Vector: Rabbits, squirrels, ticks, mosquitoes
Incubation period: 2–5 days (rarely up to 3 weeks)4
Sporotrichosis
Pathogen: Sporothrix schenckii (dimorphic fungus)
Source of infection: Soil, plant organic matter, infected animals
Endemic areas: Tropical and subtropical regions such as Brazil and Peru5
Other causes include tuberculosis, syphilis, coccidioidomycosis, sarcoidosis, herpes simplex, chancroid, leprosy, listeriosis, mumps, etc.
Simply owning a cat does not cause infection. Direct contact such as being scratched by a cat carrying B. henselae is necessary. Kittens have a high carriage rate, and fleas are vectors, so regular flea control is an effective preventive measure.
Inquiry about animal contact (cats, dogs, rabbits, ticks), outdoor activities, travel history, and occupational history is most important.
| Cause | Recommended Test | Diagnostic Criteria |
|---|---|---|
| Cat scratch disease | Serology (IgM, IgG) | IgM ≥ 1:20, IgG ≥ 1:256 |
| Tularemia | Serology | Titer > 1:128 suggests infection |
| Sporotrichosis | Culture (Sabouraud agar) | Identification of fungus |
CSD is a self-limiting disease, and treatment is primarily supportive.
POGS due to cat scratch disease is self-limiting, and in immunocompetent patients it often resolves spontaneously within 1–2 months. However, disappearance of granulomas may take several weeks, and lymphadenopathy may take several months to resolve. In prolonged cases, antibiotic therapy may be considered.
B. henselae is a Gram-negative small bacillus that is a fastidious obligate intracellular bacterium. The bacteria enter through cat scratches or bites and form a red papule (primary lesion) at the inoculation site 1–2 weeks after injury. After another 1–2 weeks, swelling and tenderness of the regional lymph nodes appear.
Ocular infection mainly occurs through hand-to-eye contact with contaminated hands. B. henselae reaching the conjunctiva proliferates beneath the conjunctival epithelium and induces a granulomatous inflammatory response. Inflammation spreads to the ipsilateral regional lymph nodes (preauricular, parotid, submandibular), causing painful lymphadenopathy.
Neurotransmitters related to corneal innervation (such as substance P and CGRP) are not major factors in this disease; direct bacterial invasion and the host cell-mediated immune response are central to the pathology.
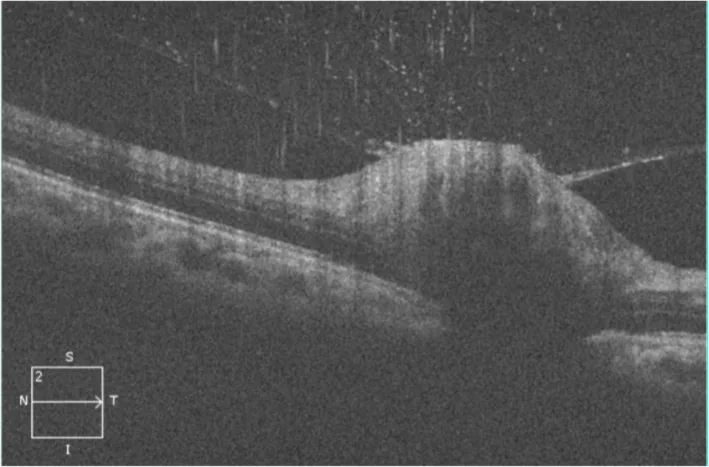
In neuroretinitis associated with CSD, edema extending from the optic disc to the macula occurs, and a characteristic star figure (macular star) appears. Hematogenous dissemination of B. henselae is thought to cause direct bacterial invasion of the optic nerve and retina.
Dixon MK, Dayton CL, Anstead GM. Parinaud’s Oculoglandular Syndrome: A Case in an Adult with Flea-Borne Typhus and a Review. Tropical Medicine and Infectious Disease. 2020;5(3):126. PMID: 32751142. PMCID: PMC7558689.
Tey MS, Govindasamy G, Vendargon FM. The clinical spectrum of ocular bartonellosis: a retrospective study at a tertiary centre in Malaysia. Journal of Ophthalmic Inflammation and Infection. 2020;10:31. PMID: 33191467. PMCID: PMC7667203.
Sabir S, Daley SF, Huang B. Cat Scratch Disease. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025. Bookshelf ID: NBK482139.
Nagy KI, Pribelszki E, Sira Á, Fullajtár B, Rácz T, Major T. Francisella tularensis Infection Causing Parinaud Oculoglandular Syndrome. The American Journal of Case Reports. 2024;25:e944321. PMID: 38941282. PMCID: PMC11332965.
Ferreira CP, Nery JAC, de Almeida ACO, Ferreira LC, Corte-Real S, Conceição-Silva F. Parinaud’s oculoglandular syndrome associated with Sporothrix schenckii. IDCases. 2014;1(3):38–39. PMID: 26955523. PMCID: PMC4762793.
Bass JW, Freitas BC, Freitas AD, et al. Prospective randomized double blind placebo-controlled evaluation of azithromycin for treatment of cat-scratch disease. Pediatric Infectious Disease Journal. 1998;17(6):447–452. PMID: 9655532.