Topical Medications
Steroid eye drops: Basic treatment for anterior uveitis
Mydriatics and cycloplegics: Prevention and treatment of posterior synechiae
Antibiotics and antimicrobials: Causal treatment for infectious uveitis
The eye is a highly unique organ. It is easily examined externally, and drugs can be administered directly in the form of topical eye drops. Uveitis is an inflammatory disease of the iris, ciliary body, and choroid, and eye drops are the first-line treatment for anterior segment involvement.
This guide categorizes and explains the eye drops frequently used in the management of uveitis into the following categories.
Topical Medications
Steroid eye drops: Basic treatment for anterior uveitis
Mydriatics and cycloplegics: Prevention and treatment of posterior synechiae
Antibiotics and antimicrobials: Causal treatment for infectious uveitis
Medications for Complications
Intraocular pressure-lowering drugs: Management of secondary glaucoma and steroid-induced glaucoma
However: Prostaglandin analogs and pilocarpine are generally avoided in uveitis
Nonsteroidal anti-inflammatory drugs: Alternative when inflammation is mild and stable
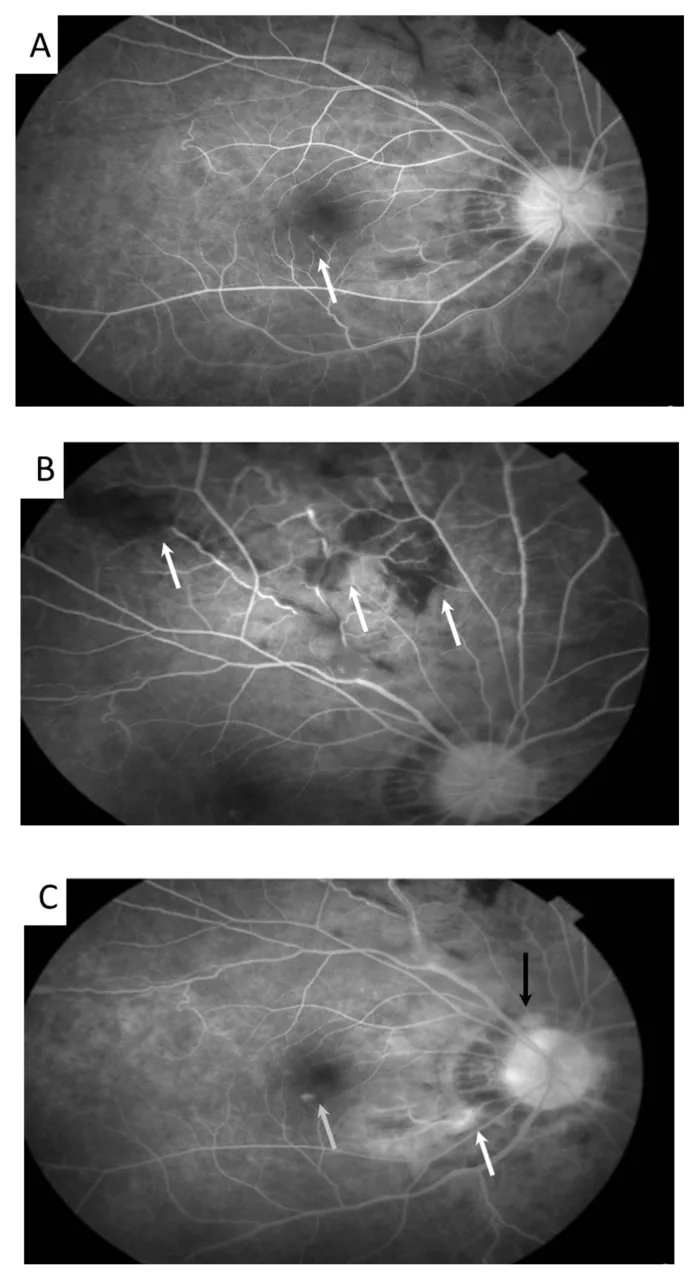
Uveitis presents with the following subjective symptoms:
| Finding | Details |
|---|---|
| Keratic precipitates (KP) | Fine to mutton-fat (sarcoidosis, tuberculosis) |
| Anterior chamber flare and cells | Graded 1+ to 4+ for inflammation severity |
| Posterior synechiae | Prevent or break with mydriatics |
| Vitreous opacities | Indicators of intermediate or posterior uveitis |
| Secondary glaucoma | Elevated intraocular pressure → hypotensive eye drops (caution in drug selection) |
Uveitis is classified into anterior, intermediate, posterior, and panuveitis based on the location. The choice of topical treatment depends on this classification and the degree of inflammation.
When severe inflammation occurs in the anterior chamber, posterior synechiae (adhesion of the iris to the anterior lens surface) can develop. Mydriatic agents relax the ciliary muscle and pupillary sphincter, preventing and breaking these adhesions. A combination of tropicamide and phenylephrine (Mydrin P) is widely used.
Uveitis is broadly divided into infectious and non-infectious types.
Causes of infectious uveitis:
Causes of non-infectious uveitis:
Diagnosis is based on detailed evaluation of the anterior and posterior segments using slit-lamp microscopy. Serological tests (including PCR) are performed to rule out infectious uveitis.
The following screening is recommended before starting immunomodulatory therapy. 1)
Inflammation severity is assessed based on the SUN (Standardization of Uveitis Nomenclature) Working Group classification. 1)
In infectious uveitis, steroids may be used alongside treatment of the cause (antibiotics, antivirals, etc.) to control postoperative inflammation. However, steroid monotherapy without adequate infection control may worsen the infection. Always prioritize treatment of the underlying cause.
The mainstay of local treatment for uveitis is steroid eye drops. In order of increasing potency: fluorometholone → loteprednol → rimexolone → prednisolone → difluprednate.
| Drug Name | Concentration | Characteristics/Uses | Main Side Effects |
|---|---|---|---|
| Fluorometholone (FML) | — | For mild inflammation | Increased intraocular pressure (low) |
| Loteprednol (Lotemax) | 0.2, 0.5, 1% | Low risk of increased intraocular pressure | Increased intraocular pressure (low) |
| Prednisolone (Pred Forte) | 0.12, 1% | Standard treatment for intraocular inflammation | Cataract, increased intraocular pressure |
| Difluprednate (Durezol) | 0.05% | Potent. For severe cases | Cataract, increased intraocular pressure |
About tapering
Tapering of topical steroids (eye drops) is not mandatory. If the treatment duration is less than 3–4 weeks, tapering is unnecessary regardless of the dose. Tapering is recommended only when steroids are used for more than 3–4 weeks, to promote recovery of the hypothalamic-pituitary-adrenal axis. This concept applies to systemic steroids; topical eye drops pose almost no risk of adrenal suppression.
While anterior chamber inflammation is present, continue instilling mydriatic eye drops to prevent posterior synechiae.
| Drug name | Duration of effect | Concentration | Main use |
|---|---|---|---|
| Atropine | 7–12 days | 0.5–3% | Severe uveitis, hyphema |
| Scopolamine | 3–7 days | 0.25% | Atropine allergy |
| Homatropine | 1–3 days | 2–5% | Useful for uveitis |
| Cyclopentolate | About 1 day | — | Uveitis and refraction testing |
| Tropicamide | 6–24 hours | 0.5, 1% | Fundus examination under mydriasis |
Tropicamide/phenylephrine combination (Mydrin P) is widely used in Japan as a standard mydriatic for anterior chamber inflammation. A typical prescription is one drop at bedtime.
Uveitis is often complicated by secondary glaucoma and steroid-induced glaucoma. For elevated intraocular pressure, beta-blockers and carbonic anhydrase inhibitors are preferred.
| Drug class | Representative drugs | Characteristics |
|---|---|---|
| Beta-blockers | Timolol, betaxolol | Suppress aqueous humor production. Twice daily |
| Carbonic anhydrase inhibitors | Dorzolamide, brinzolamide | Suppress aqueous humor production. Three times daily |
| Alpha agonists | Brimonidine | Suppress aqueous humor production and promote outflow. Contraindicated in infants |
Intraocular pressure-lowering drugs to avoid in uveitis:
For intermediate, posterior, or panuveitis that is inadequately controlled with topical steroid eye drops, systemic therapy should be considered.
The standard first-line treatment is oral prednisolone (initial dose 1 mg/kg/day, tapered within 4 weeks). 1) For steroid-dependent cases or those with difficulty tapering steroids, conventional immunomodulatory drugs or biologics are added.
First-line conventional immunomodulatory drugs (by disease):1)
Biologics:1)
Adalimumab is used as first-line therapy by 97.7% of specialists. The VISUAL I/II trials established the efficacy of TNF-α inhibition, and it is approved by the FDA and EMA. Combination therapy with methotrexate and adalimumab is used by 84.0% of specialists. 1)
For short-term use of less than 3–4 weeks, tapering is not necessary. The European Society of Endocrinology guidelines also state that “for use of less than 3–4 weeks, tapering is not required regardless of dose.” However, if used for more than 3–4 weeks, tapering is necessary to allow recovery of the hypothalamic-pituitary-adrenal axis. With topical eye drops, the risk of systemic adrenal suppression is almost nonexistent, but gradual reduction is safer than abrupt discontinuation.
The mechanisms of intraocular pressure elevation in uveitis include:
Since treatment strategies differ for each mechanism, it is important to accurately evaluate the mechanism of intraocular pressure elevation by gonioscopy.
Mechanism of action of mydriatics and cycloplegics:
Anticholinergic drugs (e.g., atropine, tropicamide) relax the ciliary muscle and pupillary sphincter, causing mydriasis and cycloplegia. Relaxation of the ciliary muscle reduces pain and photophobia, and also decreases contact between the posterior iris and anterior lens surface, preventing posterior synechiae. Adrenergic receptor agonists (e.g., phenylephrine) contract the dilator pupillae muscle and assist mydriasis.
Mechanism of action of topical steroids:
Topical steroids suppress anterior segment inflammation by inhibiting inflammatory cytokine production and immune cell migration. Difluprednate, with high potency, has high receptor affinity and shows excellent efficacy against severe anterior segment inflammation. However, it also carries a high risk of cataract induction and intraocular pressure elevation, so the principle is to select the minimum necessary potency.
Local treatment flow for anterior uveitis
Step 1: Steroid eye drops (select potency according to inflammation severity)
Step 2: Mydriatic agents (e.g., Mydrin P) to prevent posterior synechiae
Step 3: If intraocular pressure rises, use beta-blockers and carbonic anhydrase inhibitors (prostaglandin analogs and pilocarpine are contraindicated)
Step 4: If control is insufficient → systemic steroids or sub-Tenon injection
Local additional treatment for intermediate and posterior uveitis
Sub-Tenon injection: Triamcinolone (40 mg/mL) 0.5 mL
Indications: Macular edema, vitreous opacity, posterior pole inflammation
Systemic therapy: Systemic steroids are the mainstay for intermediate and posterior uveitis
Immunomodulatory drugs: Added for cases with poor control for 6 months or more
Advances in biologic agents have greatly changed the treatment of uveitis. The widespread use of adalimumab has been established, and evidence for many disease types has accumulated from the VISUAL I/II and SYCAMORE trials. 1)
Future challenges include the following: