Findings of preseptal cellulitis
Proptosis: None
Eye movement: Normal (no pain on movement)
Visual acuity: Normal
RAPD: Negative
CT: Only preseptal soft tissue swelling
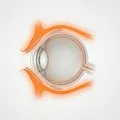
Preseptal cellulitis is an acute infectious inflammation of the eyelids and periorbital soft tissues anterior to the orbital septum. The orbital septum is a fibrous membrane that extends from the tarsal plates to the orbital rim, acting as a barrier that physically prevents the spread of infection into the orbit.
It corresponds to Chandler grade I (1970) in the severity classification of orbital infections, and is classified as Group 1 (preseptal or periorbital inflammation) in the Chan classification. Infection of the soft tissues posterior to the orbital septum is orbital cellulitis (Group 2 or higher), which is clearly distinguished from this condition.
Compared to orbital cellulitis, it is more common and generally milder. Sinusitis (especially ethmoid sinusitis), eyelid trauma, insect bites, and facial skin infections are the main triggers, and it is a disease that commonly occurs in children. In adults, it may also develop after dental infections or trauma.
Preseptal cellulitis does not involve proptosis, ophthalmoplegia, or vision loss. If any of these findings appear, progression to orbital cellulitis (Chandler grade II or higher) should be suspected, and CT imaging should be performed for evaluation. Checking eye movements, RAPD testing, and visual acuity measurement are essential examination items for differentiation.
In preseptal cellulitis, the following findings are “absent,” which helps differentiate it from orbital cellulitis.
| Finding | Preseptal Cellulitis | Orbital Cellulitis |
|---|---|---|
| Proptosis | Absent | Present |
| Ophthalmoplegia | Absent | Present |
| Eye pain (pain on eye movement) | None (usually) | Present |
| Decreased visual acuity | None | May be present |
| RAPD (relative afferent pupillary defect) | Negative | May be positive |
| CT findings | Only preseptal soft tissue swelling | Intraorbital inflammation/abscess |
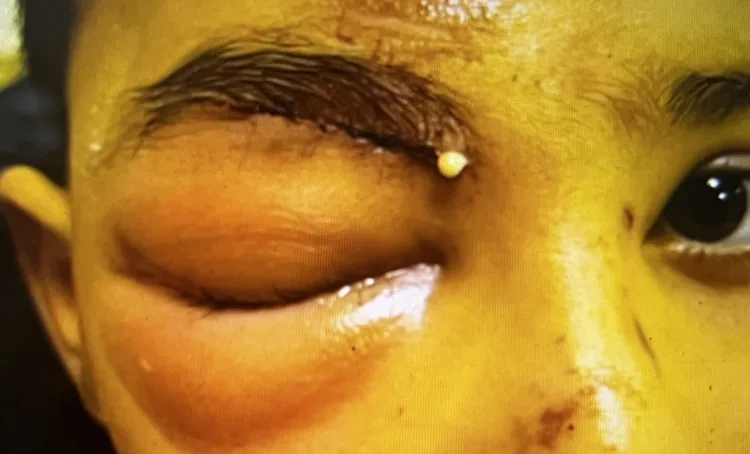
Findings of preseptal cellulitis
Proptosis: None
Eye movement: Normal (no pain on movement)
Visual acuity: Normal
RAPD: Negative
CT: Only preseptal soft tissue swelling
Findings of orbital cellulitis
Proptosis: Present
Eye movement: Impaired (pain on movement)
Visual acuity: May be decreased
RAPD: May be positive
CT: Intraorbital inflammation or abscess formation
If any of the following findings newly appear during treatment, immediately suspect progression to orbital cellulitis (Group 2 or higher) and repeat CT imaging. 1)
Preseptal cellulitis can develop through several routes.
Insect bites on the eyelid or face can cause preseptal cellulitis. Bacteria normally present on the skin (Staphylococcus aureus, Streptococcus, etc.) can enter through the bite wound and cause infection. If after an insect bite the eyelid redness and swelling rapidly increase and are accompanied by fever, suspect progression to cellulitis and seek medical attention.
The diagnosis of preseptal cellulitis is primarily based on clinical findings. The examination systematically checks the following:
If proptosis, ocular motility restriction, visual loss, or positive RAPD are absent, clinical differentiation from orbital cellulitis is possible.
CT (orbit and paranasal sinuses) is the mainstay of diagnosis. Contrast-enhanced CT is preferred to evaluate the extent of inflammation anterior and posterior to the septum and the presence of sinusitis.
In mild cases with low suspicion of sinusitis and a clear trigger such as trauma or insect bite, clinical diagnosis and initiation of antibiotic therapy may be considered, with CT performed if no improvement within 48 hours.
| Test | Purpose |
|---|---|
| Blood tests (CRP, WBC) | Assessment of inflammation severity and monitoring |
| Blood culture | Rule out bacteremia (high fever, severe cases) |
| Nasal and wound culture | Identify causative organism and antibiotic sensitivity (if possible) |
| Differential diagnosis | Key differentiating features |
|---|---|
| Orbital cellulitis | Proptosis, motility restriction, vision loss → confirm with CT |
| Hordeolum (stye) | Localized eyelid mass, no fever, limited course |
| Allergic eyelid edema | No redness, no fever, rapid resolution, recurrent |
| Orbital tumor | Chronic course, mass on imaging, no response to antibiotics |
| Dacryoadenitis | Localized to lateral upper eyelid, tenderness, often after cold in chronic type |
| Contact dermatitis | History of eye drops or cosmetics use, non-infectious, no fever |
Treatment for preseptal cellulitis is stratified into outpatient management and inpatient management based on severity.
Criteria for Outpatient Management
General condition: Good, no high fever (below 38°C)
Degree of swelling: Limited to localized eyelid swelling
Age: Older children to adults (children over 1 year old and adults)
Follow-up: Able to return for re-evaluation within 24-48 hours
Other: No immunodeficiency, good medication adherence
Criteria for Hospitalization
General condition: High fever (≥38.5°C) · Poor general condition
Degree of swelling: Extensive swelling · Rapid progression
Age: Infants (especially under 1 year old)
Insufficient improvement: No improvement within 24–48 hours after starting outpatient treatment
Other: Immunocompromised · Difficulty taking oral medication · Presence of complications
Mild cases/Outpatient management (oral antibiotics)
| Drug | Dosage | Indication |
|---|---|---|
| Cefdinir (Cefzon®) 100 mg | 3 times daily orally (Children: 9 mg/kg/day divided into 3 doses) | Mild cases/Outpatient management |
| Amoxicillin/Clavulanate (Augmentin®) 250 mg | 3 times daily orally | Mild cases/Outpatient management (alternative) |
| Clindamycin | Children: 10 mg/kg/dose, 3 times daily, oral | Penicillin allergy cases |
Moderate to severe cases / Inpatient management (intravenous antibiotics)
| Drug | Dosage | Indication |
|---|---|---|
| Ceftriaxone | 50–100 mg/kg/day, IV | Moderate to severe / Inpatient |
| Vancomycin | IV (when considering MRSA, dose adjustment based on weight) | Suspected MRSA / Severe cases |
| Ampicillin/Sulbactam | IV | When anaerobic coverage is needed |
In MRSA-endemic areas or cases unresponsive to outpatient treatment, consider switching to broad-spectrum coverage including vancomycin.
If sinusitis (especially ethmoid sinusitis) is confirmed, otolaryngological intervention is necessary. In adults, otolaryngological treatment for sinusitis is often required. If medical therapy fails, consider functional endoscopic sinus surgery (FESS) in collaboration with an otolaryngologist.
Reassessment within 24 to 48 hours after starting treatment is mandatory. Check the following points:
If improvement is insufficient or worsening occurs (new onset of proptosis or ophthalmoplegia), suspect progression to orbital cellulitis (Group 2 or higher) and immediately repeat CT and transition to inpatient management. 2)
Mild cases with good general condition, mild fever, and localized eyelid swelling can be managed as outpatients with oral antibiotics. However, reassessment within 24 to 48 hours after starting treatment is necessary to confirm improvement. If worsening occurs (proptosis, ophthalmoplegia, or vision loss), switch to inpatient treatment.
The appearance of proptosis, restriction of eye movement (ophthalmoplegia), decreased vision, worsening headache, and altered consciousness are dangerous signs indicating progression to orbital cellulitis or a more severe form. If these occur, immediate re-examination is required, along with repeat CT and urgent evaluation by a specialist.
The orbital septum is a fibrous membrane that extends from the tarsal plate to the arcus marginalis of the orbital rim, functioning as a barrier at the anterior orbit. This membrane physically prevents the spread of infection into the orbit, making it difficult for preseptal infections to extend into the orbital cavity.
In children, the orbital septum is thin and immature, so they are more prone to progression to orbital cellulitis compared to adults. Additionally, the lamina papyracea, which separates the ethmoid sinus from the orbit, is also thin in children, allowing easy spread of infection from sinusitis to the periorbital area.
When inflammation extends beyond the orbital septum into the orbit, it progresses to orbital cellulitis (Group 2 or higher). In cases with sinusitis, rapid progression from the ethmoid sinus to subperiosteal abscess (Group 3) via the medial orbital wall may occur. 2)
The progression pathway is stepwise as follows:
Transition between stages can occur within hours to days, so reassessment within 24 to 48 hours is essential.
For the decision between outpatient and inpatient management of pediatric preseptal cellulitis, stratification based on age, inflammatory response, and symptom severity is being explored. Establishing quantitative criteria for safe management with oral antibiotics alone is expected to reduce unnecessary hospitalizations while ensuring safety.
In empirical treatment of preseptal cellulitis, antibiotic selection based on regional MRSA prevalence and drug susceptibility is important. Since hospital-acquired MRSA and community-acquired MRSA differ in pathology and susceptibility, empirical treatment selection based on local drug susceptibility surveillance is required.
Research is underway to establish quantitative differential diagnostic criteria (e.g., thickness and extent of soft tissue swelling) for preseptal cellulitis and orbital cellulitis using CT findings. Setting objective thresholds for imaging diagnosis is expected to improve the accuracy of appropriate triage and treatment stratification.