IgG4-Related Ophthalmic Disease (Mikulicz Disease, etc.)
1. What is IgG4-related ophthalmic disease?
Section titled “1. What is IgG4-related ophthalmic disease?”IgG4-related ophthalmic disease (IgG4-ROD) is a disease of unknown cause characterized by elevated serum IgG4 and infiltration of IgG4-positive plasma cells into the orbit, leading to mass formation and tissue thickening. It is considered the orbital localized form of systemic IgG4-related disease (IgG4-RD).
IgG4-RD is a disease in which plasma cells producing IgG4, one of the immunoglobulins in the serum, infiltrate various organs throughout the body, causing mass formation and tissue thickening. The concept was established in 2001 as the etiology of autoimmune pancreatitis. In the ophthalmology field, IgG4-related Mikulicz disease was first reported in 2004, and the concept of IgG4-related disease subsequently spread to ophthalmology. Diagnostic criteria were first established in 2014 1) and revised in 2023 1).
In Japan, the most common primary orbital tumors are lymphoproliferative diseases, which include malignant lymphoma, reactive lymphoid hyperplasia, IgG4-ROD, and idiopathic orbital inflammation (IOI). Lymphoproliferative diseases alone account for 50-60% of all orbital tumors. It has been found that 17-60% of cases diagnosed as idiopathic orbital inflammation are actually IgG4-ROD. Many cases of what was previously called Mikulicz disease and specific orbital inflammation have been reclassified under this disease.
IgG4-ROD shows no gender difference, with an average age of approximately 55-60 years. Cases under 20 years of age are rare.
Sites of involvement in IgG4-ROD
Section titled “Sites of involvement in IgG4-ROD”In a multicenter study of 378 cases, the distribution of involved sites was as follows 1):
| Site of involvement | Frequency |
|---|---|
| Lacrimal gland | 62-88% (86% in the 378-case study) |
| Orbital fat | 28.6-40% |
| Extraocular muscles | 19-25% (21% in the 378-case study) |
| Peritrigeminal nerve | 9.5–39% (20% in a study of 378 cases) |
| Eyelid | 12% |
| Nasolacrimal duct system | 1.5–9.5% |
In the same study, subjective symptoms included dry eye 22%, diplopia 20%, decreased visual acuity 8%, and visual field defects 5%1).
Serum IgG4 is considered normal below 135 mg/dL, and the condition is characterized by three major lesions: lacrimal gland swelling, peritrigeminal nerve mass, and extraocular muscle swelling. Other orbital lesions include orbital fat swelling, masses around the optic nerve and blood vessels, and lesions of the eyelid skin, conjunctiva, lacrimal sac, and sclera.
2. Main Symptoms and Clinical Findings
Section titled “2. Main Symptoms and Clinical Findings”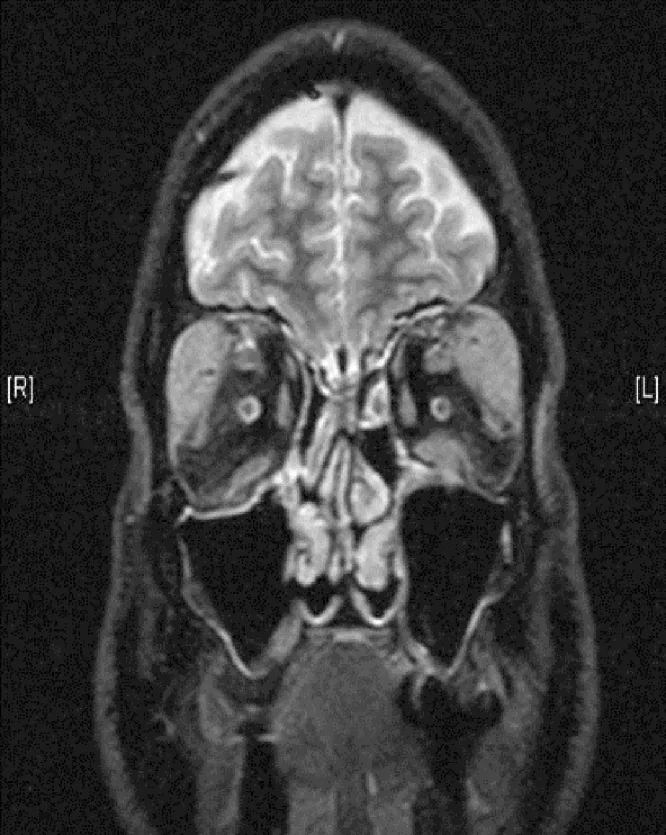
Subjective Symptoms
Section titled “Subjective Symptoms”- Eyelid swelling: due to lacrimal gland enlargement. Typically painless and slowly progressive. Often bilateral, and when accompanied by salivary gland swelling, it is classified as Mikulicz disease.
- Proptosis: due to swelling of extraocular muscles and orbital soft tissues.
- Diplopia: may cause restrictive strabismus due to extraocular muscle involvement. The inferior rectus is most frequently affected.
- Decreased visual acuity and visual field defects: Due to compressive optic neuropathy. In a study of 378 cases, decreased visual acuity was observed in 8% and visual field defects in 5%1).
- Dry eye: Observed in 22% of 378 cases. However, because lacrimal gland destruction is limited, it is often less severe than in Sjögren’s syndrome.
Clinical Findings (Findings Confirmed by Physician Examination)
Section titled “Clinical Findings (Findings Confirmed by Physician Examination)”- Lacrimal gland enlargement: Eyelid swelling with S-shaped deformity. On MRI, bilateral lacrimal gland enlargement is the most common finding.
- Trigeminal nerve enlargement: Masses around the supraorbital and infraorbital nerves. This is a characteristic finding of IgG4-ROD and helps differentiate it from thyroid eye disease.
- Extraocular muscle enlargement: Differentiation from thyroid eye disease is necessary.
- Perioptic nerve lesions: Can lead to optic neuropathy. Particular caution is needed in cases with high IgG4 levels exceeding 500 mg/dL.
- MRI findings: Isointense on T1-weighted images, hypointense on T2-weighted images, and homogeneously enhanced with gadolinium.
Systemic lesions are found in 68% of patients with IgG4-ROD. The most common sites of involvement are the salivary glands (43%), lymph nodes (27%), and pancreas (20%).
Both conditions can present with extraocular muscle enlargement and proptosis. Differentiation relies on serum IgG4 levels, thyroid function tests (T3, T4, TSH), MRI findings (IgG4-ROD shows T2 hypointensity and is more likely to involve trigeminal nerve hypertrophy), and tissue biopsy. IgG4-ROD is more often associated with lacrimal gland enlargement, while thyroid eye disease predominantly involves enlargement of the inferior and medial rectus muscles.
3. Causes and Risk Factors
Section titled “3. Causes and Risk Factors”The etiology of IgG4-ROD is unknown, but abnormalities in humoral and cellular immunity are thought to be involved.
- B-cell abnormalities: The efficacy of rituximab (anti-CD20) strongly suggests the involvement of B cells.
- Th2 cytokines: Increased production of IL-4, IL-5, and IL-13 has been reported, accompanied by eosinophilia and elevated IgE.
- Antigenic stimulation: Somatic hypermutation in the lacrimal gland suggests a local immune response.
Reported risk factors include older men (systemic type), atopic predisposition, asthma, and allergic rhinitis. Patients with IgG4-ROD may have an increased risk of non-Hodgkin lymphoma; the 2023 revised criteria Attention II also warns about follicular lymphoma and diffuse large B-cell lymphoma (DLBCL) other than MALT 1).
4. Diagnosis and Examination Methods
Section titled “4. Diagnosis and Examination Methods”2023 Revised Diagnostic Criteria for IgG4-ROD 1)
Section titled “2023 Revised Diagnostic Criteria for IgG4-ROD 1)”Judgment is made based on the following three items.
| Item | Content |
|---|---|
| ① Imaging findings | Lacrimal gland enlargement, trigeminal nerve enlargement, extraocular muscle enlargement, as well as mass, enlargement, or thickening lesions in various ocular tissues |
| ② Histopathological findings | Marked lymphoplasmacytic infiltration. IgG4-positive/IgG-positive cell ratio ≥40%, or IgG4-positive cell count ≥50/HPF (×400). Germinal centers are often observed. |
| ③ Serum IgG4 | >135 mg/dL |
- Definite: Meets all 3 items ①, ②, ③
- Probable: Meets 2 items ①, ②
- Suspected: Meets 2 items ①, ③
Attention added in the 2023 revision1):
- Attention I: Be aware of vision loss and visual field defects due to optic neuropathy. Hypertrophic pachymeningitis can also cause optic neuropathy.
- Attention II: Not only MALT lymphoma but also follicular lymphoma and diffuse large B-cell lymphoma (DLBCL) can arise in the context of IgG4-ROD.
Imaging
Section titled “Imaging”- MRI: Isointense on T1-weighted images, hypointense on T2-weighted images, and homogeneously enhanced with gadolinium.
- FDG-PET/CT: Useful for detecting distant and asymptomatic lesions.
Clinical Laboratory Testing Considerations
Section titled “Clinical Laboratory Testing Considerations”Serum IgG4 level is a marker of treatment response. However, it should be noted that 40% of patients with definite IgG4-RD have normal serum IgG4 levels. Additionally, elevated IgG4 levels can also be seen in pancreatic cancer, lymphoma, and ANCA-associated vasculitis, so specificity is limited.
Essential tests include serum IgG4 measurement, imaging (contrast-enhanced MRI/CT), and biopsy with histopathological examination (including immunohistochemistry).
Differential Diagnosis
Section titled “Differential Diagnosis”Differentiation from MALT lymphoma is particularly important. MALT lymphoma is usually negative for IgG4 staining, but some cases may be positive. Examining IgH gene rearrangement in biopsy specimens is useful for differentiation.
| Differential Diagnosis | Key Points for Differentiation |
|---|---|
| MALT lymphoma | IgH gene rearrangement test. May also be IgG4 staining positive, caution required. |
| Follicular lymphoma / DLBCL | Alerted in the 2023 revised criteria Attention II 1) |
| Sjögren’s syndrome | Anti-Ro/La antibodies. Lacrimal and salivary gland atrophy predominant. |
| Sarcoidosis | ACE level, chest imaging, non-caseating epithelioid granulomas. |
| Granulomatosis with polyangiitis | ANCA serology. |
| Thyroid eye disease | Thyroid function tests (T3, T4, TSH). No trigeminal nerve hypertrophy. |
| Idiopathic orbital inflammation (IOI) | Reclassified by IgG4 staining. 17–60% of IOI are IgG4-ROD. |
| Bacterial or fungal infection | Acute onset, pain, fever. |
5. Standard Treatment
Section titled “5. Standard Treatment”Before treatment, a tissue diagnosis is essential to rule out malignancy. Treatment may not always be necessary if only ocular lesions are present or if there are no organ lesions other than the salivary glands. However, in addition to cosmetic improvement, treatment is absolutely indicated when visual impairment such as decreased visual acuity or visual field narrowing occurs.
Oral Steroid Tapering Therapy (First-line)
Section titled “Oral Steroid Tapering Therapy (First-line)”Start with prednisolone 30 mg/day (0.6 mg/kg/day) and taper by 10% every 2 weeks. Continue a maintenance dose of 10 mg/day for at least 3 months.
Initial response is excellent at 89–100%, but the relapse rate during and after treatment reaches up to 70%. Continuation of a maintenance dose of 5 mg/day has been reported to reduce the 3-year relapse rate from 92% to 23%.
Steroid Pulse Therapy (for Optic Neuropathy)
Section titled “Steroid Pulse Therapy (for Optic Neuropathy)”Indicated when visual acuity loss or visual field defects due to optic neuropathy are severe. One course consists of Solu-Cortef 500 mg IV once daily for 3 days, and 1–3 courses are administered. In a review of 44 cases of optic neuropathy, vision improved in many cases with steroids, rituximab, or decompression surgery, but recovery was poor in severe cases with no light perception 1).
Rituximab (Not Covered by Insurance in Japan)
Section titled “Rituximab (Not Covered by Insurance in Japan)”Rituximab (anti-CD20 antibody) is the most effective disease-modifying drug, with a response rate of 93% and a relapse rate of 9%. Two 1 g IV infusions given 14 days apart are recommended. It is not covered by insurance in Japan; consider administration based on overseas experience.
Other Immunosuppressive Drugs
Section titled “Other Immunosuppressive Drugs”For steroid-resistant or relapsed cases, immunosuppressive drugs such as methotrexate, azathioprine, and mycophenolate mofetil are used, but evidence is limited.
If the lesion is confined to the lacrimal gland or systemic administration is undesirable, lacrimal gland excision or local steroid injection may be options.
Relapse is common during tapering (when reducing prednisolone to less than 10 mg/day) or after steroid discontinuation. Management of relapse includes re-administration of oral steroids (for 6–10 weeks) or addition of disease-modifying drugs such as rituximab. Rituximab has the lowest relapse rate at 9%. Long-term continuation of a maintenance dose of 5 mg/day can reduce the 3-year relapse rate from 92% to 23%, so a long-term management plan is important.
6. Pathophysiology and Detailed Pathogenesis
Section titled “6. Pathophysiology and Detailed Pathogenesis”The three main pathological features of IgG4-RD are as follows:
- Dense lymphoplasmacytic infiltration
- Storiform fibrosis
- Obliterative phlebitis
If two of these (most commonly a combination of 1 and 2) are present, a diagnosis of IgG4-RD is made. In IgG4-ROD, T lymphocytes are observed, and storiform fibrosis may be absent in lacrimal gland lesions.
On immunohistochemistry, the criteria are an IgG4-positive plasma cell / IgG-positive cell ratio of ≥40%, or ≥50 IgG4-positive cells/HPF (×400). For lacrimal gland disease, a stricter criterion requiring ≥100 IgG4-positive cells/HPF is adopted1).
B-cell abnormalities are central to the pathogenesis, and the efficacy of rituximab supports this involvement. Overproduction of Th2 cytokines (IL-4, IL-5, IL-13) leads to elevated IgG4 and IgE levels and eosinophilia. Evidence of somatic hypermutation in the lacrimal gland suggests a local antigen-driven response.
IgG4-related Mikulicz disease is characterized by symmetric enlargement of the lacrimal and salivary glands. Because destruction of lacrimal gland tissue is limited, dry eye symptoms are often not as prominent as in Sjögren’s syndrome. Response to steroid therapy is generally good, but relapse during tapering is a problem. In cases complicated by severe optic neuropathy, blindness may occur, and visual prognosis can be worse than that of orbital low-grade lymphoma.
7. Latest Research and Future Perspectives
Section titled “7. Latest Research and Future Perspectives”Development of the 2023 revised diagnostic criteria and its background1)
Section titled “Development of the 2023 revised diagnostic criteria and its background1)”Takahira et al. (2024) 1) published revised diagnostic criteria based on a multicenter study by the Ministry of Health, Labour and Welfare research group for intractable diseases, adding Attention I (alert for optic neuropathy) and Attention II (alert for lymphoma other than MALT) to the 2014 diagnostic criteria. The revision is based on a multicenter study of 378 cases (lacrimal gland 86%, extraocular muscles 21%, trigeminal nerve 20%) and a review of 44 cases of optic neuropathy (age 17–86 years, median 61, male-to-female ratio 30:14, median serum IgG4 355 mg/dL). In the review of 44 optic neuropathy cases, many patients recovered vision with steroids, rituximab, or decompression surgery, but severe cases with no light perception had poor recovery.
IgG4-ROD after SARS-CoV-2 vaccination 2)
Section titled “IgG4-ROD after SARS-CoV-2 vaccination 2)”Zhang et al. (2024) reported one case of IgG4-ROD after SARS-CoV-2 vaccination and reviewed the literature, identifying a small number of post-infection and post-vaccination cases. Among them, 5 cases occurred after vaccination and 4 after infection. However, a causal relationship has not been established, and the involvement of immune dysregulation remains hypothetical 2).
Association with SAPHO syndrome 3)
Section titled “Association with SAPHO syndrome 3)”Liu et al. (2025) reported a single case of IgG4-ROD associated with SAPHO syndrome. The involvement of the TNF-α pathway remains hypothetical and has not been established as a therapeutic target for both diseases. Although the coexistence of both diseases is rare, it may follow a refractory course 3).
Orbital decompression via transcranial approach 4)
Section titled “Orbital decompression via transcranial approach 4)”Noda et al. (2021) performed a transcranial biopsy via the pterygoid process and lateral orbital wall decompression in a 63-year-old man with a serum IgG4 level of 1,255 mg/dL. Visual acuity improved from 0.7 LogMAR to −0.1 LogMAR three days after surgery, and intraocular pressure normalized from 31 mmHg to 15 mmHg. This surgical option is noteworthy for cases with high risk of steroid therapy or requiring rapid visual improvement. 4)
8. References
Section titled “8. References”- Takahira M, Goto H, Azumi A. The 2023 revised diagnostic criteria for IgG4-related ophthalmic disease. Jpn J Ophthalmol. 2024;68:293-301.
- Zhang P, Wu Q, Xu X, et al. A case of IgG4-related ophthalmic disease after SARS-CoV-2 vaccination: case report and literature review. Front Immunol. 2024;15:1303589.
- Liu C, Chen T, Wang Y, et al. SAPHO syndrome complicated by IgG4-related ophthalmic disease: a case report and literature review. Front Immunol. 2025;16:1563542.
- Noda R, Inoue T, Tsunoda S, et al. Surgical management for IgG4-related ophthalmic disease by a transcranial biopsy combined with extraorbital decompression: illustrative case. J Neurosurg Case Lessons. 2021;1(8):CASE20170.
