Induction Therapy
Steroid pulse: Methylprednisolone 1 g/day for 3–5 days.
Oral steroids: Transition to prednisolone 1 mg/kg/day, then taper.
Cyclophosphamide: 500 mg/month for 6 months (NIH protocol). Combination with steroids is standard.

Primary angiitis of the central nervous system (PACNS) is a vasculitis in which inflammation occurs exclusively in the arteries and veins of the brain, spinal cord, and meninges, and is clearly distinguished from secondary CNS vasculitis (associated with systemic diseases).
Harbitz first reported it in 1922, and Calabrese proposed diagnostic criteria in 1988 5).
Epidemiologically, the annual incidence is about 2.4 cases per million, making it a rare disease 1, 2). The median age at diagnosis is approximately 50 years, but it can occur at any age, including in children. Regarding sex, a male predominance of 2:1 was previously reported, but some recent case series suggest no sex difference.
Vasculitis syndromes are a group of conditions classified by the size of the affected blood vessels, and PACNS is positioned as a subtype limited to CNS vessels.
The cause is unknown; involvement of inflammatory reactions triggered by infectious agents such as VZV and Mycoplasma has been proposed, but there is no definitive evidence.
PACNS is vasculitis limited to the CNS and is characterized by the absence of systemic disease. Secondary CNS vasculitis occurs in association with systemic diseases such as SLE, Sjögren’s syndrome, infections, and malignancies, and is much more common. If fever or markedly elevated ESR is present, secondary vasculitis should be strongly suspected.
Symptoms of PACNS are often nonspecific, which can lead to delayed diagnosis.
In children, hemiparesis (up to 80%), sensory loss (79%), and fine motor impairment (73%) are frequent, while headache and cognitive impairment are less common than in adults (56% and 37%).
Zhuo et al. (2022) reported a 5-year-old girl with tumor-like PACNS who presented with left homonymous hemianopia and imaging showed tumor-like lesions in the left occipital and temporal lobes2).
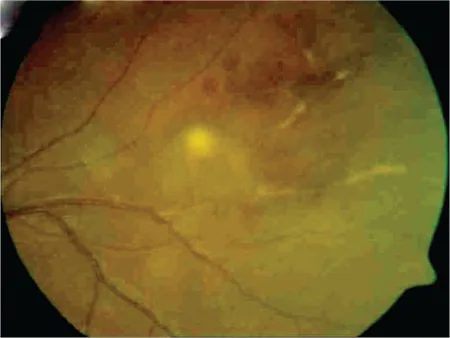
When the visual pathway (optic nerve, optic chiasm, occipital lobe) or oculomotor nerves are affected, decreased vision, visual field defects, and diplopia may occur. Uveitis and retinal vasculitis are not typical in PACNS; if present, secondary diseases such as systemic vasculitis must be ruled out.
The exact etiology of PACNS remains unknown, and no specific risk factors have been proven.
The following are causes of secondary CNS vasculitis, which must be excluded when diagnosing PACNS.
| Cause Category | Representative Diseases/Factors |
|---|---|
| Infections | VZV, HIV, HCV, CMV, syphilis, tuberculosis, aspergillosis |
| Connective Tissue Diseases | SLE, RA, Sjögren’s syndrome, dermatomyositis |
| Other systemic diseases | Antiphospholipid antibody syndrome, malignant lymphoma, neurosarcoidosis |
| Drugs | Cocaine, amphetamine, ephedrine |
PACNS is a diagnosis of exclusion, and there is no single definitive biomarker.
The criteria by Calabrese & Mallek (1988) are widely used1).
The Rice & Scolding classification further divides cases into “definite” (with histological evidence) and “probable” (based on clinical, imaging, and CSF findings) 5).
The most important differential diagnosis is RCVS (reversible cerebral vasoconstriction syndrome). RCVS is more common in younger individuals, presents with severe recurrent thunderclap headaches, and CSF is often normal. Unlike PACNS, immunosuppressive therapy is contraindicated for RCVS.
Giant cell arteritis typically presents with headache in individuals over 60 years of age and is confirmed by arterial biopsy. Since 25–50% of cases are complicated by anterior ischemic optic neuropathy, ophthalmologic findings are important.
The gold standard is histological confirmation via brain biopsy, but its sensitivity is only about 75% 3). A combination of MRI, cerebral angiography, and cerebrospinal fluid analysis is used to comprehensively diagnose after excluding secondary causes. It is recommended to perform multiple tests in parallel to complement sensitivity.
Treatment for PACNS primarily involves immunosuppressive therapy. Management should be carried out in collaboration with neurologists and rheumatologists.
Induction Therapy
Steroid pulse: Methylprednisolone 1 g/day for 3–5 days.
Oral steroids: Transition to prednisolone 1 mg/kg/day, then taper.
Cyclophosphamide: 500 mg/month for 6 months (NIH protocol). Combination with steroids is standard.
Maintenance Therapy
Start timing: Switch after 4–6 months of induction therapy.
Drug selection: Use either mycophenolate mofetil (MMF), methotrexate, or azathioprine.
Example MMF dose: Start at 500 mg twice daily, then increase to 1000 mg twice daily4).
Switch after 4–6 months of induction therapy. MMF, methotrexate, or azathioprine is used6).
In a 35-year-old male case by Kuruvilaa et al. (2022), treatment was started with steroids plus MMF (500 mg twice daily → 1000 mg twice daily) and a good outcome was obtained4).
In an 8-year-old child with SV-cPACNS (GFAP antibody positive) reported by Datyner et al. (2023), treatment followed the Brainworks protocol: dexamethasone → methylprednisolone pulse for 5 days → taper over 12 months + CYC 7 times → MMF maintenance 8).
Induction therapy (steroids + CYC) is given for about 6 months, then transitioned to maintenance therapy such as MMF. Long-term follow-up is needed due to risk of relapse, and treatment duration varies by case. Taper while monitoring treatment response with regular imaging and clinical evaluation.
PACNS has three main histopathological subtypes.
Granulomatous
Frequency: Most common subtype.
Pathological findings: Well-defined granulomas involving the full thickness of the vessel wall.
Association with beta-amyloid: Up to 50% of cases have beta-amyloid deposition, suggesting overlap with inflammatory cerebral amyloid angiopathy.
Lymphocytic
Pathological findings: Infiltration of the vessel wall by lymphocytes and plasma cells.
Characteristics in children: Lymphocytic pattern is common in pediatric PACNS5).
Necrotizing
Pathological findings: Fibrinoid necrosis of the vessel wall.
Rare subtype: Cases with eosinophilic infiltration have also been reported, showing pathological findings of EGPA but not meeting the diagnostic criteria for systemic EGPA7).
Inflammation of the vascular wall is primarily driven by immune cell infiltration and the cytokine/chemokine network 5).
While PACNS is typically bilateral (95.6% of the Mayo Clinic cohort F was bilateral), a rare subtype with recurrent episodes limited to one side has been reported. Immune response asymmetry between cerebral hemispheres is considered a cause, and 7 cases have been reported to date10).
Vibha et al. (2023) reported a case of PACNS in a 35-year-old man who presented only with recurrent focal aware seizures 10). He initially had focal seizures only, and biopsy confirmed granulomatous vasculitis; seizures resolved with steroids plus MMF.
Vessel wall MRI is a promising technique for differentiating PACNS from RCVS. PACNS often shows vessel wall enhancement (inflammatory changes), whereas RCVS typically does not. Brain MRA sensitivity is reported to be 90–100% 1).
Tumor-like PACNS accounts for about 5% of all PACNS cases and is difficult to differentiate from tumors on imaging 2). A combination of SWI (susceptibility-weighted imaging) and ASL (arterial spin labeling) has been reported useful for differentiation. PACNS tends to show hypoperfusion, while tumors show hyperperfusion.
Hydrocephalus has been reported in 1.8% of CNS vasculitis cases and is a major cause of in-hospital mortality 3). It is extremely rare in PACNS, with only 2 reported cases. The mechanism is presumed to be CSF flow obstruction due to fibrous scarring of the meninges.
Levit et al. (2023) reported a case of complement-mediated CNS vasculitis due to complement factor I (CFI) deficiency 9). CFI inactivates C3b and C4b, suppressing C3 convertase formation; its deficiency leads to abnormal activation of the alternative pathway and neutrophilic vasculitis. After treatment with the IL-1 inhibitor anakinra, no recurrence was observed for 20 months.