Direct Infection
Direct neural infection via the cavernous sinus: Optic neuropathy caused by VZV directly invading the optic nerve from the trigeminal ganglion via the cavernous sinus.

Herpes Zoster Optic Neuritis (HZON) is a rare sequela of herpes zoster ophthalmicus (HZO) that results in optic neuritis. It occurs in association with herpes zoster in the first division (ophthalmic nerve) of the trigeminal nerve.
HZO occurs in about 10–20% of all herpes zoster cases, and about half of these develop some ocular complication. HZON is a rare complication among these ocular complications, and optic neuritis has been reported in about 1.9% of eyes with HZO 1.
Hutchinson sign refers to the presence of a rash on the tip and side of the nose, corresponding to the innervation area of the nasociliary nerve. When Hutchinson sign is positive, the frequency of ocular complications is significantly higher.
Zoster sine herpete (ZSH) may present with neurological symptoms alone without a rash. In such cases, diagnosis can be difficult, and caution is needed.
If severe HZO is observed in a young patient, consider the possibility of HIV infection. In immunocompromised states with CD4-positive lymphocyte counts ≤500/μL, herpes zoster tends to be more severe.
Onset has been reported simultaneously with HZO or up to 10 weeks after HZO onset. Cases of optic neuritis developing about 1 month after rash onset 2 and about 45 days after onset 3 have been reported, so visual loss may occur some time after the HZO rash appears. Continuous attention to visual changes in HZO patients is necessary.
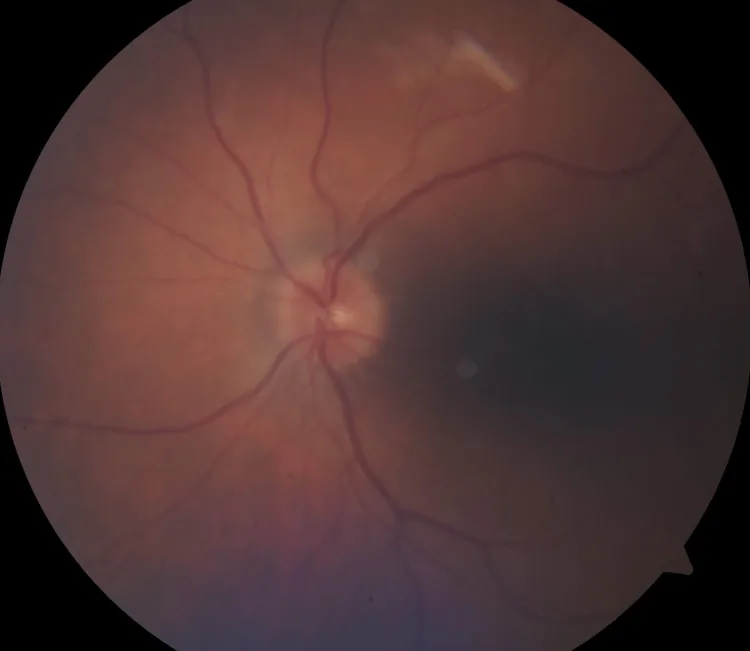
Systemic symptoms of HZO itself include fever, malaise, headache in the first division of the trigeminal nerve area, and eye pain. Before the rash appears, patients may complain of discomfort or pain in the area innervated by the trigeminal nerve.
As a symptom of optic neuritis, the main complaint is decreased visual acuity in the affected eye.
The cause of HZON is reactivation of varicella-zoster virus (VZV) that has latently infected the ganglia.
Unlike HSV, VZV is inactivated as soon as it leaves the cell. Upon reactivation, it appears directly on the skin via nerves, so the rash is strictly limited to the innervated area.
The following factors increase the risk of HZON.
Clinical diagnosis of HZON is made when acute unilateral or bilateral anterior or retrobulbar optic neuropathy occurs during the course of HZO or within approximately 3 months of onset.
The main examination methods are shown below.
| Examination | Findings/Purpose |
|---|---|
| Orbital MRI | Contrast enhancement and diffusion restriction of the affected optic nerve, linear hyperintensity of the trigeminal nucleus on T2-weighted images |
| Fluorescein angiography (FA) | Late staining of the affected optic disc |
| Lumbar puncture and cerebrospinal fluid analysis | Detection of VZV by PCR and serological tests (some PCR-negative cases reported) |
MRI is the first-choice examination for optic nerve diseases. Coronal STIR and contrast-enhanced T1-weighted images are useful. Restricted diffusion of the optic nerve has been proposed as a predictor of poor visual recovery 1. Linear hyperintensity in the trigeminal nucleus and tract on T2-weighted images of the brainstem may suggest VZV-related complications 1. Severe cases with contrast enhancement along the entire length of the intraorbital optic nerve and complicated ischemic optic neuropathy have also been reported 4.
Doppler ultrasound usually shows normal blood flow, which helps differentiate from vascular optic neuropathy.
Blood tests necessary for differential diagnosis include CBC, ESR, CRP, syphilis serology, ANA, AQP4 antibody, and MOG antibody.
Differentiation from the following diseases is important.
Exclusion of giant cell arteritis is urgent; ESR, CRP, and temporal artery biopsy may be necessary.
The basis of treatment is systemic administration of antiviral drugs.
They are used as follows depending on the severity of the case.
In standard Japanese treatment, systemic administration of antiviral drugs is also the mainstay, and severe cases are hospitalized for intravenous administration. For HZO skin lesions, acyclovir ophthalmic ointment is used concomitantly. In mild cases in immunocompetent patients, there are reports of good visual recovery with oral valacyclovir therapy 5.
Mechanism of action of acyclovir: It is phosphorylated by thymidine kinase (TK) produced by VZV, and the triphosphate form selectively inhibits viral DNA polymerase. Since it is not phosphorylated in normal host cells, it has high selective toxicity.
The advisability of concomitant steroid use is debated.
For HZO pseudodendritic keratitis, unlike HSV keratitis, steroid eye drops can be used.
In infectious optic neuritis, steroid pulse therapy (methylprednisolone 1,000 mg IV for 3 days) should not be used alone; causal treatment with antiviral drugs should be prioritized.
It is not uniformly recommended. When intraocular inflammation is prominent, concomitant use may be considered, but it may increase the risk of VZV retinitis, so careful assessment of indications is necessary. The principle is to consider use after adequate antiviral therapy. Some systematic reviews suggest that early combination therapy with antivirals and steroids may improve visual prognosis 6.
The following three pathophysiological mechanisms have been proposed for the development of HZON.
Direct Infection
Direct neural infection via the cavernous sinus: Optic neuropathy caused by VZV directly invading the optic nerve from the trigeminal ganglion via the cavernous sinus.
Inflammatory Demyelination
Inflammatory demyelination: A mechanism in which local inflammation associated with VZV infection damages the myelin sheath of the optic nerve. It shares some features with the pathology of optic neuritis.
Immune Response
Optic disc edema due to reactive immune response: A mechanism in which the host immune response to systemic or CNS infection causes edema of the optic disc.
After primary infection (chickenpox), VZV establishes lifelong latent infection in sensory ganglia, including the trigeminal ganglion. When reactivation occurs due to aging or immunosuppression, the virus travels retrogradely along nerve axons to reach the skin and ocular tissues, causing herpes zoster.
Postherpetic neuralgia (PHN) that appears after HZO is a problem as severe pain lasting months to years.
Three mechanisms are currently proposed: direct infection of the optic nerve via the cavernous sinus, demyelination of the optic nerve due to inflammation, and optic disc edema caused by a reactive immune response to systemic or CNS infection 6. It is thought that multiple mechanisms, rather than a single one, combine to cause optic nerve damage.
Vanikieti K, Poonyathalang A, Jindahra P, Cheecharoen P, Patputtipong P, Padungkiatsagul T. Isolated optic neuritis with a concurrent abnormal trigeminal nucleus on imaging: case report of a rare complication of herpes zoster ophthalmicus. BMC Neurol. 2018 Oct 4;18(1):165. doi: 10.1186/s12883-018-1168-3. PMID: 30286736; PMCID: PMC6171195. ↩ ↩2 ↩3
Mohd Zaidan KN, Mohammad Razali A, Md Noh MSF, Md Saleh R, Mohd Isa M. Herpes Zoster Optic Neuritis: A Catastrophe of a Disease. Cureus. 2024 May 15;16(5):e60387. doi: 10.7759/cureus.60387. PMID: 38883008; PMCID: PMC11178973. ↩
Vitor BM, Foureaux ECM, Porto FBO. Herpes zoster optic neuritis. Int Ophthalmol. 2011 Jun;31(3):233-236. doi: 10.1007/s10792-011-9443-y. PMID: 21626168. ↩
Kudo T, Yamauchi K, Suzuki Y, Nakazawa M, Ueno S. A case of herpes zoster ophthalmicus with optic neuritis of the total length of the optic nerve in the orbital space and ischemic optic neuropathy. Am J Ophthalmol Case Rep. 2022 Nov 23;28:101756. doi: 10.1016/j.ajoc.2022.101756. PMID: 36467120; PMCID: PMC9713266. ↩
Hunt CM, Gregory HM, Gannon W. Oral Valacyclovir Treatment of Herpes Zoster Ophthalmicus-Induced Optic Neuritis. Cureus. 2021 Aug 9;13(8):e17033. doi: 10.7759/cureus.17033. PMID: 34522513; PMCID: PMC8425502. ↩
Pourmahdi-Boroujeni M, Abtahi-Naeini B, Rastegarnasab F, Afshar K, Akhlaghi M, Pourazizi M. Optic Neuritis Associated with Herpes Zoster Ophthalmicus: A Systematic Review and Analysis. Ocul Immunol Inflamm. 2025 Oct;33(8):1732-1747. doi: 10.1080/09273948.2025.2530144. PMID: 40700721. ↩ ↩2