Idiopathic (54.6%)
Idiopathic: The most common type with unknown cause4)6). Benign and tends to resolve spontaneously.
Congenital: Accounts for about 6% of cases. In neonates, hypothalamic immaturity is involved2)6).

Harlequin syndrome is an autonomic nervous system syndrome caused by unilateral dysfunction of the sympathetic nervous system. It is characterized by anhidrosis and vasoconstriction (pallor) on the affected side of the face and upper body, and compensatory sweating and flushing on the opposite side.
It was first reported by Lance and Drummond in 1988 1). The name is derived from the red-and-black divided mask of “Harlequin,” a character from 16th-century Italian commedia dell’arte 6). Note that this is completely different from harlequin ichthyosis (a severe genetic skin disorder) 6).
The “Harlequin sign” refers to the physical finding of asymmetric facial flushing and sweating, while “Harlequin syndrome” is a concept used in a broader clinical context, including idiopathic and congenital cases 6).
Approximately 100 cases have been reported in the literature 1)4). According to a review of 108 cases by Guilloton et al., idiopathic cases account for 54.6%, and secondary/iatrogenic cases account for 45.4% 4)6). Congenital cases are estimated to be about 6% of all cases 6). It is most common in women and in the third decade of life 1), with only 37 pediatric cases reported 1). In newborns, it is relatively frequently observed due to functional immaturity of the hypothalamus 2).
It is a completely different disease. Harlequin syndrome is an autonomic nervous system disorder caused by sympathetic nervous system dysfunction, while harlequin ichthyosis is a severe hereditary skin disease. Although the disease names are similar, the pathophysiology, symptoms, and treatment are entirely different6).
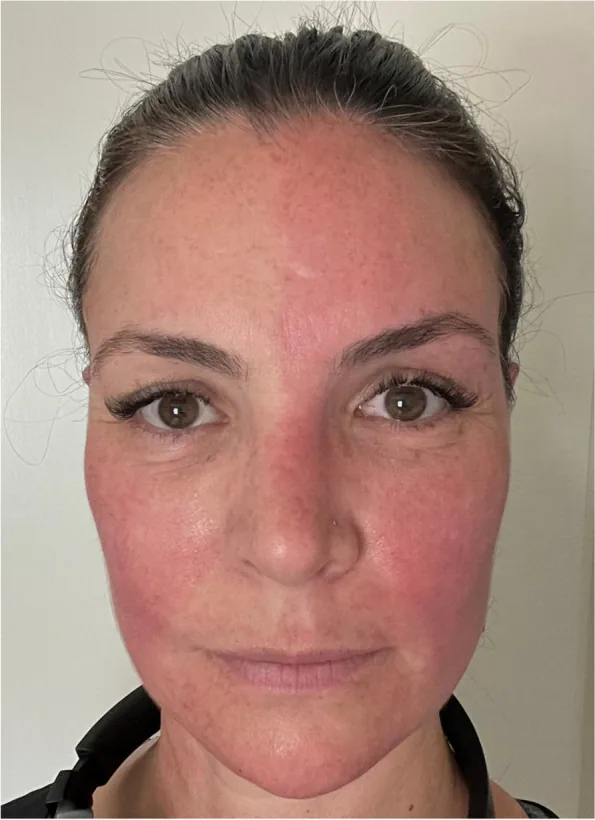
Symptoms appear intermittently and may occur at rest without any trigger.
The pathogenesis involves interruption of sympathetic innervation at the preganglionic or postganglionic level. Sympathetic function is lost on the affected side, while the contralateral side becomes compensatorily overactive, leading to asymmetric findings. Associations with migraine and trigeminal autonomic cephalalgias have also been reported1)3).
Idiopathic (54.6%)
Idiopathic: The most common type with unknown cause4)6). Benign and tends to resolve spontaneously.
Congenital: Accounts for about 6% of cases. In neonates, hypothalamic immaturity is involved2)6).
Secondary (45.4%)
Compressive lesions: Pancoast tumor, mediastinal tumor, thyroid goiter (reported with a 62×52×32 mm multinodular goiter), carotid artery dissection1)3)6)
Iatrogenic: After sympathectomy, after anesthetic procedures (e.g., ESP block), after catheter placement1)5)
Systemic diseases: Guillain-Barré syndrome, diabetic neuropathy, multiple sclerosis, brainstem infarction, syringomyelia1)2)3)
Diffusion of anesthetic into the paravertebral space can temporarily block the sympathetic nerve, causing harlequin-like findings. There is also a report of delayed onset (5 hours later) after a T2-level paravertebral block using liposomal bupivacaine5). This iatrogenic case usually resolves spontaneously within 6 to 12 hours5).
Diagnosis is primarily a clinical diagnosis based on characteristic clinical findings6).
Imaging tests are important to rule out secondary causes.
Differentiation from the following diseases is necessary.
| Disease | Key differentiating points |
|---|---|
| Ross syndrome | Triad of widespread anhidrosis, loss of deep tendon reflexes, and Adie’s pupil |
| Horner syndrome | Only miosis, ptosis, and anhidrosis. No compensatory contralateral flushing. |
| Holmes-Adie syndrome | Pupillary abnormality and loss of deep tendon reflexes are predominant |
Treatment strategy varies depending on the cause.
For secondary cases, treatment of the underlying disease is the highest priority6). Idiopathic cases are benign and self-limiting, and most are managed with counseling and observation alone2)3).
Pharmacotherapy
Propranolol: A beta-blocker. Used to suppress sweating and flushing3).
Oxybutynin: Anticholinergic drug. Expected to be effective for hyperhidrosis3).
Procedures and Surgical Treatments
Botulinum toxin injection: Local administration to compensatory hyperhidrosis sites1).
Stellate ganglion block: Symptom relief via sympathetic nerve blockade1)3).
VATS sympathectomy: A 43-year-old female patient reported complete symptom resolution immediately after surgery, with no recurrence at 4 months4).
Idiopathic cases are benign and tend to resolve spontaneously, so treatment is not always necessary2)3). Only when social or psychological distress is significant, consider botulinum toxin injection, stellate ganglion block, or sympathectomy. In secondary cases, treatment of the underlying disease takes priority.
Harlequin syndrome is based on a disruption of the three-neuron pathway of sympathetic innervation to the face and trunk3).
Whether Horner syndrome is present depends on the level of the sympathetic pathway affected by the lesion3)6).
| Lesion site | Horner syndrome present | Clinical features |
|---|---|---|
| T1–T3 (oculosympathetic + sudomotor/vasomotor) lesion | Yes | Harlequin syndrome + Horner syndrome |
| T2 to T3 only impairment | None | Harlequin syndrome alone |
| Postganglionic lesion after superior cervical ganglion | Present (medial forehead anhidrosis) | Other facial areas may be spared |
When the sympathetic nerve on the affected side is blocked, sympathetic activity on the healthy side relatively increases, leading to compensatory flushing and hyperhidrosis1)6). The asymmetric findings along the midline are due to this mechanism. The possibility of reinnervation by parasympathetic nerves has also been suggested in some cases3).
Loss of sympathetic nerve function on the affected side releases inhibition of vasodilation and sweating on that side. Meanwhile, the unaffected side exhibits relative sympathetic hyperactivity, resulting in compensatory flushing and hyperhidrosis1)6). The clear left-right difference at the midline reflects this asymmetric sympathetic activity.
Tecik et al. (2025) reported performing VATS (video-assisted thoracoscopic) sympathectomy on a 43-year-old woman with idiopathic Harlequin syndrome persisting for 5 years, resulting in complete resolution of symptoms immediately after surgery with no recurrence at 4 months follow-up4). A review by Guilloton et al. found that 54.6% of cases were idiopathic4)6), suggesting the existence of a candidate group for surgical treatment.
Dalldorf et al. (2022) reported the first case of Harlequin syndrome occurring with a 5-hour delay after a T2-level erector spinae plane block (ESP block: liposomal bupivacaine 133 mg + 0.25% bupivacaine 20 mL each side)5). This is the first report of delayed onset of local anesthetic-related iatrogenic Harlequin syndrome, which typically occurs within 1 hour, and is thought to be a characteristic onset pattern of sustained-release formulations (duration approximately 72 hours). The symptoms resolved spontaneously by the next morning.
Strong et al. (2025) reported a case of secondary Harlequin syndrome (49-year-old female) due to a 62×52×32 mm multinodular goiter, in which total thyroidectomy was performed, but symptoms persisted for about 1 year postoperatively3). This finding is noteworthy as it suggests that chronic changes in the sympathetic pathway may become irreversible even after removal of a compressive lesion.